There’s a new vision in dentistry that is gradually being recognized and is referred to as the endo-implant algorithm. This new approach considers the role of the endodontist as critical in considering whether a tooth can be saved or whether extraction and replacement with a dental implant is the correct treatment protocol.
An endodontist is in the unique position to evaluate critical factors leading to endodontic failures in order to determine whether another endodontic procedure will lead to a predictable and successful outcome. Should the outcome not be favorable, then extraction and replacement with a dental implant would be the protocol to follow.
In considering the ideal treatment plan, it is imperative to provide the patient with all treatment options, as well as the financial cost and procedures associated with each treatment option. The patient is thus given the opportunity to make an educated decision as to the best treatment protocol for him or her. The information presented to the patient should include the endodontist’s opinion regarding which treatment option is more practical and predictable.
Case study
A patient with a non-contributory medical history was referred to my office for evaluation of the maxillary left first molar. The patient was asymptomatic, and the tooth had been endodontically treated by a general dentist approximately seven months prior to the consultation and had never been restored.
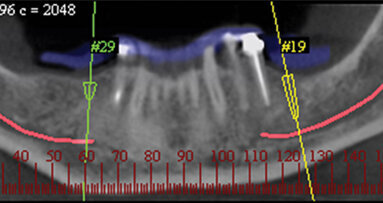
Clinically, it presented extensive decay, probing depths of 3 mm all around, exposure of the obturation material to the oral cavity and no temporary restoration. Radiographically, no periapical lesions were detected, and the bone levels around the tooth were adequate (Fig. 1).
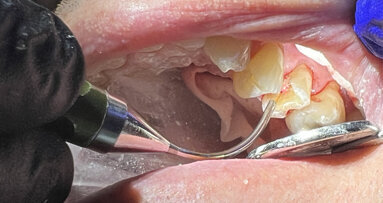
In order to determine the integrity of the tooth structure, some excavation was performed using 4.5x magnification and supplementary illumination, provided by a fiber-optic headlight, with a dental rubber dam for isolation. After the removal of some decay, a bitewing X-ray was taken (Fig. 2) and the -following was determined:
a) the floor of the pulp chamber was too shallow;
b) it was too close to perforation and
c) the peri-radicular dentine was insufficiently strong to support a permanent restoration.
These critical factors, in my opinion, rendered the tooth non-restorable. A cotton pellet and Cavit were placed in the access cavity and a follow-up call with the referring dentist was conducted in order to -update him on the condition of his patient and to determine what recommendations should be given regarding the tooth.
It was recommended to the patient that the tooth be extracted and the socket preserved through a minor grafting procedure.
This would allow for an ideal amount of bone to receive a dental implant approximately four to six months later.
It was also recommended that he receive some orthodontic treatment prior to the placement of the implant so that all the diastemas would be closed and the dentition properly aligned for this procedure.
The patient clearly understood the concept and the logistics of the orthodontic treatment recommended but expressed no interest in this approach.
The bigger picture
It is very important in evaluating treatment using implants to consider the entire dentition and not just the space or tooth in question.
It should be borne in mind that implants, unlike teeth, do not move, so if there are any misalignments in the dentition, orthodontic treatment prior to implant therapy is imperative should the patient proceed with the dental implant at a later stage. If the treatment plan is not in this sequence, the dental implant could become a challenging obstacle during the orthodontic treatment.
The patient was prescribed Amoxicillin 500 mg (one every six hours, beginning two days before the next appointment) and chlorhexidine rinses (three times a day, also beginning two days before the next appointment). The use of tartar-control toothpaste was also recommended in order to avoid staining of teeth. On the day of surgery, the patient’s blood pressure was 119/73 with a heart rate of 76.
Under local anesthetic (Lidocaine 2 percent HCl with epinephrine 1/50,000 x 2 cpl) and using a dental rubber dam, magnification loupes and supplementary illumination, the tooth was sectioned into three pieces. The rubber dam was removed, and using PDL-Evator elevators (Salvin), all three roots were extracted without any complications. Spoons were used to curette the socket in order to clean any granulation tissue and engage the cancellous bone.
This crucial step results in some bleeding and thus promotes angiogenesis. The crest of the interradicular bone was engaged with the socket cupped part of a XiVE osteotome (DENTSPLY Friadent), and a sinus lift was performed using the Summer’s technique.
There were no signs of a sinus perforation based on the Valsalva test. The sockets and sinus-lift area were then grafted with a mixture of DBX and MCP using a marshmallow technique.
