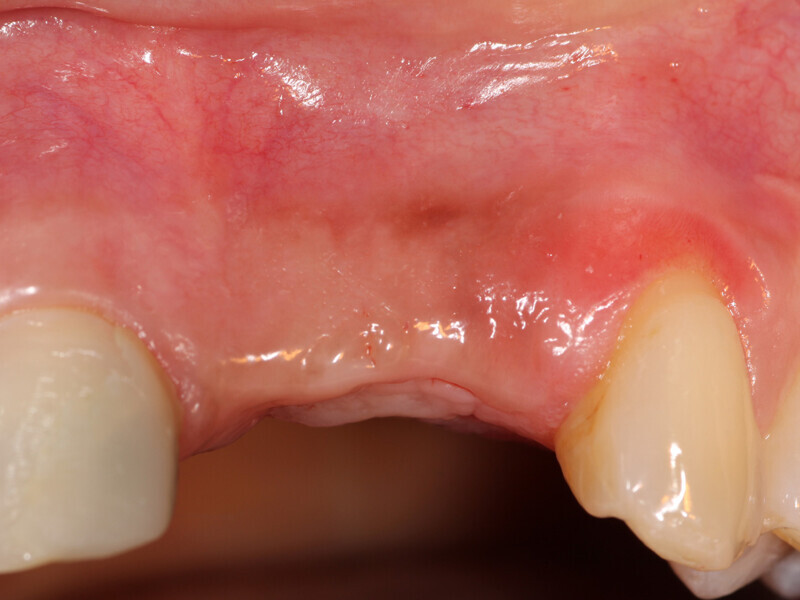
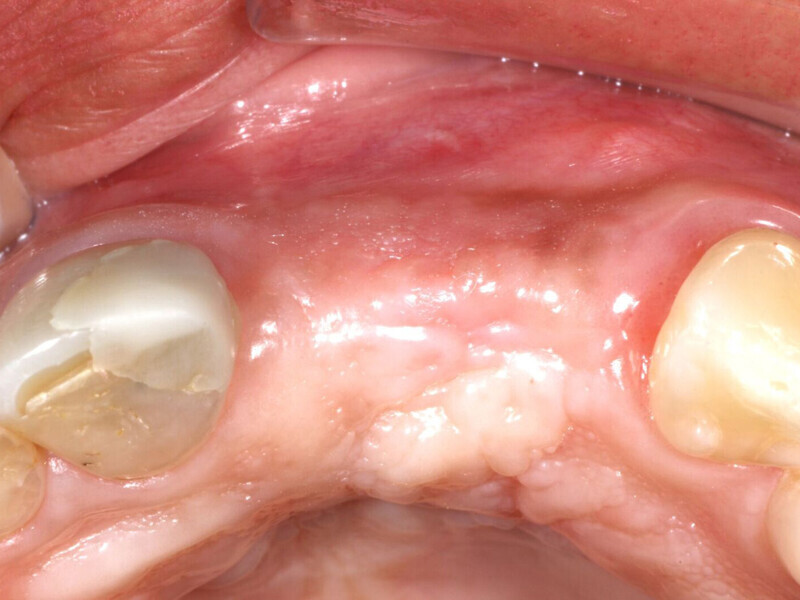
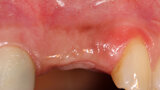
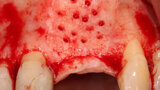
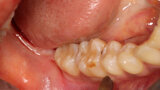
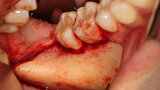
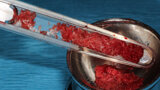
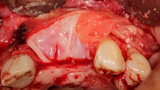
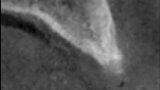
