Biomimetic dentistry is based on the philosophy that the intact tooth in its ideal hues and shades and, more importantly, its intracoronal anatomy, mechanics and location in the arch, is the guide to reconstruction and the determinant of success. This approach is conservative and biologically sound and in sharp contrast to the porcelain-fused-to-metal technique in which the metal casting with its high elastic modulus makes the underlying dentin hypofunctional.
embedImagecenter("Imagecenter_1_361",361, "large");
The goal of biomimetics in restorative dentistry is to return all of the prepared dental tissues to full function by the creation of a hard-tissue bond that allows functional stresses to pass through the tooth, drawing the entire crown into the final functional biologic and esthetic result.[1]
According to Douglas A. Terry, DDS, in dentistry there is no one biomaterial that has the same physical, mechanical and optical properties as tooth structure (i.e., dentin, enamel, cementum) and possesses the physiological characteristics of intact teeth in function. By utilizing biomimetic therapeutic approaches, dentists can improve and become closer to natural biological structures and their function.[8]
There are two major perspectives to which the term “biomimetic” is applied: a purist perspective that focuses on recreating biological tissues and a descriptive perspective that focuses on using materials that result in a mimicked biological effect.[8] Although different, both share a common goal of mimicking biology in restoration.[8] This has been an increasingly common goal for dentists and patients alike in achieving esthetic and functional dentistry.
Biomimetic dentistry techniques provide the patient with minimally invasive options that conserve sound tooth structure as a clinical imperative.[2] Biomimetics is essentially described as a mimicking of natural life, which can be accomplished using contemporary composite resins and adhesive dental procedures.[2] Conservation and biological mimicry make up the foundation of a biomimetic philosophy and together produce the effect that today’s patients expect.
From an esthetic/restorative perspective, biomimetics or biomimicry is the application of methods and systems to artificially replace biologic elements in order to recreate optimal oral health.[8]
Practicing interdisciplinary esthetic restorative dentistry enables dentists to achieve biomimetic results with cosmetic dentistry.[8] These techniques and materials are crucial to modern dentistry in that they combine a focus on dental health and appearance. A biomimetic material should match the part of the tooth that it’s replacing in several important ways, including the modulus of elasticity and function of the respective areas (e.g., pulp, dentin, enamel, dentoenamel junction).[8]
The production of bone-, dentine- and enamel-like biomaterials for the engineering of mineralized (hard) tissues is a high priority in regenerative medicine and dentistry.[10] The ability to manufacture such materials has allowed dental restorations to attain significantly more nature-like results that inevitably perform at a higher level than less life-like materials of the past.
The physiological performance of an intact tooth requires a balance between biological, mechanical, functional and esthetic parameters in order to achieve biomimetic qualities.
This necessitates the development of “anatomical morphological thinking” when developing a restoration so that it replicates the natural tooth in form, function and esthetics.[8] Such biological thinking will enable dentistry to focus on future health as well as the lasting appearance of the patients’ smiles, both of which are necessary for patient satisfaction.
According to Wynn Okuda, DMD, “modifications to existing cavity design should be based on preservation of natural dentition. The goals and objectives of biomimetic replacement should be to mimic the structure being replaced, thus allowing minimal removal of non-affected adjacent tooth structure.”[8] Incorporating biomimetic principles stems from somewhat of a philosophical approach to practicing dentistry, Okuda says.[8] Dentists must take time to research methods of minimally invasive approaches to solving dental problems.[8]
Over billions of years, nature has created a formula for highly functioning materials that have withstood evolution. To create structures that will continue to function at such a level, dentistry must copy and integrate nature’s complex methods. Terry states that “we need to develop treatment modalities that allow us to reproduce the biomechanical behaviors of the intact tooth. As research scientists, clinicians and technicians work together in understanding the complex orientation of this composite material called tooth structure, improvements will continue.”[12]
The same philosophy of using nature as a guide for restoration and regeneration can be extended to a functional solution creating missing structures in cosmetically focused patients.
Minimally invasive treatments are procedures that restore form, function and esthetics with minimal removal of sound tooth structure.[3] This is accomplished by removing only dental tissues that cannot be adhesively bonded.[9] This conservative approach leaves patients with as much of their natural tooth structure as possible while restoring or creating tissue that will enhance utility and appearance.
