Dental implants are placed either utilizing a one-stage approach (healing abutment placed at implant placement) or a two-stage approach (implant is covered by soft tissue at time of placement) and modification of the soft tissue to expose the implant fully may be required. When the prosthetic phase is initiated, soft tissue is either removed to uncover the implants or reshaped at gingival margin for better esthetics, which can be accomplished by several methods.
A cutting instrument (i.e., scalpel or tissue punch[1]) has been the traditional approach to incise through the soft tissue to the underlying implant.
The result is a bleeding edge that can interfere with impressions if they are to be taken at the same appointment. Additionally, postoperative sensitivity has been reported and can result from the fresh cut edge. Typically a delay of two weeks or longer is required before impressions can be taken, so that bleeding doesn’t hamper the accuracy of how the soft tissue is captured.
An alternative to the blade, electrosurgery has been offered as it can cauterize the cut edges and decrease postoperative bleeding. Yet, this presents with two negatives outcomes to its use in and around dental implants.
embedImagecenter("Imagecenter_1_2177",2177, "large");
Electrosurgery requires a circuit be formed between the monopolar tip intraorally and the surgical unit with a grounding plate placed on the patient a distance from the oral cavity. When the current is activated, it flows between the electrosurgery tip through the soft tissue to the grounding plate, completing the circuit with the metallic implant conducting the current along the path.[2] Temperature increases have been reported that when exceeding a threshold of 10 degrees C at the osseous interface with the implant may lead to bone loss and possible de-integration of the implant. A general recommendation is to avoid electrosurgery units in and around dental implants.
As electrosurgery affects cell layers deep to the surface (deeper penetrating), combined with the temperature increase, tissue shrinkage is often reported.[3] A delay between uncovery and impressions allows the cut edge of gingival tissue to stabilize and is required so the gingival margin captured is stable when the prosthetics is returned for insertion.
Diode lasers are increasingly being utilized in dental practices due to both lower costs to implement this technology than the more expensive CO2 and ND:YAG lasers and the wide range of effective treatment afforded by these devices. Diode lasers, such as the Picasso Lite+ (AMD Lasers, Indianapolis, IN, www.amdlasers.com) (Fig. 1), provide adequate power to modify soft tissue in and around the dental implant for uncovery or alteration of the gingival margin to improve the esthetics.
Additionally, these operate within the temperature range recommended, so that the negative effects associated with electrosurgery do not occur to the bone around the implant.[4] Coagulation can also be controlled combined with the lack of tissue shrinkage after use of the diode laser allowing impressions to be taken at the time of uncovery. As the diode laser affects fewer cell layers, tissue response does not involve an inflammatory response that can lead to tissue shrinkage during the healing period the first few weeks after treatment (Fig. 2).[5-9]
Utilization of the diode laser
Diode lasers are primarily used in a contact application when cutting or coagulation is required.[10] The diode laser tip is used in either an initiated state or an uninitiated state. Initiated refers to the tip of the diode laser, which has been coated with a blocking material. This allows energy from the diode, when activated, to heat the tip causing cell ablation (vaporization) at the contact point with cutting resulting.[11] The light energy in the coated tip is converted into heat by refraction of the blocking material on the diodes tip creating a “hot tip.”
This secondary thermal effect of the heated tip allows cutting or incising of the soft tissue, resulting in an area of carbonization at the border of the vaporization. Coagulation occurs in the tissue bordering this zone of carbonization as a result of contact with the overheated tip rather than by the laser energy itself (Fig. 3).
Bacterial decontamination can be accomplished with an unitiated diode tip, which is useful in treatment of peri-implantitis on the implants’ surface or within the periodontal sulcus/pocket around implants and natural teeth.
Initiation of the tip is accomplished with the diode set at 0.5 watts and touched to a piece of blue articulating paper (Bausch Ref BK05), and the laser is activated for one second. This is repeated six to eight times, contacting different areas of the tip so that when finished the entire tip and 3-4 mm of the sides have been marked with the articulating paper. It is recommended to avoid articulating ribbon as it will ignite and is ineffective in initiating the tip. A properly initiated tip will glow orange when the foot pedal is depressed.[12]
The tip should be wiped with a piece of dry gauze to remove debris periodically as it is being utilized to maintain efficiency. When cutting fibrous tissue, it may be necessary to reinitiate the tip during the procedure if the tip appears to not be cutting well.
Cutting efficiency is related to wattage. The higher the wattage, the faster the soft tissue is vaporized. But a greater zone of unwanted lateral thermal damage may result. It is advised to use the lowest wattage to accomplish the task to avoid the risk of thermal damage within the adjacent tissue. The assistant during usage of the diode laser uses the HVE near the site to remove any odors and periodically can spray water on the site to aid in cooling the tissue.