Fig. 1: Deficient facial aspect to the anterior maxilla resulting from resorption following tooth extraction. (Photos provided by Dr. Arun K. Garg; Dr. Gregori M. Kurtzman; Dr. Renato Rossi Jr.; and Dr. Maria del Pilar Rios)
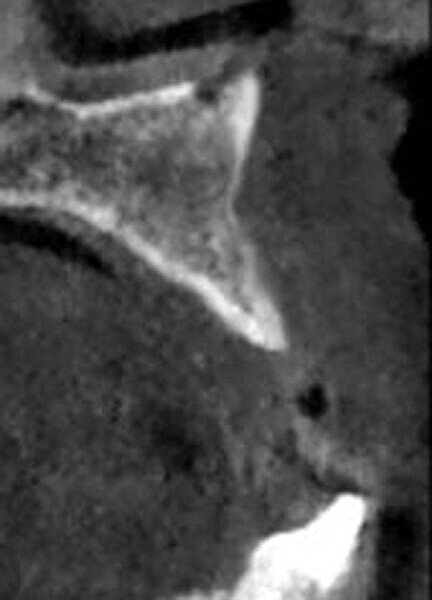
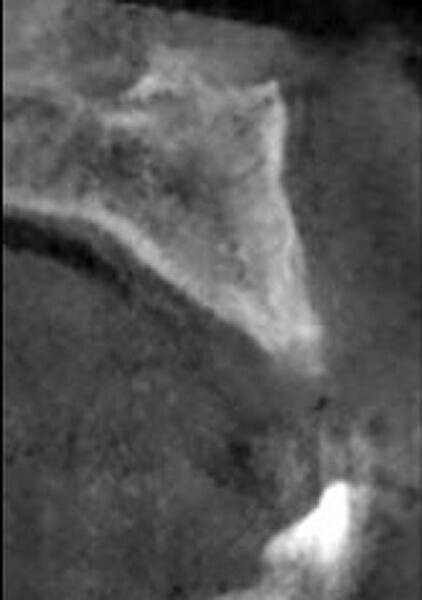
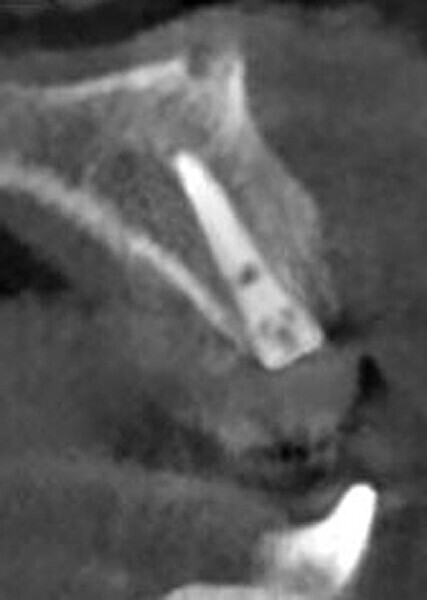
Fig. 2: CBCT cross-section demonstrating insufficient ridge width facial-palatally to permit implant placement in the healed extraction sites.
