NEW YORK, N.Y., USA: Eva Grayzel is an unusual late-stage oral cancer survivor: She can speak. Because of that, she feels obligated to tell dentists about their profession’s role in her delayed diagnosis and the heart-wrenching impact the illness had on her and her family. With cases of HPV-related oral cancer on the rise in young people, Grayzel’s message is timelier than ever.
According to the Oral Cancer Foundation, oral cancer will be newly diagnosed in about 100 new individuals each day in the U.S. alone, and because so many of the diagnoses aren’t made until long after the cancer has spread, a person dies from oral cancer every hour of every day.
Grayzel is tireless in her efforts to increase awareness. Her emotional story, which she shares with dental professionals across the globe, helps further her screening-awareness campaign, based at www.sixstepscreening.org.
It’s been 13 years since Grayzel’s diagnosis of squamous cell carcinoma and the radical treatment that took a third of her tongue, her entire left sternocleidomastoid muscle, much of her saliva flow and nearly her life. But it’s her account of how the illness affected her relationship with her two young children that is perhaps the most transfixing. Today, she calls herself lucky, not just because she’s alive and cancer-free, but also because unlike so many late-stage survivors, she literally kept the tip of her tongue, physically enabling her to clearly and passionately articulate her message.
Grayzel spoke with Dental Tribune recently.
Aren’t oral cancer screenings already part of a routine dental checkup?
The American Dental Association’s guidelines say every checkup should include an oral cancer screening. But the guidelines do not say what an oral cancer screening entails, such as how many steps or how long it should take. As a result, some dentists might think they are doing oral cancer screenings, but they may be falling short. Did they pull out the tongue for lateral inspection? Did they feel the palate to see if it was soft and hard in the right places? Did they ask the patient to say “Aah” so they could look at the symmetry of the back of the throat? Did they check the lymph nodes under the chin? Did they feel the neck for enlarged lymph nodes? Did they flip the lips out to look inside the lips and cheeks? That’s all a part of it. If patients don’t get that, they should personally demand it.
With just 3 percent of cancers in the U.S. occurring in the oral cavity and pharynx, why are enhanced awareness and comprehensive screenings by dental professionals so critical?
Oral cancer kills. It's critical that dentists serve their patients right by providing the best care possible. After I was diagnosed, I wanted to know why the heck the dentists I had turned to didn’t know what was staring at them from my lateral tongue. You didn’t need a magnifying glass. You didn’t have to look way back. It was right there, a huge ulceration that was there for months.
Dentists are not mandated to have any continuing education in the early detection of oral cancer, which is dentistry’s deadliest disease. The state of New York is the only exception, requiring one two-hour course to maintain licensure. It's more than critical, it's criminal for dentists not to do screenings properly and thoroughly; to do that they need current education keeping up-to-date in detecting the early signs. The tagline for the Six-Step-Screening campaign is, “If you’re not getting it, ask for it!” If enough patients demand it, dentists will have to change what they know about oral cancer to provide the best care for their patients.
Would mandated C.E. requirements in oral-cancer screening have made a difference in your case?
An optional oral cancer course isn’t a big draw because it doesn’t make money. And dental practices are a business. So when dentists have to choose a course, they typically need to choose a course that will grow their business. But a course on oral cancer is a course that will provide their patients the best care possible and potentially save lives. The ulcer in my mouth was a classic presentation of oral cancer. I could have been diagnosed early if my dentists and oral surgeons knew what they were looking at. At the very least, they should have questioned the initial biopsy. If you are out of dental school 20 years, and haven't taken any C.E. in detection of oral cancer, how can you expect to be up-to-date on lesion recognition?
Do you talk about malpractice in your presentations?
Normally, I don't have time to get into details, but if it is brought up in Q&A, I answer honestly. Yes, there was a malpractice suit. There was negligence no doubt; however, I sued for two main reasons.
First, I didn't want it to happen to someone else, and if they didn't take responsibility for their actions, change wouldn't happen.
Second, I was abandoned as their patient. I want to believe that my dentists and oral surgeons didn't know what to say to me after hearing about my late-stage diagnosis. Therefore, they didn't say anything at all. They never called. I wished they would have said, “I’m sorry this happened to you. Is there anything we can do?” There are many ways to say you’re sorry without admitting guilt.
