Using a disposable CK2 microsurgical blade (SybronEndo), the incision is made. With the smaller size of this blade, very accurate incisions can be made that have a cleaner cut than those of the much larger BP #15 or BP #15S blade. As the incision is being made, the operator needs to visualize the suturing process.
Sometimes just a small variation in the design of the incision can make a big difference in the ability to achieve easier and less traumatic closure of the surgical flap. In general, the surgeon is working with relatively healthy tissue and no attempt should be made to remove or alter the periodontium. This is especially applicable when making a full sulcular flap.
All flaps are full thickness and the incision must be complete, so there is no inadvertent tearing upon retraction of the flap. The split thickness flap is to be avoided as it is the most traumatic and healing is compromised. The periosteum does not survive the flap reflection procedure. It has been postulated that depolymerized periosteal collagen plays a role in rapid reattachment of the flapped tissues to cortical bone.1 In general, all flaps should be extended, at a minimum, to the mesial of the second tooth anterior to the apex of the root being surgerized.
The flap design differs depending on the integrity of the bone over the roots, the amount and nature of the attached gingival tissue, the anatomy of the jaw and the absence or presence of fixed dental appliances. Basically, there are two flap designs: triangular (one releasing incision) and rectangular (two releasing incisions). They are normally either a full sulcular flap, or a mucogingival flap, depending on the location and situation. In general, the longer the length of the flap, the easier it is to control, and it has no effect on the healing process.
embedImagecenter("Imagecenter116",116);
The full sulcular flap: This design is routinely used in all posterior quadrants. The full sulcular flap should be used in the anterior if there is a thin zone of attached gingival tissue or there is a concern about the possibility of a dehiscence over the root of the tooth being operated on.
The incision is made through the gingival crest, following the curvature around the cervical of the teeth involved in the surgical area. The operator should attempt to incise the tissue through the crest of gingival to the osseous crest of bone, leaving the healthy gingival attachment intact. The advantage of the full sulcular flap is the ability of the operator to easily visualize the “emergence form” of the involved teeth.
The Leubke-Ochsenbein or Mucogingival Flap: This flap is used only when there is an adequate amount of attached gingival tissue present and the periodontal probing is within normal limits. The incision design should be scalloping in nature and generally follows the architecture of the teeth, which allows for easy repositioning upon completion of the apical microsurgical procedures.
All releasing incisions are made parallel to the long axis of the teeth. This is important because the blood supply to the area is also parallel to the long axis. If a “wide base” type flap is made, the blood supply to the tissue adjacent to the flap is compromised and healing may not be as predictable and uneventful. The reflection of the flap is accomplished using the Molt, or Ruddle R or Ruddle L (SybronEndo) periosteal elevators. The working end of the instrument is gently inserted into the releasing incision, line into the free gingival tissue apical to the mucogingival attachment, and as far apically as the incision and boney contours will gently permit.
The instrument is manipulated in a gentle apical-to-coronal movement within the unattached gingival portion of the flap. Maintaining the same motion, the instrument is moved slowly toward the same apical position at the more distal extent of the flap. The working end of the elevator should be sharp so the reflection will be a “dissecting” process, so crushing or tearing of the tissue is avoided. Occasionally, especially in the posterior quadrants of the mandible, the mucogingival line will clinically seem to be firmly attached to a microscopic boney ridge. The attached tissue must be gently dissected from it. Once the mesial few millimeters are elevated, the rest will generally “peel away” without much effort at all and easily release from the osseous surface. The time spent initially, to gently free the attached gingiva, will be rewarded by a more uneventful healing process. This atraumatic elevation and reflection of the flap is a major contributor to the rapid healing response routinely observed only 24 hours postoperatively. It is important the approximating surfaces of the flap are never touched after the incision is completed, so there are no crushing injuries to inhibit or retard the healing process. An instrument such as the old wax spatula-shaped periosteal elevator has no place in the armamentarium of the endodontic micro surgeon.
Once the flap is gently and cleanly reflected, any “tissue tags” should be left intact as they will aid in the healing process. It is not necessary to clean the flap and exposed bone because these efforts are time consuming, could be traumatic to both the hard and soft tissue, and ultimately compromise the healing process.
The retraction of the flap must also be accomplished in a gentle and atraumatic manner. The most common cause of postoperative pain and swelling arises from impingement of the tissue during the retraction process. The surgeon has to constantly monitor the end of the retractor to make sure there is no inadvertent impingement on the flap. This is when the “scope assistant” is most helpful because he or she is observing the surgical site with a different set of eyes! An effective way to achieve atraumatic retraction is to prepare a groove in the cortical plate of the bone, well apical to the anticipated access to the root-end.
A surgical length #8 round bur, on a high speed Innovator handpiece (SybronEndo), is used to make the groove. A high-speed handpiece that has air escaping from the working end should never be used because of the danger of air embolism. The “groove” creates a definite place for the retractor instrument to seat into and is easily maintained in position, by either the doctor or the assistant, and eliminates the problem of inadvertently slipping during the surgery. Impingement of the tissue is also more predictably avoided by using a groove to hold the retractor.
