Felines (cats) are by nature carnivores and, as such, their diet reflects that. It is accepted that diet affects health, and ability to eat (or lack thereof) can have negative effects on the diet, and thus, general health. Implants have become an option for replacement of lost canines in these animals.
This allows the animal to maintain the level of mastication found in those felines who have normal oral health and permit better nutrient uptake as well as psychological maintenance of the animal. We will discuss two cases of lost maxillary canines and implant treatment to replace the lost teeth.
Case report 1
A 4.5-year-old male neutered Russian Blue cat weighing 11.5 pounds was referred for multiple bite wound evaluation and a luxated R maxillary canine tooth (#104) of three-day duration. On initial examination, there were multiple bite wounds with deep penrose drains in place, bruising and abrasions in the inguinal areas. The sites were stable. Also, the R maxillary cuspid was luxated with a slight mesial deviation, mobility and painful.
All treatment options were considered with the owner of the pet. These included: stabilization of the luxated tooth followed by endodontic treatment in two or three months; extraction of the canine and no replacement; or extraction with immediate implant placement, providing the alveolar process and vault were intact and primary stability of the implant could be attained. After discussion with the feline’s owner reviewing the pros/cons of the different treatment options, the owner chose to have the canine extracted and implant placed.
embedImagecenter("Imagecenter_1_2178",2178, "large");
The authors believe all three options have their own inherent complications. The owner did not desire having a cat without prominent anterior teeth. The owner, a well-educated engineer, analyzed all of the options and made an informed decision.
The lead author has performed numerous stabilization and endodontic treatment cases with luxated canines in dogs with relatively good results. In his experience a Figure 8 wire around the canines and use of acrylic or spot cure with some flowable composite has not been a positive experience for cats with luxated canines. They typically don’t tolerate the procedure very well. With a fracture as it presented in this case, the maxillary right cuspid (tooth #104) is not very stable and can be a challenge maintaining proper occlusion. Even with the best intentions, possible periodontal ligament devitalization and endodontic treatment being attempted in two to three months, a very good possibility of root resorption complication exists.[1] Additionally, extraction and immediate implant placement can also be problematic. But it’s less problematic than attempting to stabilize the luxated canine with subsequent endodontic treatment.
At the time surgery was performed, all past immediate implants in cats have integrated, and no integration failures have been observed during long-term follow-up on these patients. If the implants are not restored (put to sleep), the buccal osseous morphology is well-maintained, preventing a traumatic episode with the ipsilateral canine. Implant placement in these situations are becoming more predictable with happy owners and patients.[2]
Surgical phase
The patient was pre-medicated with Atropine Sulphate (1/120 grain; 1 ml/20#; subcutaneously: VetOne; Boise, Idaho) and Acepromazine (10 mg/ml; .02-.05/#; subcutaneously; VetOne). Atropine is given before anesthesia to decrease mucus secretions orally and has the added benefit of regulating heartbeat during sedation. Acepromazine is a common tranquilizer and central nervous system depressant given to pets. It is also used to prevent anxiety associated with thunder, fireworks and vet or groomer visits.
General anesthesia was induced by mask with Sevoflurane (vaporizer #7, O2 @ 4L per minute; VetOne). Oral tracheal intubation was completed and anesthesia was maintained at vaporizer setting #3, O2 1L/minute following Feline Anesthetic Protocol (FAP).
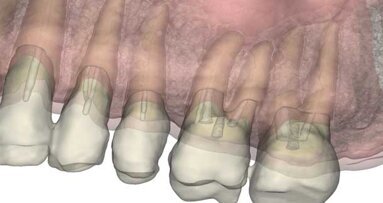
A complete oral exam and digital PA radiographs were obtained. A luxation of tooth #104 and some mobility was noted. Additionally, a widening of the periodontal ligament space with a vertical fracture of the incisive bone at the diastema of teeth #s 103/104 was observed (Fig. 1).
