All steps have been meticulously followed, the REF has been placed, the crypt has refilled nicely, the final radiograph has been approved, and it is time to suture the flap into position. Sadly, most operators now push the microscope aside and suture without it. To do this robs the operators of an opportunity to demonstrate to themselves and their patients the amazing capabilities of the OM.
The doctors must make a commitment to master the suturing technique using the OM.
It will never be accomplished with the OM pushed aside at this critical step in the apical microsurgical procedure. The following will be based largely on the author’s own experiences during nearly 20 years of doing, teaching and writing about apical microsurgery.
Dr. John Harrison has published some of the most clearly written and comprehensive work on wound healing associated with periapical surgery.
There are five publications that are a “must read” for the endodontic surgeon. These publications can be found in the Journal of Endodontics: 1991, Vol. 17, pp. 401-408, 425-435, 544-552; 1992, Vol. 18, pp. 76-81; and 1993, Vol. 19, pp. 339-347.
After reading these articles, the microsurgical protocol developed by Drs. Gary Carr, Richard Rubinstein and others becomes clearer and is more easily understood. The word “atraumatic” is an important factor to achieve predictable wound healing.
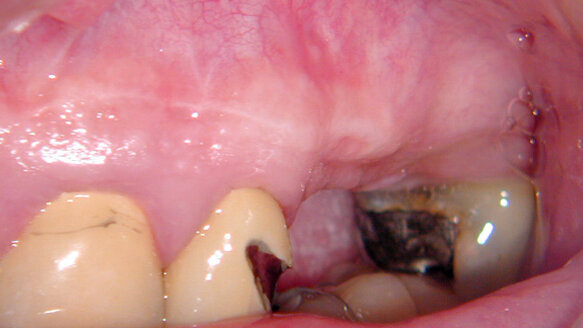
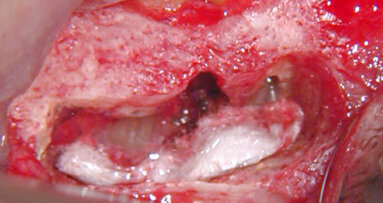
When the surgical site is ready for closure, the flap should be gently massaged to close approximation with the attached tissue. But, keep in mind, the flap has probably lost dimension, or “shrunk” slightly, due to the mere act of retraction over a period of time and has endured a slight decrease of blood flow to it. Fortunately, this is usually not a problem. If the initial incision was planned with this final step in mind, the tissues should re-approximate with minimal manipulation. Now is when the operator will appreciate nice “scalloping” and a sharp scalpel when making the incision in the beginning of the surgery (Fig. 1).
Remember the old saying, “Hindsight is always 20/20”? The smooth side of a small #2 mouth mirror can be used to hold the tissue in position while the second surgical assistant (on the same side of the chair as the doctor) hands the doctor the needle holder with the needle positioned properly in the beaks so the sutures can be easily and accurately placed.
All suturing is accomplished using 6-0 black monofilament nylon (Supramid, S. Jackson). Some microsurgeons are using 8-0 and, even 10-0 sutures; but the 6-0 is easy to use, doesn’t tear through the tissue as readily and the results are no different than with the more technique-demanding, thinner sutures. Keep in mind, the sutures will be removed in 24 hours so it is really a moot point as to whether the suture is 6-0, 8-0 or 10-0.
The results achieved with 6-0 suture seem to be well suited to apical microsurgery. The black silk suture, traditionally used in surgery, is a detriment to the rapid healing we are trying to achieve. Not only does bacterial plaque more readily accumulate on it than monofilament but, also, the braiding acts as a wick for the migration of bacteria into the wound. This can result in an increased inflammatory response and compromised healing.
The type of needle used depends on the type of flap to be sutured. For the Oshenbein-Leubke Flap, a taper point needle (TPN), 3/8 circle (Supramid, S. Jackson, code MEA-60B) is used.
The TPN is far superior to the reverse cutting type needle (RCN) because there isn’t the tendency to cut, or tear, the flap edges. Also, the TPN require less effort to exit at a point in the attached tissue where the operator intends, not where the needle wants to exit.