Retraction can be accomplished using either the Carr or Rubinstein Retractors; however, there are many styles of retractors to choose from. The retractor is chosen that will best maintain clear visibility to the surgical area and is comfortable for the operator.
After the flap is retracted and if there is any tension on the flap, the vertical releasing incision can be extended, or an additional “releasing incision” at the opposite side of the flap can be considered. The releasing incision is usually very minimal, only 3–4 mm long, and many times does not require suturing.
It is imperative the operator keeps in mind there should be no tension or stretching of the tissues. One should not hesitate to extend or modify the incision to eliminate tension on the tissues. When there is tension, there is usually an opportunity for crushing or ischemia of the tissue and a resultant delay in the healing process. Generally speaking, the larger the flap, the easier it is to maintain atraumatically during the surgical procedure.
It is important the tissues and osseous surface must be kept as moist as possible during the entire procedure. This can be accomplished with a fine stream of water from the Stropko irrigator (www.stropko.com).
Dr Berman, an old retired general surgeon and one of my dental school instructors, would begin each surgery by saying, “Treat the tissues with tender loving kindness and they will respond in a like manner.” How many times I have heard those very words while performing apical microsurgery. Apical microsurgery can truly be a gentle technique.
(This is part two in a six-part series on apical microsurgery.)
About the author
John J. Stropko received his DDS from Indiana University in 1964, and for 24 years practiced restorative dentistry. In 1989, he received a certificate for endodontics from Boston University and recently retired from the private practice of endodontics in Scottsdale, AZ, USA. Stropko is an internationally recognized authority on micro-endodontics. He has been a visiting clinical instructor at the Pacific Endodontic Research Foundation (PERF), an adjunct assistant professor at Boston University and an assistant professor of graduate clinical endodontics at Loma Linda University. His research on ‘in-vivo root canal morphology’ has been published in the Journal of Endodontics. He is the inventor of the Stropko Irrigator, has published in several journals and textbooks and is an internationally known speaker. Stropko has performed numerous live micro-endodontic and micro-surgical demonstrations.
Reference
1. Harrison JW, Jurosky KA. Wound healing in the tissue of the periodontium following periradicular surgery. II. The dissectional wound. J Endod 1991; 17 (11): 544-52
Surgery will never replace solid endodontic principles and should always be a last resort. Apical microsurgery consists of nine basic steps that must be ...
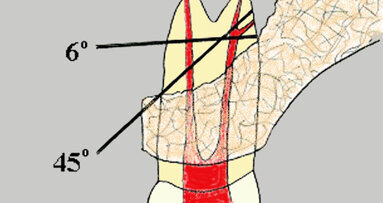
The amount, or degree, of the root-end bevel (REB) is of utmost importance and should be precisely planned in advance after considering the overall ...
In Parts 1 and 2, I discussed the preparation of the patient, the incision and atraumatic flap elevation. These are the first three steps necessary to ...
All steps have been meticulously followed, the REF has been placed, the crypt has refilled nicely, the final radiograph has been approved, and it is time to...
In Parts 1 through 4, the necessary steps and procedures were presented, enabling the operator to atraumatically and predictably allow the root-end ...
The first article I wrote on CAD/CAM 25 years ago was about the three Ps: prep, powder and picture. At that time, all we were worried about was the final ...
The American College of Prosthodontists is taking Southwest Florida by storm from Wednesday through Saturday. The JW Marriott Marco Island will host this ...
In performing long-lasting comprehensive dentistry, form, function, esthetics and stability are the attributes that we strive for and should for good ...
Carrying on the conversation from the first part on the ongoing fight for improved safety in anaesthesia in dentistry, Dental Tribune International again ...
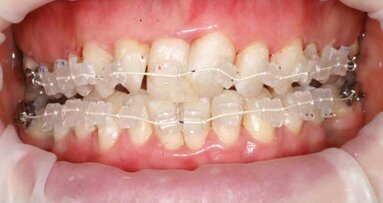
Thanks to the latest advances in cosmetic tooth alignment, general dentists are now able to provide simple, straightforward treatment for adult patients ...
Live webinar
Fri. 22 May 2026
10:00 AM EST (New York)
Dr. Paweł Aleksandrowicz PhD
Live webinar
Fri. 22 May 2026
11:00 AM EST (New York)
Live webinar
Fri. 22 May 2026
12:00 PM EST (New York)
Prof. Dr. Ali Murat Kökat
Live webinar
Fri. 22 May 2026
1:00 PM EST (New York)
Live webinar
Fri. 22 May 2026
2:00 PM EST (New York)
Live webinar
Tue. 26 May 2026
12:00 PM EST (New York)
Live webinar
Tue. 26 May 2026
2:00 PM EST (New York)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East






































To post a reply please login or register