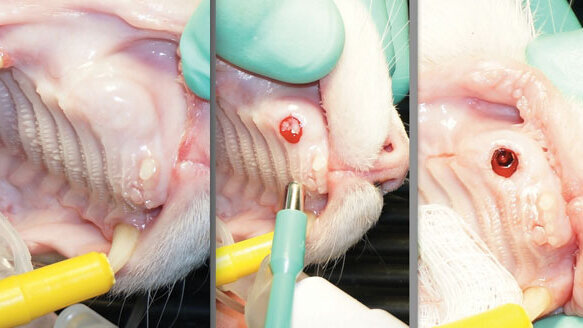
A sulcular full thickness MP flap was elevated to evaluate the alveolar process of the maxillary bone. The canine tooth (#104) was atraumatically extracted to avoid any further damage to the alveolar socket and surrounding bone. Socket debridement was performed and copious levage was complete with 0.9 percent NaCl (VetOne). The site was prepared to accept a 5.0 x10 mm Engage implant (OCO Biomedical, Albuquerque, N.M.), which was subsequently placed into the osteotomy and positioned subcrestally with a final insertion torque of 45 Ncm.
The crestal gap between the implant and socket was filled with Fusion Bone Putty (Veterinary Transplant Services (VTS), Kent, Wa.) to assist in socket regeneration and to minimize bone resorption.[3,4,5] A cover screw was placed and the flap repositioned to achieve primary closure with 5-0 resorbable monofilament sutures (Securos Surgical, Fiskdale, Mass.) (Fig. 2). Recovery was uneventful and the patient was discharged with post-surgical instructions the same day. Clavimox (62.5 mg/ml @ 1ml bid) (Zoetis, Florham Park, N.J.), a broad-spectrum antibiotic, and Buprenorphine (0.1 ml bid orally for 3-5 days) (Reckitt Benckiser Healthcare, Parsippany, N.J.), an opioid pain reliever, were dispensed to the owner.
Uncovering and restoration phase
At six months post-insertion, the patient was re-evaluated for soft-tissue healing and osseointegration. FAP was again utilized as in the surgical phase. Dental radiographs were evaluated and implant stability and integration were determined to be adequate.
A tissue punch was used to expose the implant head, preserving adequate attached gingiva on the buccal. The cover screw was removed and closed tray implant impression abutment was placed (OCO Biomedical) and a radiograph taken to verify proper mating of the impression head to the implant (Figs. 3a, 3b). Impressions were fabricated with a fast set VPS hand mix putty and a fast set light body VPS impression material (Benco Dental Supply, Tucson, Ariz.).
A transmucosal healing abutment (OCO Biomedical) was placed to insure proper emergence profile to support the future prosthetic components[6, 7] (Fig. 3c). The impression was sent to the dental lab (Doks Dental, Tucson, Ariz.), and a soft-tissue stone model was fabricated with analogs embedded within. The planned prosthetic was waxed up for a palladium implant restoration, which would be luted into the implant (Fig. 4).
At one-month post impressions, the patient returned for delivery of the implant restoration. FAP was again utilized and the prostheses was tried in and then was cemented into the integrated implant utilizing a self-adhesive resin cement (BisCem, Bisco Inc., Schaumburg, Ill.) (Fig. 5).
The 26-month follow-up demonstrated excellent emergence profile and implant stability with no evidence of periimplantitis or soft-tissue inflammation surrounding the implant restoration (Figs. 6, 7).
Case report 2
A 14.3-year-old male neutered DLH cat weighing 16.2 pounds presented for an oral examination. Generalized calculus and gingivitis was noted, as well as multiple Feline Oral Resorptive Lesions (FORL) and a complicated crown fracture of the right maxillary canine (#104).
Initial treatment options were discussed with the owner, which included scaling and root planing to treat the generalized periodontal condition and selective extractions determined by the initial probing and dental radiographs. The fractured canine treatment would be discussed after a complete oral examination and radiographs were completed under a general anesthesia. The right maxillary canine (#104) fracture appeared to have been present for a long period with some definite buccal bone changes related to the fracture.
Surgical phase
Patient was pre-medicated with Atropine Sulphate (1/120 grain; .2 ml subcutaneously) (VetOne) and Acepromazine (10 mg/ml; .05 ml subqutaneously) (VetOne). General anesthesia was induced by mask with Sevoflurane (Vaporizer #7 / O2 at 4L/minute) (VetOne). Oral tracheal intubation was completed and anesthesia was maintained at vaporizer setting #3 / O2 at 1L/minute following Feline Anesthetic Protocol (FAP).
