A myriad of factors influences the initiation and progression of peri-implant disease; unfortunately, the treatment of peri-implant disease is at best favourable in the short term, the disease having a high rate of persistent inflammation and recurrence.3 A study by Guarnieri et al. showed that active periodontal therapy in chronic periodontal patients followed by long-term regular periodontal maintenance was successful in the retention of the majority of periodontally compromised teeth.4 In the same patients, a higher tendency for implant loss than tooth loss was found. The series of case reports presented in this article will provide decision guide categories for best practices which facilitate retention of compromised teeth using endodontic therapies.
Case report 1: CBCT in endodontics
Perhaps the most important advantage of CBCT in endodontics is that it demonstrates anatomical features in 3D that intra-oral, panoramic and cephalometric images cannot. In addition, because reconstruction of CBCT data is performed natively using a personal computer, data can be reoriented in true spatial relationships.5
In October 2015, a 55-year-old male patient, previously seen for treatment in the office, self-referred for a second opinion regarding the recommended extraction of a suspected fractured tooth in the maxillary right quadrant. He reported that a soft swelling had become apparent over the past week. Clinical examination noted fluctuant swelling between tooth #15 and tooth #14, and a 12 mm probing defect was detected along the mesiobuccal line angle of tooth #15.
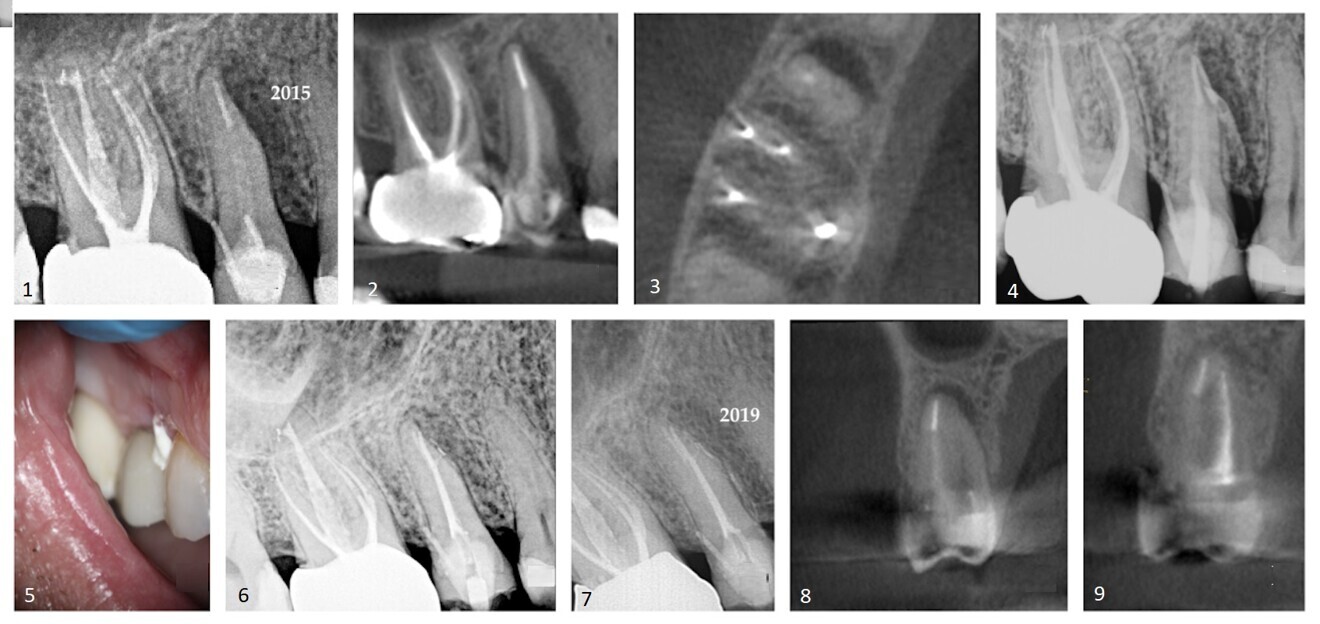
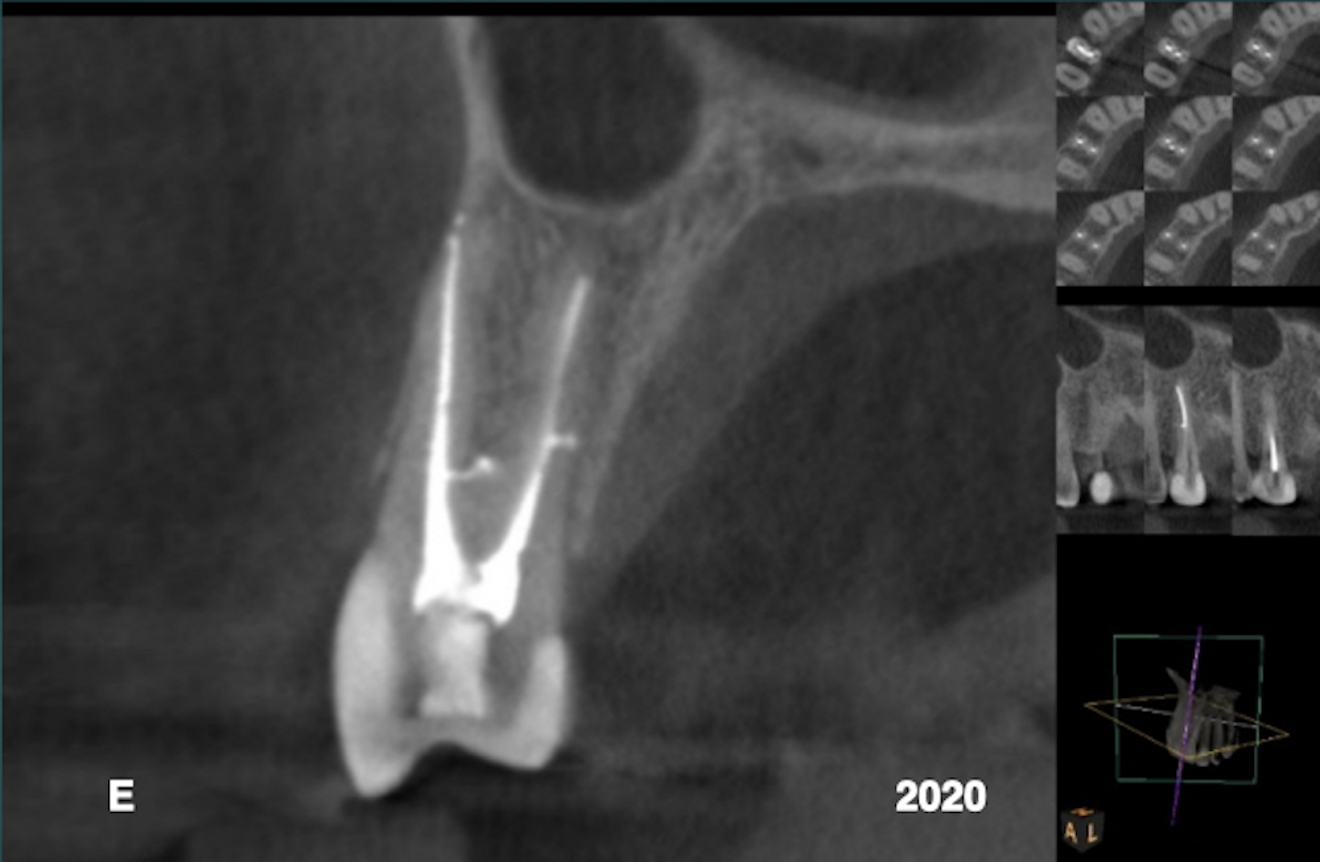
The patient provided a periapical radiograph showing a mesio-proximal periradicular radiolucency associated with tooth #15 (Fig. 1). The sagittal slice of the CBCT volume (Carestream CS 9000, Carestream Dental) showed the extent of the lesion (Fig. 2). In the previous root canal therapy, only the buccal canal had been detected and treated. The axial slice showed an untreated palatal canal (Fig. 3). A fibre post placed in the buccal canal had been used to retain the core. The patient was advised of the misdirected anchoring pin extending into the periodontal ligament. With the patient’s consent, it was decided to selectively treat the palatal canal.
After an interim six-week period of calcium hydroxide therapy (UltraCal XS, Ultradent; Figs. 4 & 5),6 the root canal space was obturated using a warm vertical condensation technique.7 The obturation material was expressed into a lateral branching portal of exit (Fig. 6). The four-year follow-up showed resolution of the lateral lesion (Figs. 7–9). The initial presumption of a fractured root was proven false, suggesting that diagnosing conditions based on insufficient data acquisition is unreliable. The use of CBCT is an imperative in endodontic procedures of any kind provided ALARA (as low as reasonably achievable) principles regarding radiation dose are followed.