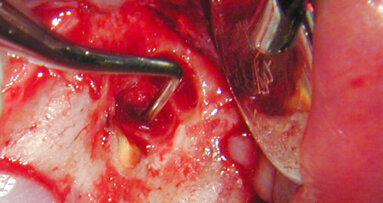
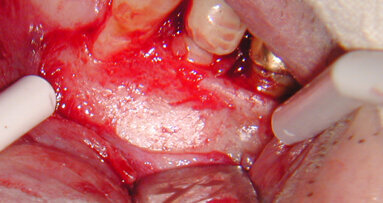
In other words, it is easier to guide a TPN to the desired point of exit in the attached tissue than it is a RCN. They just seem to cooperate more when suturing this type of flap! One of the nicest things about using this flap design is the ability to easily see the healing taking place (Figs. 2–6)
For the Sulcular Flap, a reverse cutting needle (RCN), 3/8 circle (Supramid, S. Jackson, code MPR-60B) is used. This needle is used because the larger size facilitates passing it through the contacts when doing a sling suture. The sling, or mattress type, suture is routinely used to save time on closure, rather than doing individual buccal to lingual sutures. On many occasions, the TPN (see above paragraph) is also used to suture the attached gingival area of the flap at the coronal aspect of the releasing incision.
A technique for suturing using the SOM: While the scope assistant holds the retractor in place, the second assistant uses a small Castro-Viejo type needle holder. The beaks of the holder must grasp the needle approximately 3/4 of the distance from the pointed end to where the suture is attached to the needle. Special attention, by the second assistant, must be taken to keep the beaks of the holder away from either end of the needle, as these are the areas of the needle’s greatest weakness and can be inadvertently bent or broken (Fig. 7).
Care is taken so the needle is firmly grasped perpendicular to the beaks of the holder. This allows the operator more definite control and a better “feel” of the needle during the suturing process.
The second assistant now passes the needle holder into the doctor’s normal working hand (Hand A). The doctor then begins the suturing process by inserting the needle through both sides of the incision. When the needle is completely through both sides of the incision, the needle is then grasped between the thumb and index finger of the opposite hand (Hand B).
While the doctor is doing this, the second assistant is holding the end of the suture so it won’t inadvertently be pulled through the tissues. The doctor proceeds to make the three loose “loops” around the beaks of the needle holder to start the first knot.
While the doctor is making these initial “loops,” the second surgical assistant is placing the end of the suture into the doctor’s visual field of the microscope, so the end of the suture can be easily grasped in the beaks of the needle holder by the doctor.
The second assistant can be sure the end of the suture is within the doctor’s field of vision by looking into a monitor that has been placed so it is easily seen (Fig. 8).
The “loops” around the beaks of the needle holder create enough friction so there is a controllable tension between the doctor’s Hand B and the beaks of the needle holder in Hand A. Care must always be taken that the tension is only between Hand B and the needle holder in Hand A, so no undesirable tension is exerted on the tissue during the suturing process.
The purpose of maintaining some tension is to give the doctor a positive tactile sense while taking up the excess suture material in Hand B. As the suture is drawn through the tissue by Hand B, Hand A is lowered to prevent exerting too much tension on the tissue.
The tension on the suture is regulated by the looseness, or tightness, of the “loops” which control the amount of friction for the suture to overcome as it is gathered. Hand B continues gathering as Hand A yields the suture with a “descending” motion while still maintaining the desired tension, and the beaks of the holder have the end of the suture firmly secured.
When the end of the suture is at the desired length relative to the incision, the “loops” are allowed to slip off the beaks for the initial knot. Then, using the same basic rhythm of movements, the “securing” and “locking” knots are placed. It is an alternating rhythm of movement that is difficult to describe in writing, but is actually very easy for the beginning microsurgeon to learn.
The doctor now allows the second surgical assistant to take the needle holder from Hand A and simultaneously be handed the micro-scissors so the suture can be cut close to the knot.
After the second assistant takes the scissors and the suture, the doctor is handed a micro-forceps to gently move the knot between the point of insertion and the incision, helping to prevent plaque build-up over the incision itself (Fig. 9).
Note: When moving the knot with the micro-forceps, it is important that the knot be “pushed” to place, not “pulled” to place. This ensures the suture’s original tension and integrity is maintained.