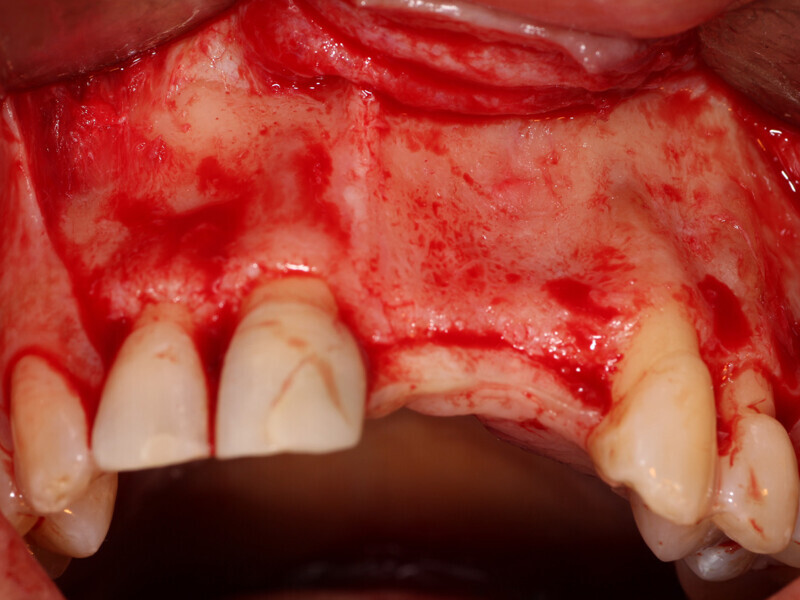
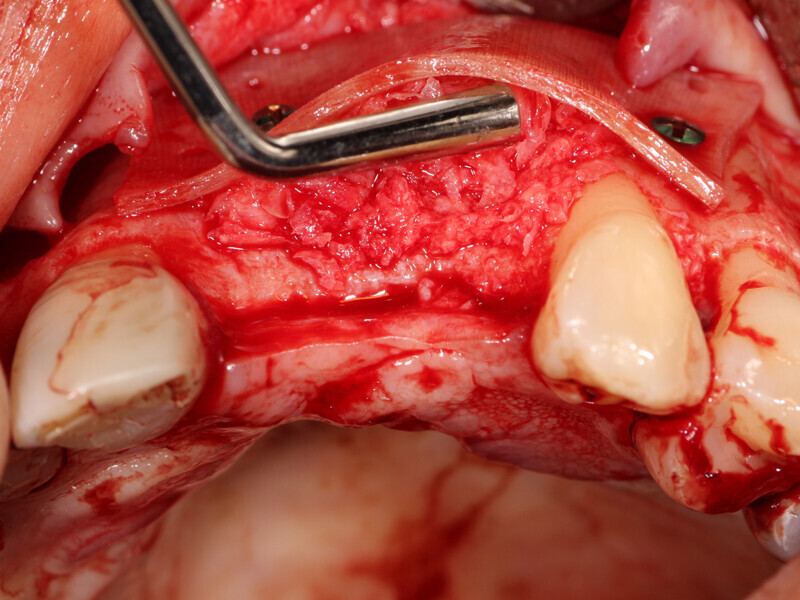
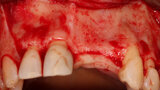
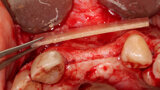
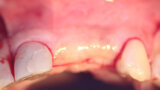
Fig. 3: A full thickness flap was created to expose the deficient facial aspect of the edentulous premaxilla that will receive augmentation to accommodate implant placement.
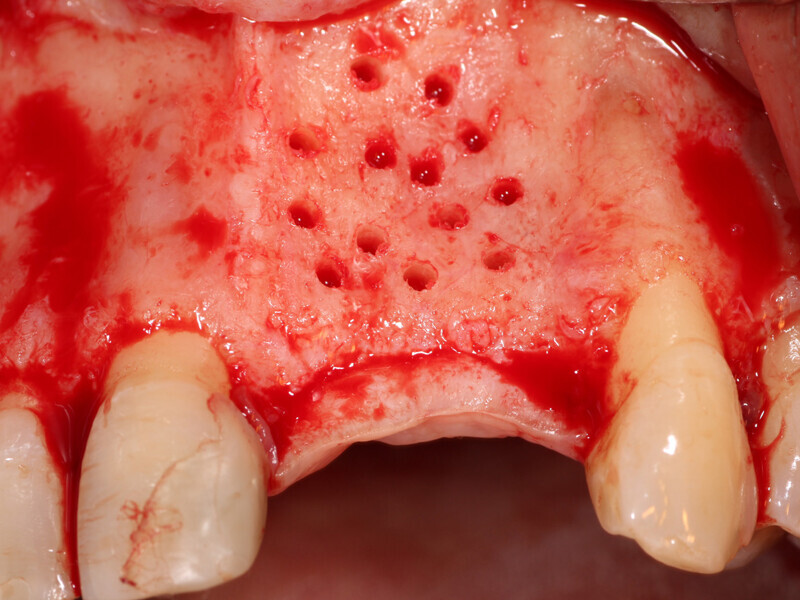
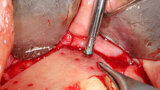
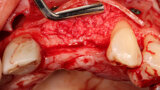
Fig. 4: The facial plate is fenestrated with a bur through the cortical bone in the edentulous space that will receive the osseous graft.