Case report 2: Root amputation (periodontal and endodontic lesion)
Root resection is a treatment option for molars with advanced furcation involvement. In a study by Derks et al., mandibular molars after root resection showed a survival probability of almost 80% even 20 years later.8
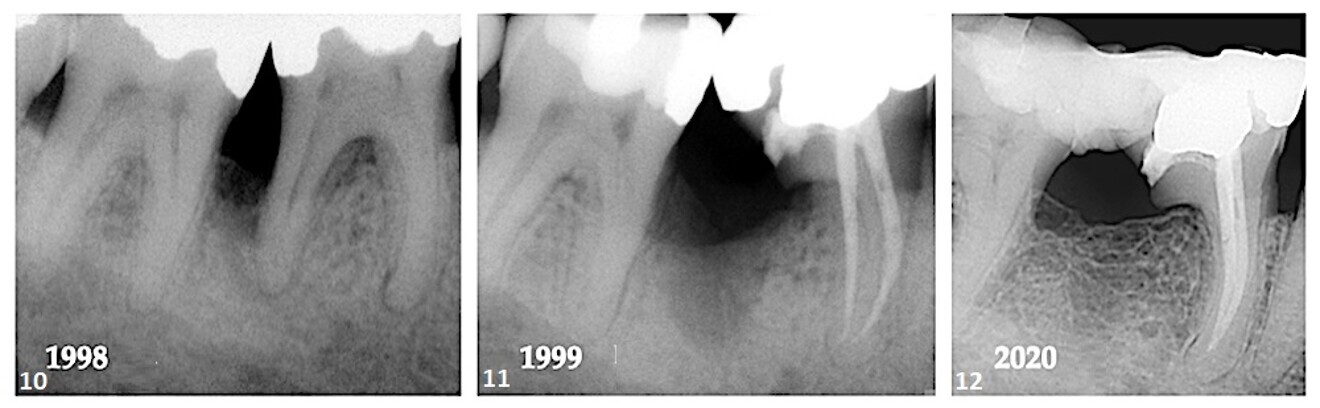
In October 1998, a 39-year-old male patient presented to the office complaining of gingival tenderness in the mandibular right quadrant. Extensive bone loss was noted interproximally between tooth #47 and tooth #46; however, the periodontal status of the dentition in general was within normal limits. Pulp sensibility testing of the teeth in the mandibular right quadrant identified the pulp of tooth #46 to be necrotic (Fig. 10). It was explained to the patient that treatment of periodontal and endodontic lesions was in general unfavourable and that success depended on the severity of bone loss, root trunk length, degree of root separation, curvature of the root to be resected, ability to eradicate the osseous defect, pulpal status, and restorative and oral hygiene procedures required.
With the patient’s consent, the distal root of tooth #46 was resected and the overlying crown portion retained (Fig. 11). At some point after the amputation procedure, the referring dentist splinted teeth #47 and 46 with a composite and Ribbond bridge. Twenty-two years after the initial procedure, osseous regeneration and cortication in the furcal region were evident between teeth #47 and 46 (Fig. 12).
Advancements in strategies to maintain compromised teeth in concert with a greater understanding of risk factors associated with dental implants invite a reassessment of the benefits of strategic extraction of a tooth with a questionable prognosis or of limited strategic value.9 With the use of hard- and soft-tissue augmentation procedures, platelet-rich fibrin, minimally invasive flap design and suturing techniques in conjunction with surgical operating microscopes, it is unreasonable to sacrifice a tooth for an implant when this venerable treatment option shows favourable prognosis and success rates.10
Case report 3: Resorptive defect