This grafting mixture helps the site produce its own bone in terms of mineral and collagen from the DBX, and it provides a better scaffold effect from the MCP. The area was covered with a PTFE membrane, slightly tucked under the periosteum (not more than 2 mm). Sutures were done with polyglycolic acid using a criss-cross four-x corner technique (Fig. 3).
Removing the sutures
The sutures were removed two weeks later. Two weeks after suture removal, the patient was seen again for the removal of the membrane.
This was done by gently picking at the membrane with cotton pliers and exerting pull on it — there is often no need for anesthesia.
The benefit of using this allograft cocktail is that the waiting period for re-entry was approximately four to six months versus six to nine had a xenograft been used. The quantity and the quality of the bone appeared to be much better with the use of this allograft cocktail.
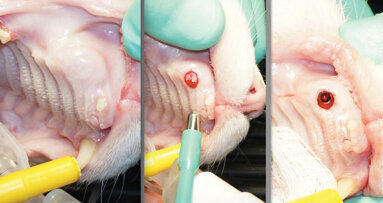
At the time of re-entry, the patient’s blood pressure was 113/69 with a heart rate of 64 (Figs. 4, 5). Under local anesthetic (Lidocaine 2 percent HCl with epinephrine 1/50,000 x 2 cpl), a tissue punch access was done using a 3.8 tissue punch XiVE drill (DENTSPLY Friadent).
The pilot drill from the ANKYLOS implant system (DENTSPLY Friadent) was then used to drill 6 mm, just short of the sinus floor (Fig. 6). A series of XiVE osteotomes, from size 2.0 up to 3.4, were used to perform a sinus lift using the Summer’s technique. The osteotomy was prepared to a depth of 11 mm (Fig. 7).
A Valsalva test was performed to ensure that the sinus had not been perforated. An ANKYLOS implant A11 (3.5 mm x 11 mm) was placed and primary stability was obtained.
The density of the bone perceived as D-3 during the drilling stage likely changed to D-2 with the use of the osteotomes.
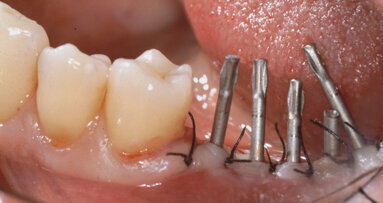
The implant-transfer mount was removed, as was the cover screw that came pre-mounted inside the implant, and a 1.5 mm sulcus former (healing abutment) was placed into the implant (Figs. 8, 9).
This case clearly demonstrates one of the reasons endodontists are becoming increasingly involved in implant dentistry. They are able to provide a comprehensive evaluation of the tooth in question, and they are able to present the patient with the best options based on clinical assessment.
embedImagecenter("Imagecenter109",109);
Dr Jose M. Hoyo may be contacted at drjhoyo@aol.com.
Privacy is something we all value. It should not come as a surprise to anyone that dental patients want to ensure more than ever that their personal ...
NEW YORK, N.Y., USA: The Florida National Dental Convention, hosted by the Florida Dental Association, will take place June 12 to 14 at the Gaylord Palms ...
NEWPORT BEACH, Calif., USA: Glidewell Laboratories recently announced that it is now offering digital treatment planning and surgical guide fabrication to ...
Felines (cats) are by nature carnivores and, as such, their diet reflects that. It is accepted that diet affects health, and ability to eat (or lack ...
Already in 2005, a report from Kalorama Information1 estimated that the growth in implant-based dental reconstruction products would outstrip other areas of...
For years the term “orthodontics” conjured images of metal wires, painful brackets and middle school chants of “brace face,” all of ...
The passive utilization and micro-volume management of sodium hypochlorite as an endodontic irrigant has been illustrated with a laboratory demonstration ...
Pulpal exposures are unfortunately a routine occurrence when treating carious teeth and frequently lead to endodontic treatment owing to the size of the ...
Samuel O. Dorn, DDS, received the American Association of Endodontists’ highest honor, the Edgar D. Coolidge Award, given for leadership and exemplary...
The needle implants were designed and presented in the early 1960s by the French dentist Scialom. He understood that, using biomechanical properties related...
Live webinar
Wed. 3 June 2026
1:00 PM EST (New York)
Live webinar
Thu. 4 June 2026
2:00 PM EST (New York)
Live webinar
Mon. 8 June 2026
12:00 PM EST (New York)
Live webinar
Mon. 8 June 2026
1:00 PM EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 PM EST (New York)
Live webinar
Wed. 10 June 2026
11:00 AM EST (New York)
Live webinar
Wed. 10 June 2026
2:00 PM EST (New York)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East
















































To post a reply please login or register