While indirect porcelain veneers can require a great amount of preparation and removal of tooth structure, direct composite bonding follows the conservative approach. Direct resin composite restorations offer an alternative treatment that provides excellent esthetics and preservation of tooth structure given that the preparation is limited to only areas of affected unsupported enamel.[23]
Patients today want their dentistry more esthetic but less invasive and composite resin accomplishes both.[11] Evidence suggests that composites can provide optimal esthetics with minimal or no tooth intervention, immediately improving esthetics while leaving options for future orthodontic and restorative care.[13] Furthermore, as a person ages, so do their restorations.
Eventually, teeth that have been restored will break down and need to have those restorations replaced.[4] Fortunately, if an initial restoration was created using minimally invasive procedures, there should be more tooth structure to work with at the time when a second restoration may be needed.[2]
In this way, the biomimetic approach takes into account both the present and future dental health of the patient.
Nowadays, there are many modern composite resins developed for highly esthetic procedures that, when properly used, can result in restorations that are indistinguishable from natural dentition.[24] This article extrapolates the minimally invasive biomimetic principles of restoration and applies them to procedures for introducing missing tissue and creating cosmetic improvements, which ultimately benefit the patient’s overall oral health and appearance.
The process of mimicking tissue that was not initially present uses biomimetic methodology similar to that used in restorative dentistry that conserves tooth structure. Two cases will be presented that demonstrate the diversity of options biomimetic techniques provide for the field of cosmetic dentistry.
Case No. 1
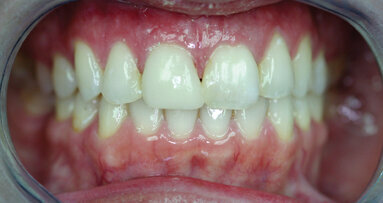
A 34-year-old, healthy male presented for treatment of the spacing between his upper and lower anterior teeth as well as whitening. He desired a more esthetic appearance overall. After an examination, the patient was presented with two options. Both porcelain veneers and biomimetic composite bonding would eliminate spacing and create a whiter smile, though the composite bonding technique demonstrated several advantages that made it the right choice for the patient.
The biomimetic effect of composite bonding ensures that the patient will attain a natural and highly functional result. Today’s composites have much improved physical and esthetic properties, enabling minimally invasive treatment modalities to be performed with immediate results that are able to satisfy the most cosmetically discerning patients.[14–19]
Porcelain veneers, on the other hand, require greater and irreversible tooth intervention. In addition, they would require at least two appointments and somewhat considerable tooth preparation.[13] The composite bonding chosen for this patient involves minimal intra-enamel preparation from sand-blasting or cleaning the enamel surface with pumice and no local anesthetic.[13]
With this type of treatment, fewer teeth (or just parts of teeth) can be treated and, becuase there is no laboratory fee, there is less cost for the patient.[22] Composite bonding can be considered as a viable minimal or non-invasive treatment alternative.[20, 21]
Treatment
An initial in-office whitening procedure was accomplished one week before the composite fill restoration. Treatment for general upper and lower diastemas was then carried out and consisted of the following: the maxillary anterior teeth and mandibular anterior teeth were pumiced with Pumice Preppies (Whip Mix Corp.), rinsed and dried.
The teeth were then treated with Ultra Etch 35 percent phosphoric acid (Ultradent Products) for 15 seconds, rinsed and left moist. Bonding agent Prime & Bond NT (Dentsply Corp.) was applied to the teeth, air thinned and then light cured for 20 seconds.
The diastemas were restored with Esthet-X HD Micro Matrix Restorative (Dentsply Corp.). A layer of A2 was applied to block light transmission through the diastema, simulating the dentin layer. Characterization was accomplished by adding Pink Tint Venus applied with a No. 10 endodontic file into the surface of the A2.
This layer was cured for 20 seconds. A second layer of Esthet-X HD enamel shade WE was applied and contoured simulating the enamel layer. This layer was light cured for 20 seconds. The composite resin was then contoured, finished and polished with Sof-lex discs (3M ESPE).
Case No. 2
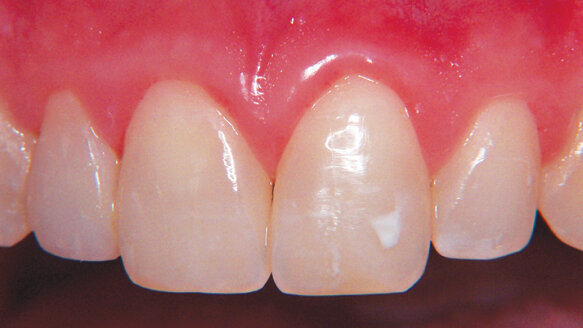
A 23 year-old healthy male presented with one peg-lateral incisor that he wished to improve esthetically. A peg-shaped lateral incisor can be defined as a tooth with reduced meso-distal diameter and with proximal surfaces converging markedly in the incisal direction.[25]
This tooth’s shape and size alteration is inherited genetically and occurs in the range of 1–2 percent of the population.[25,26] Options for treatment again included a porcelain veneer or restoration with composite bonding. The patient again opted for the biomimetic procedure of restoring with composite bonding.