Your speaking schedule and other efforts look demanding; what motivates you?
I was given a second chance at life. I work hard every day to seek out engagements to share my story with dental professionals. It’s a tribute to those who have come before me and an obligation to those who will follow. And there will be many; the numbers are going up, especially among young people because of the HPV connection. Every time I speak, I save lives. What could be more motivating?
Implants in radiated bone are typically discouraged due to osteoradionecrosis. Do you have implants?
Yes. I was fortunate enough to see a specialist in oncologic dentistry who did a Cone-Beam X-ray and told me my bone was dense enough in places to hold an implant, and I had a window of opportunity to do it. I was told that if bone isn't stimulated it will recede over time, and then I would have no future option for implants. I had three implants in my maximally radiated bone. It's been four years, and they are all successful.
What can dental professionals learn from a survivor?
When dentists hear my story, they say to themselves, “I don't ever want that to happen to any of my patients.” When people feel an emotional connection, they are motivated to change. They want to learn more. They want to get their staffs on board. They are motivated to save lives.
About Eva Grayzel
Eva Grayzel’s background as a performance artist and master storyteller enables her to communicate her experience as a patient and late-stage oral cancer survivor in a unique and powerful way. She shares her intimate and dramatic story at dental meetings and dental schools throughout the world. A champion for early detection, Grayzel created the Six-Step-Screening campaign at www.sixstepscreening.org, for which she was recognized by the American Academy of Oral Medicine. She is the author of “You Are Not Alone: Families Touched by Cancer” and the just published “Mr. C Plays Hide & Seek.”
HOUSTON, US: Because oral cancer is still frequently only diagnosed at an advanced stage, there is a need for adjunctive tools that support early detection ...
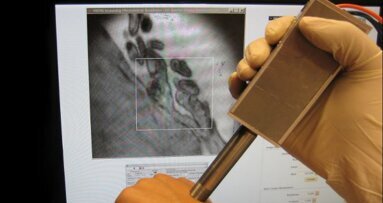
AUSTIN, Texas, USA: In order to reduce the time taken to diagnose oral cancer, researchers have developed the first prototype of a handheld detection device...
VANCOUVER, BC, Canada: Researchers from the University of British Columbia’s (UBC) Faculties of Medicine, Science and Dentistry are leading a US$4.7 ...
Champaign, Ill. & Lubbock, Texas, USA: U.S. researchers have found evidence of bacteria associated with early childhood caries in the saliva of infants ...
MELVILLE, N.Y., USA: Henry Schein Inc. is once again helping raise awareness of the importance of early breast cancer detection and is donating funds to ...
NEW YORK, N.Y., USA: NYU Oral Cancer Center has been awarded a five-year, $3.1 million grant by the National Cancer Institute (NCI), part of the National ...
The gentle touch of a brush on the tongue or cheek can help detect oral cancer with success rates comparable to more invasive techniques such as biopsies, ...
An abnormal immune response or “feedback loop” could very well be the underlying cause of metastases in oral cancers, according to Dr. Marco ...
BALTIMORE, US: Growing evidence suggests that the oral microbiome may influence the development of cancers beyond the oral cavity. In a recent preclinical ...
“Our primary goal as a company is to help save lives,” is how Forward Science cofounder Robert Whitman describes his company’s mission. ...
Live webinar
Wed. 10 June 2026
11:00 AM EST (New York)
Live webinar
Wed. 10 June 2026
2:00 PM EST (New York)
Nacho Fernández-Baca DDS, MSc
Live webinar
Wed. 10 June 2026
7:00 PM EST (New York)
Live webinar
Thu. 11 June 2026
1:00 PM EST (New York)
Live webinar
Thu. 11 June 2026
2:00 PM EST (New York)
Prof. Hani Ounsi DDS PhD FICD
Live webinar
Fri. 12 June 2026
8:00 AM EST (New York)
Dipl.-Hdl. Joachim Brandes
Live webinar
Mon. 15 June 2026
11:00 AM EST (New York)
Dr. Cristian Scognamiglio, Dr. Alessandro Perucchi



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East



















































To post a reply please login or register