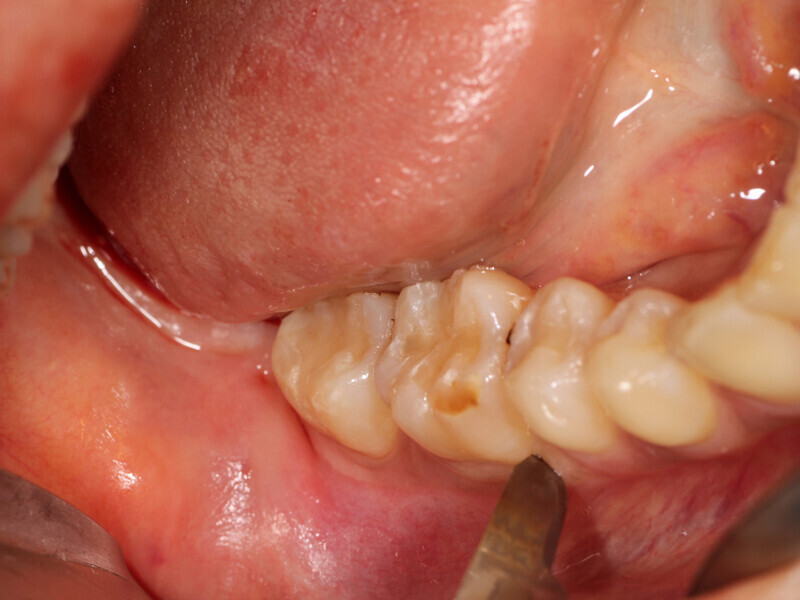
Fig. 5: A vertical releasing incision is made between the first molar and second premolar in the area to be flapped for donor site development in the right posterior mandible.
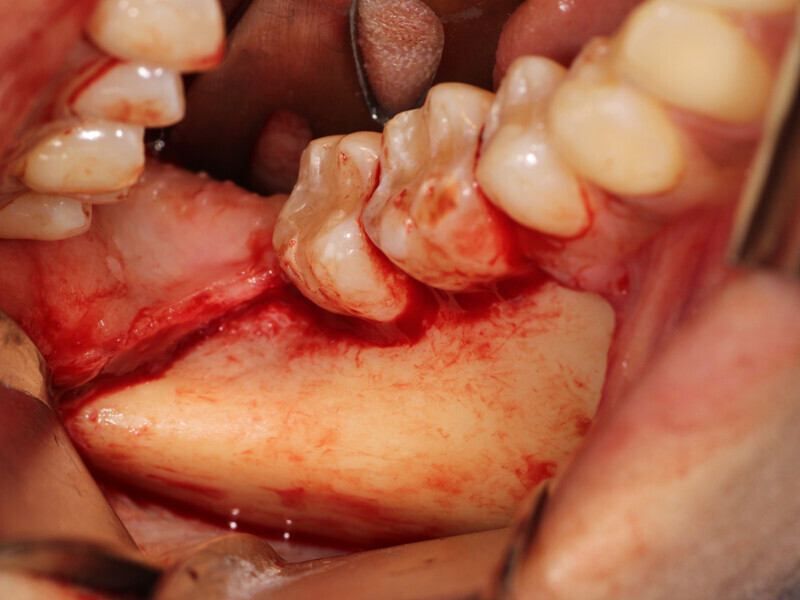
Fig. 6: A crestal incision is made with a sulcular incision to connect to the vertical releasing incision that was created then a full thickness flap is elevated to expose the lateral aspect of the mandibular body that will serve as the donor harvesting site.