A complete oral exam and dental radiographs were obtained. Multiple FORL were noted and charted. FORL are common in cats and are similar to cervical external resportive lesions in humans. These teeth typically have a poor prognosis and require extraction to treat them. Selective surgical extractions were successfully completed while tension-free tissue flaps were placed at the extraction sites to achieve primary closure.
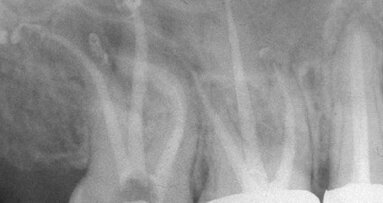
The right maxillary canine (#104) had sustained a prior traumatic fracture with pulp exposure. Definite buccal enlargement consistent with alveolar inflammation (osteitis) was present. Radiographs confirmed the diagnosis with secondary root changes evident (Fig. 8). Endodontic treatment would have been an option; however, the root morphology and sclerotic canal would be problematic.
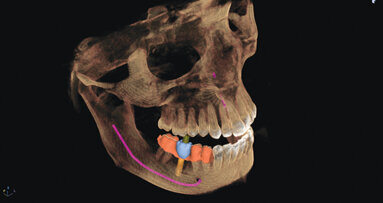
As in Case 1, the owner elected to extract the tooth and place an immediate endosseous implant, if possible, and wait four-to-six months before a final restoration could be placed. In many cases, the author is placing immediate implants with the future option of restoration utilizing digital treatment planning. Using these advanced computer-aided techniques (extra-oral scanning and CAD/CAM design and milling), final results have proven to be exceptional compared to the traditional methods of VPS impression taking and wax-cast restorations.
A coronectomy was made on the right maxillary canine (#104) for easy access of the tooth root. It is imperative to remove the remaining root while maintaining the buccal eminence. A mini envelope flap was utilized to maintain a good blood supply to the crestal bone. A fine diamond burr (#FG 703) (Benco Dental) in a high-speed water cooled drill was used to detach the periodontal ligament, making luxating and extraction a simpler process with less risk of alveolar fracture (Fig. 9a).
Examination of the socket was performed and removal of any inflammatory granulation tissue was accomplished with a curette and fissure burr. Socket measurements (probing and radiograph) were obtained and the site was prepared to accept a 5.0 x10 mm Engage implant (OCO Biomedical), which was inserted subcrestally with a final insertion torque of 50 Ncm (Figs. 9b, 9c). The crestal gaps between the implant and osteotomy were augmented with feline periomix, a DFDBA product (Veterinary Transplant Service, Kent, Wa.), which was rehydrated with 2 percent Xylocaine with 1:50.000 epinephrine (Dentsply, York, Pa.). Flap apposition was made to achieve primary closure with a combination of simple interrupted and cruciate suture patterns. Suture material was 5-0 Securocryl with a reverse cutting P3 needle (Securos Surgical, Fiskdale, Mass.) (Fig. 9d).
Recovery was uneventful, and the patient was discharged with postsurgical instructions the same day. Clavimox (62.5 mg/ml for 1 ml bid) (Zoetis) and Buprenorphine (0.1ml bid orally for 3-5 days) (Reckitt Benckiser Health Care) were dispensed.
Uncovering and restoration phase
At five-months post-implant placement, the patient returned for the start of the restorative phase (Fig 10a). FAP was administered and radiographs were obtained to verify osseous integration (Fig. 11). A tissue punch was utilized to expose the cover screw, and it was removed from the implant (Figs. 10b, 10c). It is crucial to develop and maintain healthy keratinized tissue at the healing abutment site. This KT will minimize bone resorption and inflammatory reaction around the prosthetics.6, 7 A closed tray impression coping was secured to the implant (Fig. 12, bottom), and VPS impressions were obtained. The impression coping was removed intraorally, and a healing abutment was placed (OCO Biomedical) to develop the tissue emergence profile (Fig. 12, top).
The impressions were sent to the dental lab (Precision Ceramics, Montclair, Calif.), and a soft-tissue stone model was created with the implant analogs within the model. The final restoration would be a custom anodized abutment and solid zirconia crown to be luted to the abutment. The soft-tissue model was digitally scanned and designed virtually (Fig. 13). The abutment was CAD/CAM milled, and then the zirconia crown was milled to fit the abutment (Fig. 14).