This also minimizes thermal issues, which improves initial healing. To remove the soft tissue covering the implants’ cover screw or reshape the tissue for esthetics, a setting of 0.8-1.0 watts in a continuous mode is usually sufficient. A 400 micron diode tip (orange) is utilized for oral and periodontal surgical applications. The 300 micron tip (purple) is designed for periodontal applications such as Laser Assisted Periodontal Treatment (LAPT).
Beyond the carbonization zone, an area of hemostasis (coagulation) occurs. Typically, sites treated with the diode laser will demonstrate little to no bleeding depending on the condition of the tissue prior to treatment. Tissue that is hemorrhagic will require longer contact with the diode laser to achieve coagulation and may ooze due to the inflammation present prior to laser treatment. The coagulation effects and lack of post-treatment tissue shrinkage allow immediate implant impressions should that be desired.
The laser also creates an area of biostimulation adjacent to the coagulation area.
Following irradiation with a diode laser, tissues and cells have a biostimulatory effect that provides faster or more favorable wound healing compared to tissue treated with a scalpel or electrosurgical unit. The laser irradiation stimulates the proliferation of mesenchymal stem cells without DNA alterations in the affected cells.[13] Thus, wound healing is enhanced and soft tissue at the cut edges demonstrates faster healing than when treated with a scalpel or other methods by stimulation of gingival fibroblasts inducing growth factors.[14,15]
It has been reported that biostimulation via the diode laser also has a positive effect on bone cells and can be stimulatory to the bone cells at the crest around the implant.[16,17] Compared to conventional methods, tissue healing as well as postoperative sensitivity is less with the diode laser then with other methods.[18]
Implant uncovery technical considerations
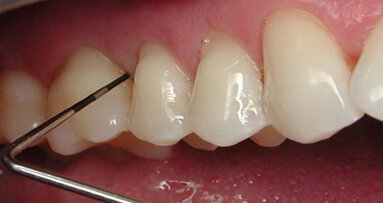
The width of attached gingiva remaining will dictate the best method for implant uncovery (Fig. 4a). When a wide band of attached gingiva is present and a sufficient amount (3 mm or greater) will be present after uncovery on both the buccal and lingual, then the diode laser is activated and inserted at the center of the site and worked in a spiral pattern outward until the entire cover screw is exposed (Fig. 4b).
A curette or other instrument may be necessary to loosen the tissue over the cover screw as the periosteum becomes adherent to the titanium cover screw during implant healing. Sites that present with a narrow width of attached gingiva of 3-5 mm at the crest’s center will require some conservation of the remaining attached gingiva. In this clinical situation, the diode is utilized to remove an elliptical piece of soft tissue over the cover screw, and then the tissue is pushed buccally and lingually to preserve the attached gingiva (Fig. 4c).
If less attached gingiva is present on either side of the center of the crest, then the practitioner will need to preserve all of the attached gingiva present, and a conventional flap is recommended to be able to position the tissue in a more apical direction. When this is necessary, incisions can be made with the diode laser as an alternative to a scalpel (Fig. 5).
Case report
A 30-year-old female patient presented with severely malposed maxillary central incisors tipped facially and a desire for esthetic improvement. A CBCT was taken and minimal bone was noted present over the facial of the central incisors. Options for treatment were presented to the patient that included: orthodontics to correct esthetics or extraction of the central incisors, placement of implants at these sites and restorations on the anterior teeth. The patient indicated she did not wish to pursue an orthodontic treatment option due to the time involved.
The patient presented for surgery and the central incisors were atraumatically extracted under local anesthetic. The adjacent teeth were prepared for crowns, which would support a provisional bridge during the healing/integration period. A 4-mm wide, 24-degree Co-Axis Implant (Keystone Dental, Burlington, Mass.) was placed into the osteotomy at each central incisor orienting the prosthetic axis to a vertical position, while the implant’s body followed the trajectory of the premaxilla.
A healing screw was placed and osseous graft material (NovaBone, Jacksonville, Fla.) placed on the facial to thicken the resulting bone. The soft tissue was closed with resorbable PGA sutures. A stent created over the wax-up of the study models that had been modified was filled with an auto-cure provisional resin (Perfectemp 10, DenMat, Lompoc, Calif.) and seated over the anterior and allowed to set. Upon setting, the stent with provisional was removed intraorally and trimmed and polished. At the implant sites, the material was shaped to a bullet shape to assist in forming an emergence profile in the soft tissue and preserve the papillas.