Treatment
Treatment consisted of direct composite bonding to the upper right lateral incisor. No prepping of the tooth was required. The tooth was cleaned with pumice (Pumice Preppy, Whip Mix Corp.). A 35 percent phosphoric acid (Ultra Etch, Ultradent Products) was applied to the entire enamel surface for 15 seconds. The etchant was then rinsed off, leaving the enamel surface moist. The bonding agent, Prime & Bond NT (Dentsply Corp.), was applied, air thinned and light cured for 20 seconds.
Esthet-X HD Micro Matrix Restorative (Dentsply Corp.) shade C1 was applied, contoured and cured. This was followed by a layer of Esthet-X HD Micro Matrix Restorative (Dentsply Corp.). The ideal characteristics of very high polishability, varied opacity options and contourability make the Esthetix-X HD an excellent choice for this application. The restoration was then finished and polished with Sof-lex Discs (3M ESPE).
Summary
Biomimetic principles can be applied to cosmetic dental cases to minimize the reduction of existing healthy tooth structure in the pursuit of improved esthetics. The results can accomplish the esthetic enhancement, the cost to the patient can be reduced and the underlying tooth structure can be preserved for the present and future dental health of the patient.
Note: This article was originally published in Cosmetic Tribune U.S. Edition, Vol. 4 No. 7, July 2011. A complete list of references is available from the publisher.
About the author
Susan McMahon, DMD, has served as a clinical professor in prosthodontics and operative dentistry at the University of Pittsburgh School of Dental Medicine. She is a guest lecturer in cosmetic dentistry at West Virginia University School of Dentistry and lectures to dentists in the United States and Europe on tooth whitening and cosmetic dentistry.
The advent of human bone grafting has led to applications within the specialties of dental and sinus reconstructive surgery for corrections to maladies such...
The advent of human bone grafting has led to applications within the specialties of dental and sinus reconstructive surgery for corrections to maladies such...
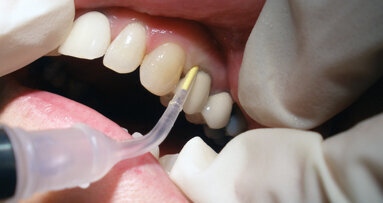
The STA Injection System (Fig. 1) available from Milestone Scientific, a computer-controlled local anesthetic delivery or C-CLAD, is not only great for ...
The STA Injection System, a computer-controlled local anesthetic delivery, or C-CLAD, is not only great for single tooth anesthesia, but is also very useful...
When opportunity knocks, is your practice ready to answer? As dentists we have opportunities every day to help our patients and contribute to improving our ...
NEW YORK, NY, USA: Revenues generated from cosmetic dental procedures will likely remain stable, if not increase, in the coming year, according to a recent ...
HONOLULU, HI, USA: Dr Jimmy Eubank, a world-renowned speaker and researcher in the field of cosmetic dentistry for more than 30 years, was honored with a ...
ALPHARETTA, GA / NEW YORK, NY, USA: Talk about having it made. Dr. Darrell Morton was recently chosen as the official cosmetic dentist for Georgia and South...
Success in gardening depends partially on pest control. The use of chemicals to inhibit pest growth often yields a healthier crop. Periodontal therapy is to...
BEVERLY HILLS, Calif., USA: Celebrity personality and actor Charlie Sheen recently visited Beverly Hills cosmetic dentist Dr. Kevin Sands. Following his ...
Live webinar
Mon. 8 June 2026
12:00 PM EST (New York)
Live webinar
Mon. 8 June 2026
1:00 PM EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 PM EST (New York)
Live webinar
Wed. 10 June 2026
11:00 AM EST (New York)
Live webinar
Wed. 10 June 2026
2:00 PM EST (New York)
Nacho Fernández-Baca DDS, MSc
Live webinar
Wed. 10 June 2026
7:00 PM EST (New York)
Live webinar
Thu. 11 June 2026
1:00 PM EST (New York)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East
















































To post a reply please login or register