Relapse of mandibular anterior crowding occurs in many well-treated cases, whether they had bicuspid extraction, non-extraction treatment, third molar removal, non-removal or agenesis. Why? Is it related to (a) form and function, (b) tooth-mass issues, (c) occlusion, (d) temporomandibular relationship, (e) arch length discrepancy, (f) heredity, (g) orofacial musculature, (h) intra-oral forces, (i) extraoral forces or (j) oral habits?
Or is it a combination of all the above?
The literature is filled with quality research studies attempting to discover answers to why relapse occurs, and despite decades of research, lower anterior crowding is still unpredictable (Freitas, K., Freitas, M., Henriques, J., Pinzan, A., & Janson, G., 2004). “The degree of post-retention anterior crowding is both unpredictable and variable and no pre-treatment variables either from clinical findings, casts, or cephalometric radiographs before or after treatment seem to be useful predictors” (Little, 1999, p.191).
For many years, the implication has been that nonextraction orthodontic cases might result in a higher percentage of postretention lower anterior crowding compared to extraction cases, but do they? Review of the literature regarding the effects that third molars have on lower anterior crowding presents both agreement and opposition for both sides of the problem, but the bulk of the evidence seems to indicate that third molars play an insignificant role in lower anterior crowding.
Parallel studies often show dissimilar deductions, and, more than likely, the problem is multifactorial. Bramante (1990) noted that in the 1930s Dr. Charles Tweed redirected orthodontic treatment procedures to extraction therapy with the removal of four first premolars as a more disciplined approach to effective orthodontic treatment. He added: “Fifty years later, we have found that extraction treatment and uprighting lower incisors does not prevent long-term post-retention crowding and that flattened profiles are not always esthetically desirable” (p. 91).
Form and function certainly underlie growth and development in the craniofacial skeleton and the role that the biological environment plays. According to Carlson (1999), the “form-function” principle of craniofacial biology in general was attractive but primarily to account for the factors that may have influenced broad morphological variation and change associated with the evolution of the whole complex. Carlson added that the form-function principal is much less effective in explaining variations of craniofacial form, growth and treatment outcomes associated with causes of skeletal discrepancies and malocclusion.
So where does the discussion of lower incisor crowding end? Is the problem multifactorial, a product of improper orthodontic treatment modalities (or techniques), form vs. function, or does genetics play a large part in creating or solving the problem?
We can go on and on discussing virtues of the many possibilities and causative factors involved with post-retention relapse of lower incisor crowding, but here we are in the 21st century and cannot provide an absolute answer to the riddle of postreatment stability. It is still an important objective but also still a scar of orthodontics.
Answers may never be absolutely identified, which, of course, begs consideration for some form of indefinite retention in almost all cases. However, we shouldn’t feel totally alone with regard to our knowledge (or lack of knowledge) for an absolute answer to why relapse of postretention tooth movement occurs because, according to our medical colleagues at the Mayo Clinic (n.d.), even after years of research, physicians still have no cure for the common cold either.
Note: This article was published in Ortho Tribune U.S. Edition, Vol. 8 Nos. 3/4, AAO Review 2013. A complete list of references is available from the publisher.
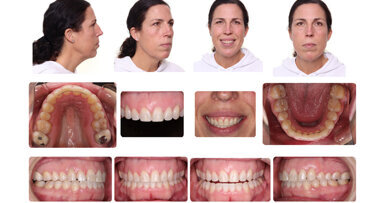
A 48-year-old female presented with a Class I crowded malocclusion with moderate maxillary and mandibular crowding. The facial profile was convex with a ...
A 21-year-old male presented with a chief complaint of relapse of adolescent orthodontic treatment. He expressed an interest in clear aligner therapy for ...
The aetiology of external cervical root resorption remains unclear, and it is probably a multifactorial problem, causing dentine exposure to the oral cavity...
Anterior open bites present orthodontists with a unique challenge: achieving successful and timely treatment while minimizing patient inconvenience. ...
This article illustrates recent advancements by Glidewell Laboratories to improve the esthetic properties of BruxZir Solid Zirconia restorations. As the ...
BruxZir Solid Zirconia crowns and bridges were originally designed by Glidewell Laboratories as an esthetic alternative to posterior cast gold or metal ...
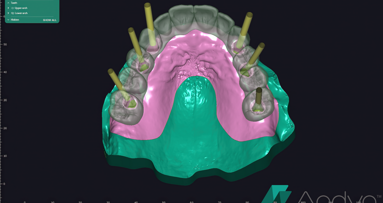
This article shows the step-by-step laboratory production process of a log-term prototype for the development and sculpting of anterior gingival tissue. The...
LEIPZIG, Germany: A free webinar, to be presented by the Dental Tribune Study Club on July 30, will introduce a novel anterior restorative from the makers ...
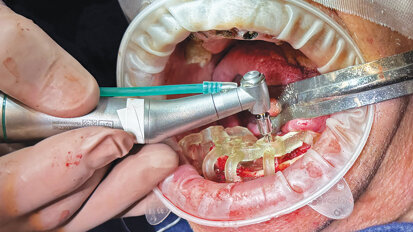
Michael Boyd, a 55-year-old male, lived a life of many challenges. By age 52, Michael had a diabetic medical emergency and upon recovery was relieved of his...
With its Single Tooth Anesthesia (STA) System, Milestone Scientific is changing the way local anesthesia is being delivered today. Dr Mark Hochman, a ...
Live webinar
Thu. 11 June 2026
1:00 PM EST (New York)
Live webinar
Thu. 11 June 2026
2:00 PM EST (New York)
Prof. Hani Ounsi DDS PhD FICD
Live webinar
Fri. 12 June 2026
8:00 AM EST (New York)
Dipl.-Hdl. Joachim Brandes
Live webinar
Mon. 15 June 2026
11:00 AM EST (New York)
Dr. Cristian Scognamiglio, Dr. Alessandro Perucchi
Live webinar
Tue. 16 June 2026
10:00 AM EST (New York)
Elke Schilling Dentalhygienikerin, B.A. Medical Care Management
Live webinar
Tue. 16 June 2026
7:00 PM EST (New York)
Prof. Dr. Wael Att, Dr. Robert A. Levine DDS, FCPP, FISPPS, AOD, Dr. Victor Astolfi Gonzalez-Mogena ITI Scholar Columbia
Live webinar
Wed. 17 June 2026
8:00 AM EST (New York)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East














































To post a reply please login or register