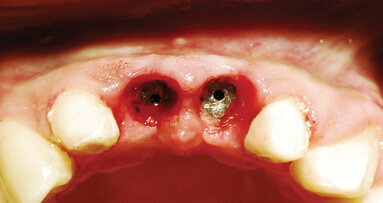
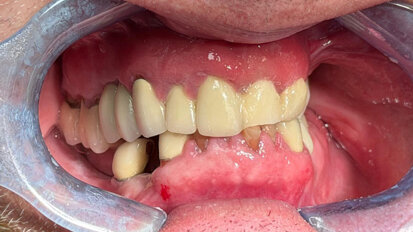
Six months post-implant placement, the provisional bridge was removed and preservation of the papillas was confirmed with a natural emergence profile within soft tissue (Figs. 6,7). Local anesthetic was administered. The Picasso Lite+ diode laser was set at 2.5 watts in continuous mode with an initiated tip and at the center of the depression in the soft tissue above the implants cover screw and moved in a circular motion moving outward until the entire cover screw was exposed (Fig. 8).
The process cuts the desired soft tissue and coagulates any bleeding from the cut edges. This was then repeated on the second implant (Fig. 9). Open tray implant impression abutments were placed into the implants and seating verified radiographically. An impression of the maxillary arch was taken utilizing Aquasil heavy body VPS (DENTSPLY Caulk, Milford, Del.) in a Mira Advanced Implant tray (Hager Worldwide, Hickory, N.C.) and Aquasil Ultra syringed around the preparations and implant abutment heads. Healing abutments were placed into the implants (Fig. 10). The previously placed provisional bridge was tried in and modified at the pontics to allow the bridge to fully seat over the healing abutments and luted with a provisional cement (Fuji Temp LT, GC America, Alsip, Ill.).
Two weeks later, the prosthetics returned from the lab (DenMat Labs, Lompoc, Calif.) and the provisional bridge was removed. The healing abutments were removed and the soft tissue demonstrated a lack of inflammation and a good periodontal health where it had been modified by the diode laser (Fig. 11). Ceramic crowns were tried in on teeth 7, 10 and 11, and the screw-retained zirconia-based implant crowns inserted. A radiograph was taken verifying fit of the implant prosthetics. A torque wrench was utilized to tighten the fixation screws on the implants to 30 Ncm and the ceramic crowns were luted with Panavia SA resin cement (Kuraray, NY, N.Y.). Occlusion was checked and adjusted where needed.
Conclusion
Diode lasers are a useful adjunct to soft-tissue modification to uncover dental implants or esthetically recontour the gingival margin. They provide better safety than electrosurgery, maintaining a temperature profile within the safety zone of bone and do not cause tissue shrinkage that can affect the esthetic outcome. As the diode’s tip provides simultaneous cutting and coagulation (hemostasis), a clear advantage to the use of a scalpel or tissue punch is that immediate impressions can be accomplished without site bleeding affecting the accuracy of the capture of the soft-tissue contours and position.
Note: This article was published in Implants, the international C.E. magazine of oral implantology, North America Edition, Vol. 4, Issue 4, 2015. A complete list of references is available from the publisher.
Dental implants are placed either utilizing a one-stage approach (healing abutment placed at implant placement) or a two-stage approach (implant is covered ...
NEW YORK, NY, USA: With international certifications now in place for its Picasso diode laser, AMD LASERS is poised for continued growth in North America as...
NEW YORK, NY, USA: For any dentist interested in adding laser technology to his or her practice, AMD LASERS, a company based in Indianapolis, IN, USA, has ...
ANAHEIM, CA, USA: AMD LASERS, the company that builds the world’s most affordable dental laser technology, announces the launch of the Picasso soft ...
There are many opinions, both in favor of and against, the utilization of lasers in periodontal therapy. There are also many reports of the different ...
While dental lasers have been commercially available for several decades and their popularity among patients is unparalleled, the dental profession has ...
TULSA, OKLA., USA: AMD LASERS, a global developer and manufacturer of dental lasers and provider of dental laser education, has announced that its Picasso ...
The concept of using dental lasers for the treatment of periodontal disease elicits very strong reactions from both ends of the spectrum. Everyone has an ...
Did you know that in addition to its advanced dental treatments, the Fotona LightWalker laser can also offer patients facial aesthetic rejuvenation options?...
AMD LASERS — a company based in Indianapolis, IN, USA, that manufactures laser therapy equipment for dentists that is easy to use and affordable ...
Live webinar
Tue. 26 May 2026
12:00 PM EST (New York)
Live webinar
Tue. 26 May 2026
2:00 PM EST (New York)
Live webinar
Wed. 27 May 2026
8:00 AM EST (New York)
Live webinar
Thu. 28 May 2026
12:00 PM EST (New York)
Dr. Anthony Viazis DDS, MS. Inventor & Founder of Fastbraces®
Live webinar
Mon. 1 June 2026
1:00 PM EST (New York)
Live webinar
Wed. 3 June 2026
1:00 PM EST (New York)
Live webinar
Thu. 4 June 2026
2:00 PM EST (New York)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East














































To post a reply please login or register