In Part 1 of this three-part series, we presented a sinus lift technique involving hydraulic pressure to elevate the floor of the maxillary sinus. Many respected clinicians and researchers have taken the task to compare the effects as it is related to a percentage of sinus perforation using existent intracrestal sinus lift techniques.
These proven surgical techniques include the use of osteotomes (Summers — and its multiple variations), balloon lift, hydraulic sinus condensing technique (Chen and Cha) and motor-driven drilling systems.
Scientific articles published in 2012 by Loma Linda School of Dentistry (Garbacea and Lozada ) and the Department of Periodontics and Oral Medicine, University of Michigan School Dentistry (Chan and Avila), assessed crestal sinus floor elevation using cadaver heads and endoscopes to study the incidence of maxillary perforations. Both studies concluded that perforations can occur with any technique but are more likely to happen when the membrane is raised past the 10-mm mark measured from alveolar crest. A recent prospective study published in 2012 by the Division of Prosthetic Dentistry, Maxillofacial Unit in Sweden (Fornell and Johansson) presented a CBCT-guided osteotome sinus elevation technique that shows improvement over conventional techniques in that there is decrease in the percentage of perforations.
embedImagecenter("Imagecenter_1_743",743, "large");
The purpose of this article is to introduce a surgical technique that combines planning and drilling using CAD/CAM surgical guides with hydraulic intracrestal approach sinus lift. This technique is a combination of creative thinking from the authors and innovative instrumentation developed by Hiossen Implant Systems.
Four patients were treated using this technique; 20 taper-hydrophilic implants (Hiossen ET-III) were inserted and integrated over a period of six months. Two patients were partially edentulous and two were fully edentulous. A total of 12 fixtures were placed on sound residual anatomical bone and eight were placed on atrophic ridges (Misch classification SA3). The diameter of the fixtures in areas were sinus was lifted were 5 mm, and the length varied from 8.5 to 10 mm. This technique is indicated when treating patients with maxillary ridges with classification SA3 following Misch protocols for patients with 5 to 8 mm or Mongalo classification #B for ridges with 4 to 7 mm of anatomical residual ridges.
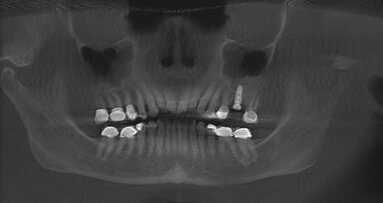
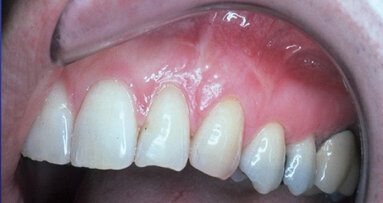
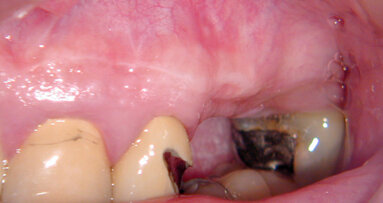
Patient No. 1 is a 55-year-old female missing posterior dentition. This case was selected to illustrate the technique, because it resembles cases that are commonly encountered in general-practitioner offices. The first step was to fabricate an all-acrylic partial with gutta-percha markers to be used as scanning prosthesis; the idea is to always keep in mind that surgeries should be guided with final prosthetics in mind (Fig. 1). The images from CBCT were converted into 3-D working models, and surgical plans (Fig. 2) were used to design and order CAD surgical guides (Fig. 3). Anterior implants not needing sinus lift were placed with the guide following flapless proven protocols (Fig. 4), and the guide was used to drill on the posterior site were lift was necessary by allowing the drills to be short 1 mm to the sinus floor (Fig. 5).
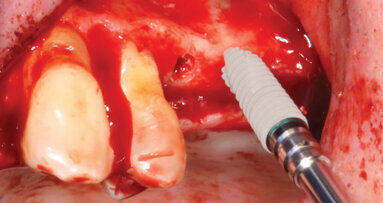
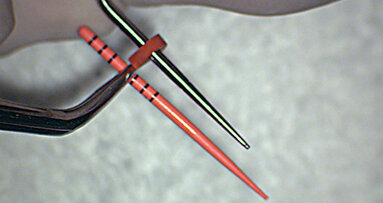
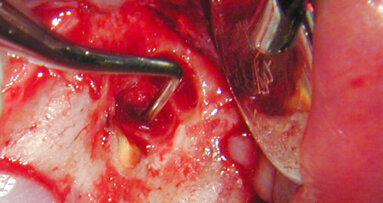
The floor of the sinus was imploded using non-cutting end drills (CAS) (Fig. 6). Three cc of saline was used to create hydraulic pressure and elevate the membrane (Fig. 7). One gram of non-ceramic synthetic bioactive crystals (Ossteogen by Implandent) was packed per implant site and fixtures were inserted at 20-30 Newtoms (Fig. 8).
All patients were scanned postoperatively to verify 360 degrees of bone spread surrounding the implant and to ascertain that sinus membrane was not perforated. Three-dimensional images revealed no perforation and excellent distribution of the synthetic bioactive material surrounding the implants placed.
Six months were allowed for bone remodeling and ossoeintegration. While this prospective study represents a very small number of cases to come to any kind of scientific conclusions, we are excited with the prospect of being able to introduce a technique that might reduce the percentage of perforations as a consequence of intracrestal sinus lifts.
Note: This article was published in Dental Tribune U.S., Vol. 8, No. 2, February 2013 issue.
In 1974 Dr. Hilt Tatum Jr. performed the first sinus lift in the world. His technique became known as the “lateral window” approach and has been...
When Dr. O. Hilt Tatum performed his sinus lift technique in 1975, I wonder if he had any idea of how it would evolve or the controversies that would ...
NEW YORK, N.Y., USA: For a successful dental implant, the first step for some patients is reconstructive surgery of the jaw. A bone graft to augment the ...
I invented the Continuous Wave of Obturation Technique (CWOT) in 1986 and used it with the Touch’n Heat (SybronEndo) until the winter season of ...
In today’s new information age, patients want a better quality of life. They want to keep their youthful, brighter-appearing smile more than ever; keep ...
In the ever-evolving landscape of dentistry, staying ahead requires embracing innovative technologies that enhance patient care and elevate practice ...
NEW YORK, N.Y., USA: Researchers at the New York University College of Dentistry (NYUCD) recently surveyed otolaryngologists from New York state to help ...
All steps have been meticulously followed, the REF has been placed, the crypt has refilled nicely, the final radiograph has been approved, and it is time to...
In Parts 1 through 4, the necessary steps and procedures were presented, enabling the operator to atraumatically and predictably allow the root-end ...
During the 1960s, when the Begg lightwire and the Tweed edgewise were the mainstream techniques of orthodontic therapy, Dr. Maxwell Fogel and Dr. Jack ...
Live webinar
Tue. 5 May 2026
3:00 PM EST (New York)
Live webinar
Wed. 6 May 2026
1:00 PM EST (New York)
Live webinar
Wed. 6 May 2026
8:00 PM EST (New York)
Ms. Ellen Karlin, Dr. Sara Karlin
Live webinar
Thu. 7 May 2026
11:00 AM EST (New York)
Live webinar
Thu. 7 May 2026
12:00 PM EST (New York)
Live webinar
Thu. 7 May 2026
12:00 PM EST (New York)
Dra. Maria Carolina Erhardt, Dra. Thais Tomé Feldens
Live webinar
Thu. 7 May 2026
2:30 PM EST (New York)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East



















































To post a reply please login or register