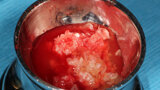
Fig. 7: Autogenous bone that was harvested with the mx-grafter (Maxilon, Hollis, N.H.) from the posterior lateral aspect of the mandible is placed into a sterile mixing dish.
Fig. 8: Buffy coat from the PRP tubes that had been centrifuged is added to the sterile dish containing the harvested autogenous bone and particulate graft material.
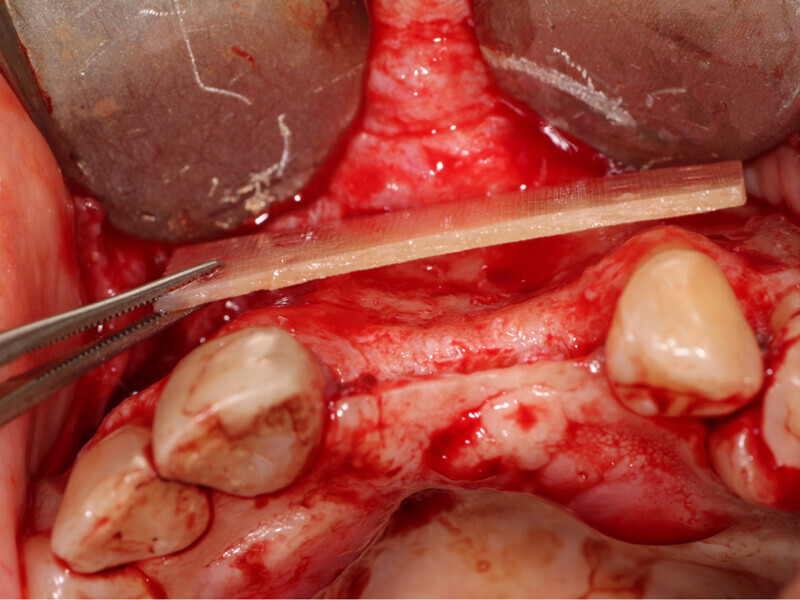
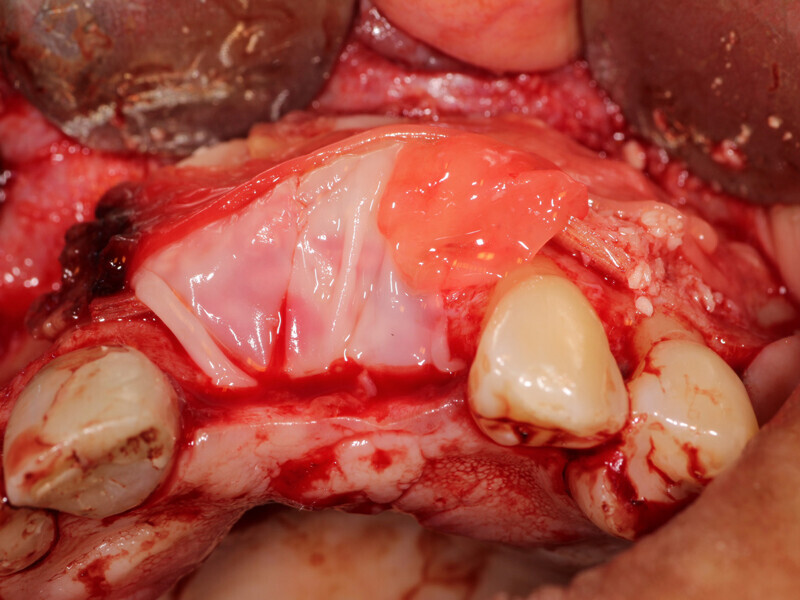
Fig. 9: A 15-by-30-mm piece of Flexo-Plate Plus (Osteolife Biomedical, Jupiter, Fla.) will be placed as the new facial extend of the ridge to contain the graft and act as a mold for the desired ridge augmentation.