Progressive internal resorption or those instances with perforations of the root can be distinguished from external resorption by varied radiographic techniques. In teeth with internal resorption, the radiolucent lesion moves with the canal when the radiographs are taken at different angles, whereas in external resorption the radiolucent lesion moves outside of the canal.11, 12
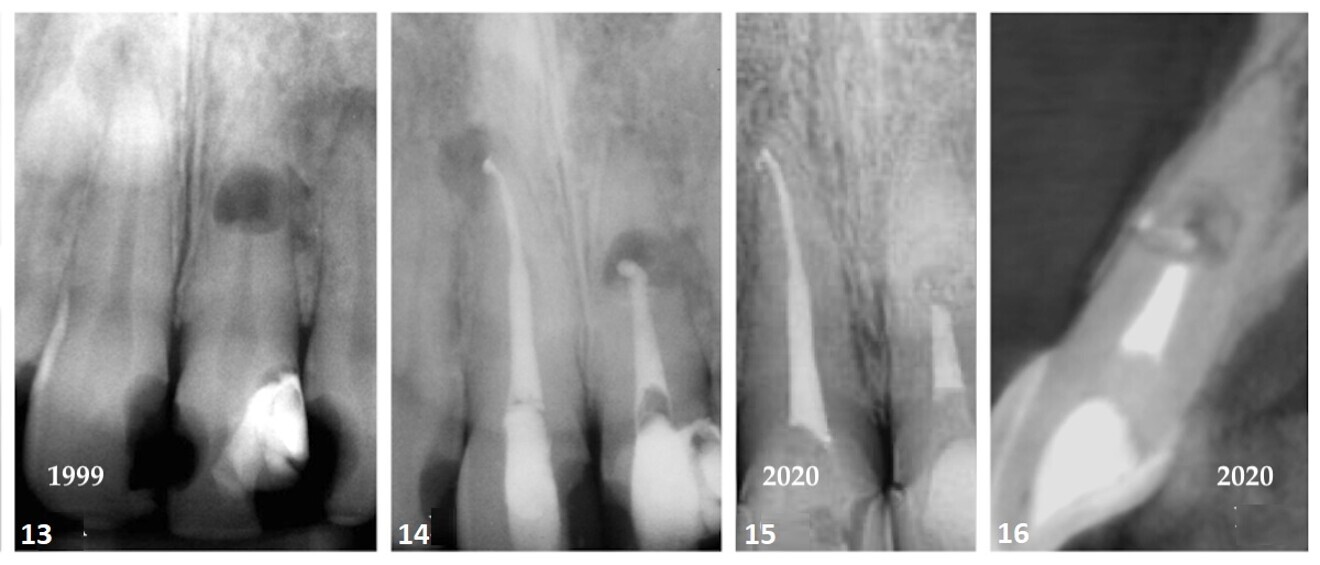
In March 1999, a 47-year-old female patient presented to the office with facial swelling, and tooth #11 was tender to percussion. A periapical radiograph of the maxillary anterior sextant showed large Class III and IV restorations. Tooth #11 exhibited periapical rarefaction. Tooth #21 showed internal resorption at the mid-root level (Fig. 13). The patient reported that tooth #21 had been traumatised some 35 years before. In the absence of CBCT imaging, it was assumed that the resorption had perforated the facial aspect of the root and disrupted the overlying cortical bone.
Pulpal sensibility testing of the teeth in the anterior determined that tooth #11 was pulpless. The tooth was endodontically treated and obturated using a warm vertical condensation technique. Tooth #21 was instrumented to the incisal level of the resorptive defect, and the canal sealed with white mineral trioxide aggregate (Fig. 14).13 Were the tooth to be treated today, the choice of obturation material would be EndoSequence BC putty (Brasseler). Currently, there is a trend towards the use of an injectable platelet-rich fibrin regenerative approach to resolve internal resorptive defects that shows great potential for long-term healing.14 Follow-up after 21 years showed that the periradicular radiolucency associated with tooth #11 had resolved and that the resorptive defect had been reduced in size (Figs. 15 & 16).
Case report 4: Cracked tooth
In a study of 2,086 cracked teeth by Krell and Caplan,15 the most common teeth demonstrating fracture were mandibular second molars (36%) followed by mandibular first molars (27%) and maxillary first molars (18%). There were no statistically significant differences in treatment success based on pulpal diagnosis (irreversible pulpitis, 85%; necrosis 80%; previously treated, 74%), patients’ age or sex, year of treatment, tooth type, restorative material or number of restored surfaces at the time of examination.