One of the most common mistakes made when suturing is to make the suture too tight. It is better to make the suture a little too loose than to make it too tight. When the suture is too tight, it causes ischemia and thus compromises rapid healing. When making a sling suture in a sulcular flap, it is easy to be too aggressive when tying the knot, causing the rest of the suture to get too tight. The doctor should always recheck the tension over the entire length of the suture before completing the securing knots.
The releasing incision is usually an integral part of every flap and is considered differently from the rest of the incision. Normally, the releasing incision is not sutured, but if it is, the suture should be looser than the other sutures. It has been shown that epithelial creep, or streaming, occurs rapidly, or at a rate of about
1 mm per side per 24 hours.
In other words, a wound whose edges were separated 2 mm would be expected to come together within a 24-hour period. In hundreds of surgeries during the past 12 years, there were only a few cases where the releasing incision wasn’t completely closed.
Of those few that didn’t close within 24 hours, they all closed within 48 hours. To repeat: If the operator prefers to suture the releasing incision, it must be sutured loosely (Fig. 10). Another consideration is to be sure to suture “like tissues to like tissues.” Never suture attached gingival tissue to unattached gingival tissue. If one side of the suture “tears out,” it will be the attached gingival side.
When using the OM to suture, the incision can be closed accurately with extremely good approximation. It is because of well-planned and nicely scalloped incisions; atraumatic flap elevation procedures; and the very close repositioning of the flap with thin, hair-like sutures (6-O) that we can plan on routinely removing sutures in 24 hours (see Figs. 6 and 7).
The sutures have completed their task after 24 hours, and in fact, have now become foreign bodies that can cause irritation, excessive inflammation, be a source of infection and, ultimately, result in a retardation of the healing process.6
For those who doubt the 24-hour Suture Removal Theory, an easy exercise is this:
- At the next surgery, be sure to place at least five sutures.
- After 24 hours, have the patient come in and remove the worst-looking suture, the one you think isn’t healing as well as the others.
- Then, the next day, remove the next worst-looking suture.
- The next day, do the same, and so on. At the end of the fifth day, the worst-looking suture will be the one remaining! If that doesn’t convince you, nothing will.
Post-operatively, the usual result is little, or no, pain or swelling. The post-operative instructions are ice packs 15 minutes on and then 15 minutes off for the first six hours only, gentle rinsing with Peridex for the next 24 hours, and have sutures removed the next day. Experience has demonstrated that prescribing Ibuprofen 600mg every six hours, along with 1-2 tabs of Tylenol OTC (taken between the doses of Ibuprofen), has a very effective anti-inflammatory effect.
It is the exception, rather than the rule, that a patient requires a stronger medication for post operative pain. Antibiotics are not usually prescribed.
If everything is within normal limits, the patient is instructed to begin gentle cleaning of the area on the third day post-op, using a wash cloth over his or her index finger, and to begin gentle brushing, with a soft brush, on day five. The patient is scheduled for a follow-up visit two weeks after surgery.
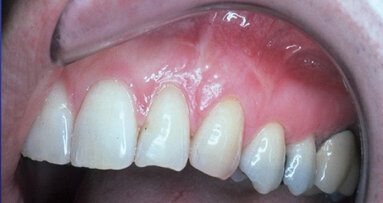
At the two-week visit, normally the incision is barely visible, and on most occasions, can hardly be detected.
A word of caution: Not all patients respond to treatment as well as others. Don’t be in a hurry to treat a problem that may not exist. On a few occasions, patients may be slower than normal in response to treatment, sometimes taking several weeks to heal as well as other patients have or do in just days.
If there is any doubt, place the patient on antibiotics and an anti-inflammatory for a week as a precaution, but what is really desired is more time for delayed healing to occur.
The apical microsurgical technique described in the previous six parts has become the standard of care in endodontic treatment and raises endodontic apical surgery to a new and exciting level.
For the first time, apical surgery can be performed with predictable results. But these results can only be achieved if the proper protocol is followed meticulously.
The steps must be followed without compromise. Much more could be written, but hopefully enough of an overview has been given to stimulate just one more doctor to begin using the OM. It is the finest tool our profession has ever been given.