One month post-impressions, the patient again returned for delivery of the final components. Patient was anesthetized with the same protocol utilized at the prior appointments. Radiographs were obtained to verify the proper seating of the abutment into the implant (Fig. 15). After verification, the abutment screw was hand tightened and checked with the torque wrench for the manufacturer recommended 30 Ncm. The zirconia crown was cemented to the abutment utilizing BisCem (Bisco Inc.), and the prosthetics were complete.
The patient was seen for several post-operative appointments. At 7- and 10-month visits, photos demonstrate exceptional results with this paradigm shift in the treatment of non-repairable fractured maxillary cuspids in this cat (Figs. 16, 17).
Conclusion
Replacement of lost canines in felines allows the animals to maintain a better diet by helping them to better masticate food. This allows the animals to gain proper nutrients from food, which helps maximize overall health and lifespan. Additionally, as the animals are able to chew normally, the authors believe they have a better psychological well-being, leading to a happier animal and overall better quality, and ultimately, quantity of life.
Digital treatment planning has made a dramatic change in the way dental implants can be incorporated into our canine and our feline patients. This provides easier treatment by the practitioner yielding a superior product as compared to traditional methods previously utilized as discussed in Case 1. As with human patients, treatment options need to be provided with the animal’s owner making the final, informed decision on care to be rendered.
Note: This article was published in Implants, the international C.E. magazine of oral implantology, North America Edition, Issue 1, 2016. A complete list of references is available from the publisher.
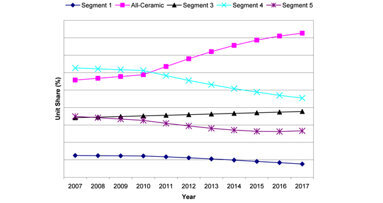
The economic recession has had a dramatic impact on the dental prosthetics industry in the United States, however the market is expected to rebound in 2012 ...
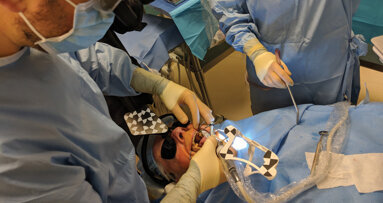
A revolution in surgical guidance is afoot. A new dynamic navigation technology called “Trace and Place” (TaP for short), was developed by ClaroNav and ...
There’s a new vision in dentistry that is gradually being recognized and is referred to as the endo-implant algorithm. This new approach considers the...
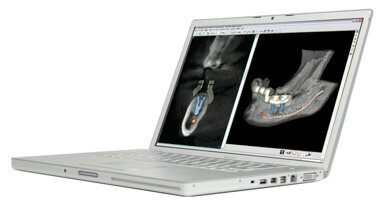
CBCT imaging has been primarily considered an integral part of the guided implant surgical process. However, with the availability of ultra-low-dose ...
NEW YORK, NY, USA: Materialise Dental has launched its latest software version: SimPlant Crystal, allowing clinicians to obtain crystal clear images from CT...
NEWPORT BEACH, Calif., USA: Glidewell Laboratories recently announced that it is now offering digital treatment planning and surgical guide fabrication to ...
In 1985, Dr. Gary Carr introduced microscopes and ultrasonic handpieces to the specialty of endodontics in an effort to improve the quality and outcomes of ...
Does rotary NiTi deserve the title of a new paradigm? The definition of “paradigm” states that it represents a new fundamental model. In the ...
NEW YORK, N.Y., USA: The Florida National Dental Convention, hosted by the Florida Dental Association, will take place June 12 to 14 at the Gaylord Palms ...
With the 1.7 version of the GALILEOS software, Sirona has succeeded in incorporating one of the key benefits of 3-D X-ray technology into GALILEOS ...
Live webinar
Wed. 3 June 2026
1:00 PM EST (New York)
Live webinar
Thu. 4 June 2026
2:00 PM EST (New York)
Live webinar
Mon. 8 June 2026
12:00 PM EST (New York)
Live webinar
Mon. 8 June 2026
1:00 PM EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 PM EST (New York)
Live webinar
Wed. 10 June 2026
11:00 AM EST (New York)
Live webinar
Wed. 10 June 2026
2:00 PM EST (New York)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East















































To post a reply please login or register