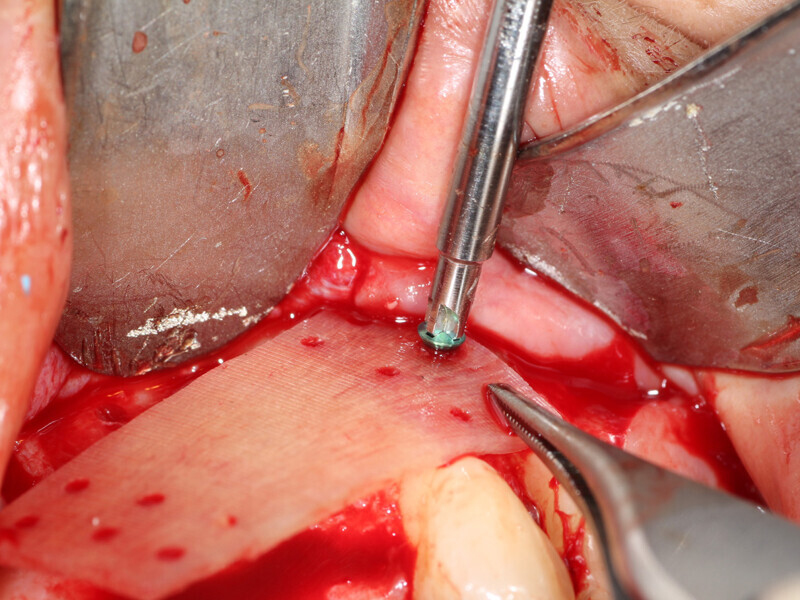
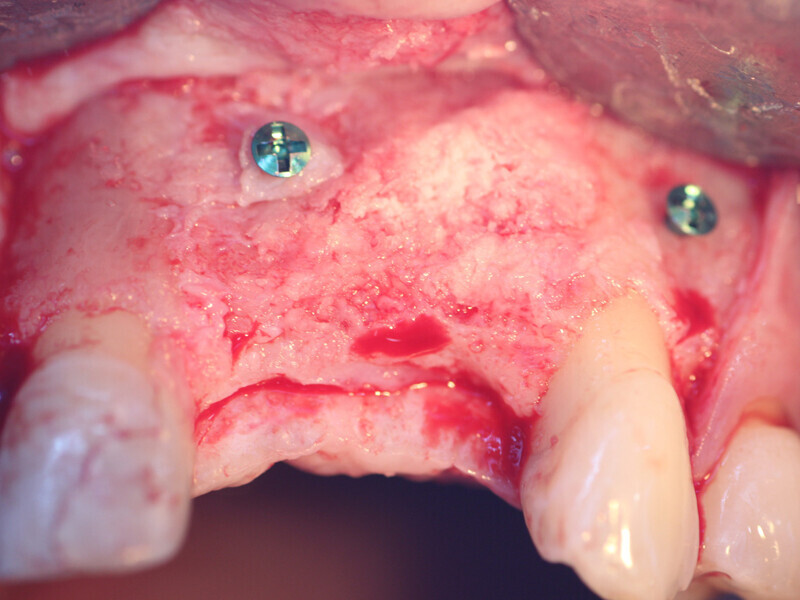
Fig. 10: Holes are placed through the Flexo-Plate Plus and fixation screws are placed to stabilize it on both left and right over the area being grafted.