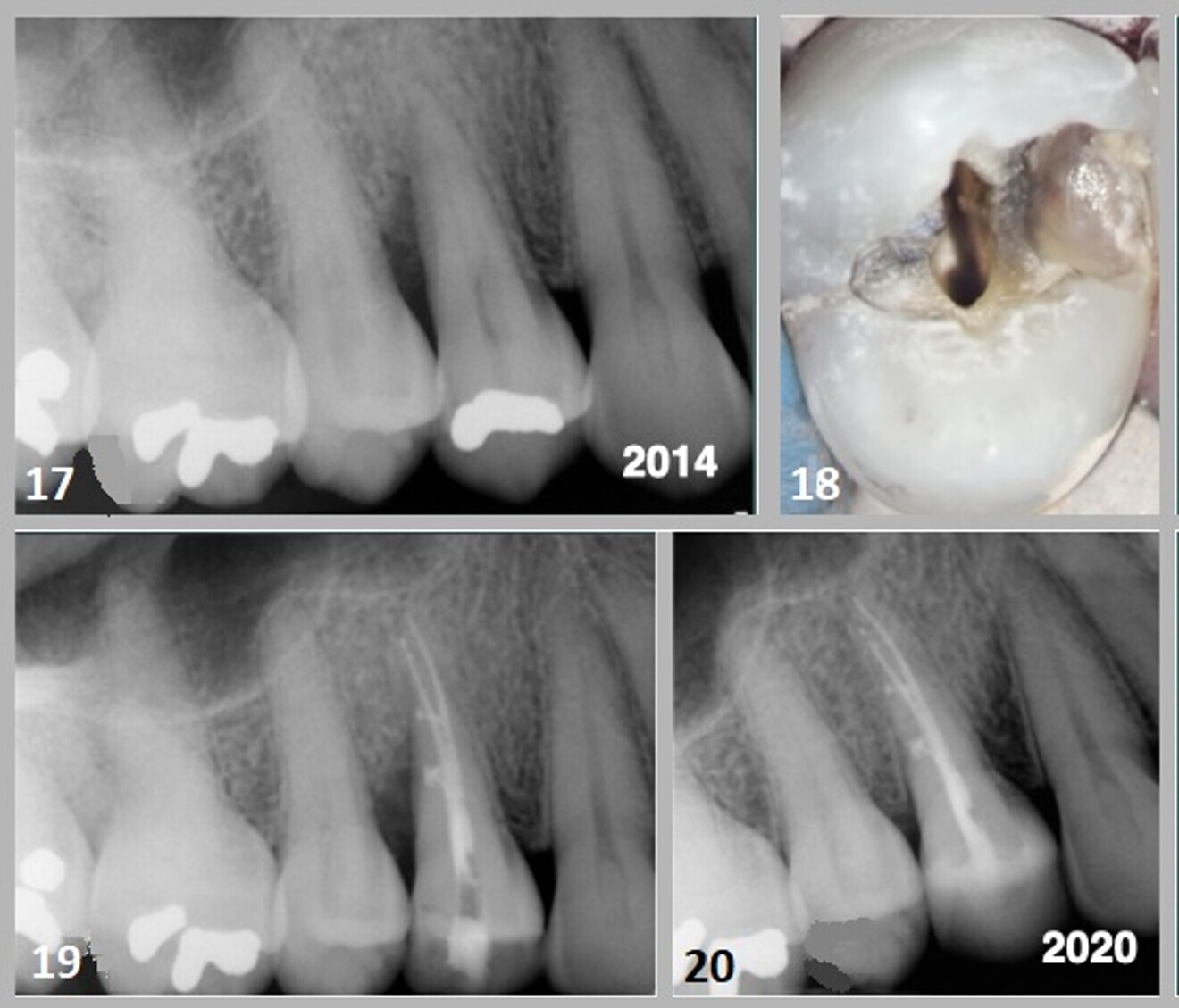
In July 2014, a 45-year-old female patient presented to the office with the chief complaint of swelling in the distal papilla of tooth #14 for a period of ten days. Clinical examination revealed an occlusal amalgam restoration with a probeable seam in the distal marginal ridge. The probing depths along the distobuccal and lingual line angles of the tooth demonstrated an infrabony pocket of 8 mm. The periapical radiograph showed a small amalgam restoration with a vertically angulated radiolucency interproximally between tooth #14 and tooth #15. A fracture line extending into the mesial marginal ridge was identified (Figs. 17 & 18). The tooth was assessed for vitality with thermal and electric pulp tests, which elicited no response.
The treatment options were explained to the patient: (1) extraction and restoration with a three-unit fixed bridge; (2) extraction, soft- and hard-tissue augmentation, and implant-retained restoration; or (3) root canal therapy and restoration with cuspal protection. The patient was advised that the third option had a questionable prognosis; however, for financial reasons, she chose to proceed with that option. It should be noted that management of cracked tooth syndrome varies based on the severity of the symptoms and depth of tooth structure involved.
Endodontic therapy was performed using a warm vertical condensation technique (Fig. 19). The access preparation was sealed with a flowable and hybrid composite restoration using the Bioclear Matrix system developed by Dr David Clark. The radiograph taken at a six-year follow-up (2020) showed osseous regeneration in the interproximal area, which had eliminated the periodontal defect (Fig. 20).
Conclusion
The treatment planning process demands the inclusion of a myriad of data pertaining to the status of the tooth and root structure. The decision guide of the American Association of Endodontists encourages the clinician to consider local and systemic case-specific issues, economics, the patient’s desires and needs, aesthetics, potential adverse outcomes and ethical factors. The treatment performed must reflect best practices for the patient’s needs.



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East


















































To post a reply please login or register