Apical microsurgery can be an enjoyable part of the daily regimen, for both the doctor and the newly involved dental team!
embedImagecenter("Imagecenter_1_179",179, "large");
About the author
Dr. John J. Stropko received his DDS from Indiana University in 1964, and he practiced restorative dentistry for 24 years. In 1989, he received a certificate for endodontics from Boston University and recently retired from the private practice of endodontics in Scottsdale, Ariz.
Stropko is an internationally recognized authority on micro-
endodontics. He is the inventor of the Stropko Irrigator, has published in several journals and textbooks and is an internationally known speaker. He is the co-founder of Clinical Endodontic Seminars and and was an instructor of microsurgery for the endodontic courses presented at the Scottsdale Center for Dentistry. Stropko and his wife, Barbara, currently reside in Prescott, Ariz. You may contact him at topendo@aol.com.
References
1. Craig KR, Harrison JW. Wound healing following demineralization of resected root ends in periradicular surgery. J Endod 1993 Jul; 19(7): 339-47.
2. Martell B, Chandler NP. Electrical and dye leakage comparison of three root-end filling materials. Quintessence Int 2002 Jan; 33(1): 30-4.
3. Aqrabawi J. Sealing ability of amalgam, super EBA cement, and MTA when used as retrograde filling materials. Br Dent J 2000 Mar 11; 188(5): 266-8.
4. Rubinstein RA, Kim S. Long-term follow-up of cases considered healed one year after apical microsurgery. J Endod 2002 May; 28(5): 378-83.
5. Dragoo MR. Resin-ionomer and hybrid-ionomer cements: Part I. Comparison of three materials for the treatment of subgingival root lesions. Int J Periodontics Restorative Dent 1996 Dec; 16(6): 594-601.
6. Harrison JW, Gutmann JL. Surgical Endodontics. Blackwell Scientific Publications 1991; 278-331.
In Parts 1 through 4, the necessary steps and procedures were presented, enabling the operator to atraumatically and predictably allow the root-end ...
Surgery will never replace solid endodontic principles and should always be a last resort. Apical microsurgery consists of nine basic steps that must be ...
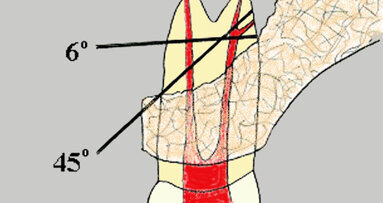
The amount, or degree, of the root-end bevel (REB) is of utmost importance and should be precisely planned in advance after considering the overall ...
In Parts 1 and 2, I discussed the preparation of the patient, the incision and atraumatic flap elevation. These are the first three steps necessary to ...
Using a disposable CK2 microsurgical blade (SybronEndo), the incision is made. With the smaller size of this blade, very accurate incisions can be made that...
In today’s new information age, patients want a better quality of life. They want to keep their youthful, brighter-appearing smile more than ever; keep ...
In Part 1 of this three-part series, we presented a sinus lift technique involving hydraulic pressure to elevate the floor of the maxillary sinus. Many ...
LUBBOCK, Texas, USA: Osteogenics Biomedical, a leader in the development of innovative dental bone grafting products, has announced the acquisition of ...
NEW ORLEANS, La., USA: In what will certainly be considered a highlight of AAE17, two live endodontic microsurgeries — one mandibular, one maxillary ...
In 1974 Dr. Hilt Tatum Jr. performed the first sinus lift in the world. His technique became known as the “lateral window” approach and has been...
Live webinar
Wed. 27 May 2026
8:00 AM EST (New York)
Live webinar
Thu. 28 May 2026
12:00 PM EST (New York)
Live webinar
Mon. 1 June 2026
1:00 PM EST (New York)
Live webinar
Wed. 3 June 2026
1:00 PM EST (New York)
Live webinar
Thu. 4 June 2026
2:00 PM EST (New York)
Live webinar
Mon. 8 June 2026
12:00 PM EST (New York)
Live webinar
Mon. 8 June 2026
1:00 PM EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East















































To post a reply please login or register