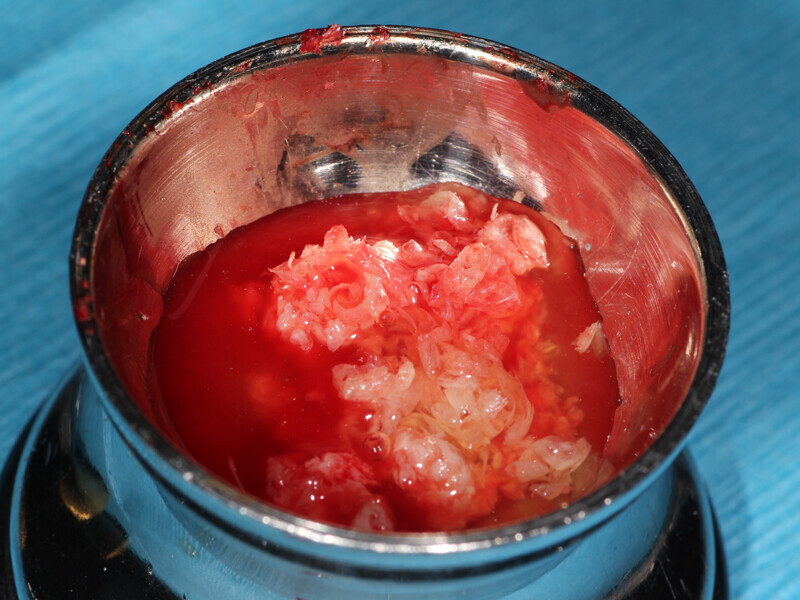
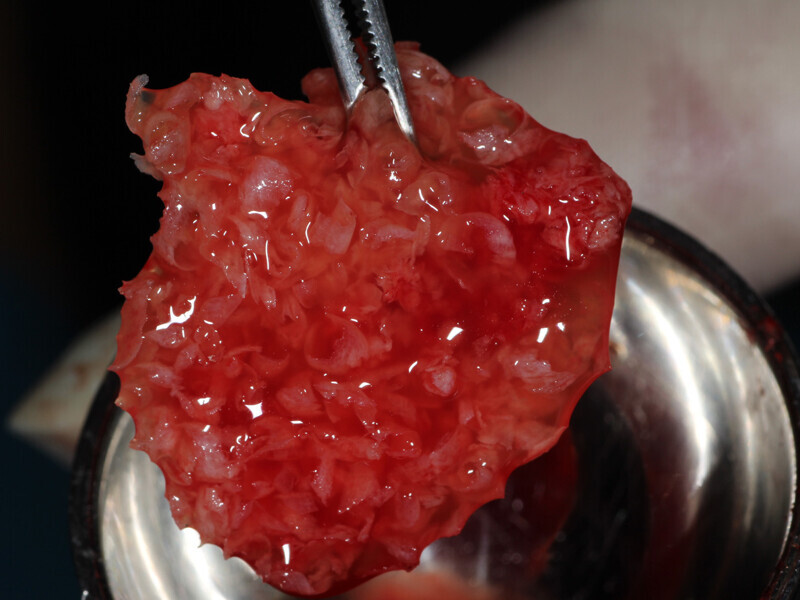
Fig. 11: The ‘gummy bone’ graft material has coalesced into a flexible mass containing the PRP buffy coat, harvested autogenous bone and particulate graft material.
Fig. 12: The PRP autogenous and particulate graft (‘gummy bone’) is placed into the space between the stabilized Flexo-Plate and the deficient edentulous ridge.
Fig. 13: A PRP membrane was placed over the grafted area prior to flap closure as a resorbable long term membrane to prevent soft tissue ingrowth as the osseous graft heals and matures.
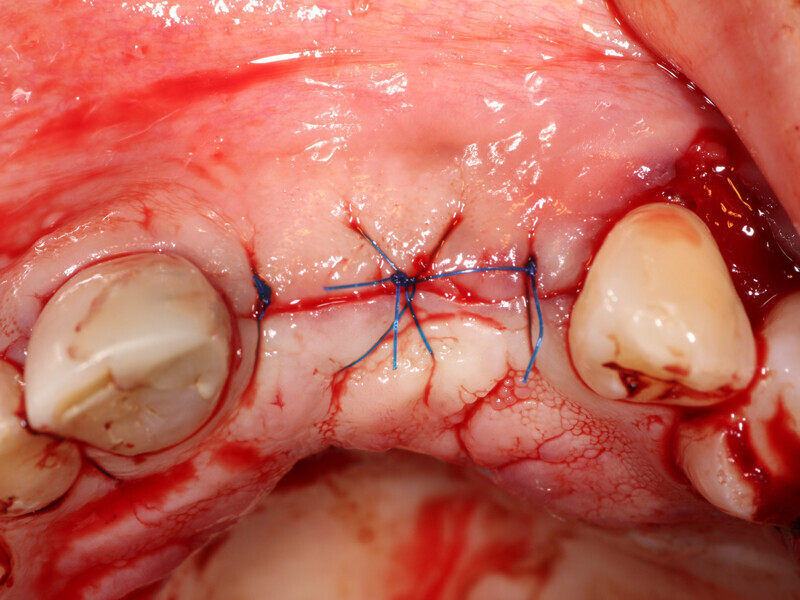
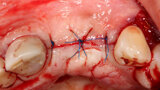
Fig. 14: Flap is closed without tension using 5-0 Polypropylene suture (Riverpro, Osteolife Biomedical, Jupiter, Fla.) in a simple interrupted pattern.
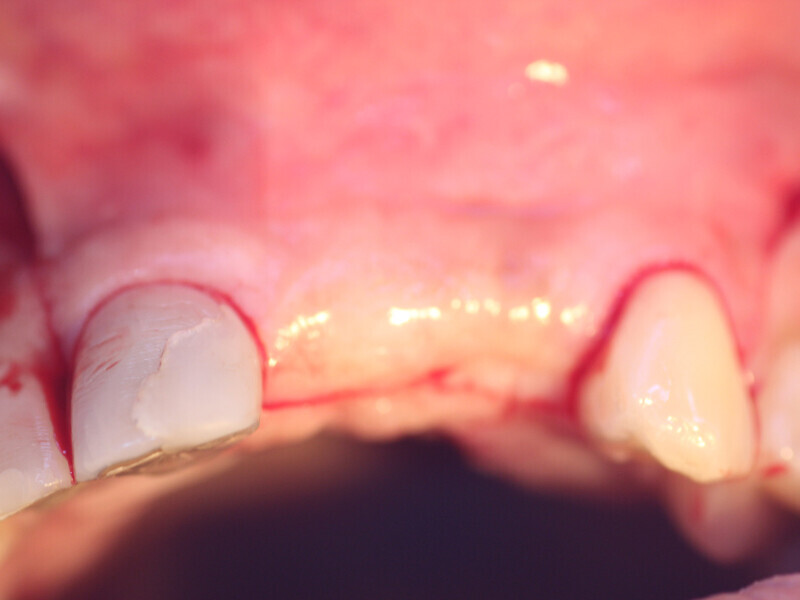
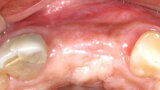
Fig. 15a: The previously deficient ridge at the left central and lateral incisors resulting from resorption following the previously extracted teeth had been augmented and is ready for implant placement following 4.5 months of graft healing.
Fig. 15b: The previously deficient ridge at the left central and lateral incisors resulting from resorption following the previously extracted teeth had been augmented and is ready for implant placement following 4.5 months of graft healing.
Fig. 16: CBCT cross-section of the grafted facial aspect of the deficient ridge demonstrates adequate width for implant placement following healing of the graft at 4.5 months.
Fig. 17: The healed grafted ridge at 4.5 months following flap elevation demonstrating adequate width facial-palatally to allow implant placement.
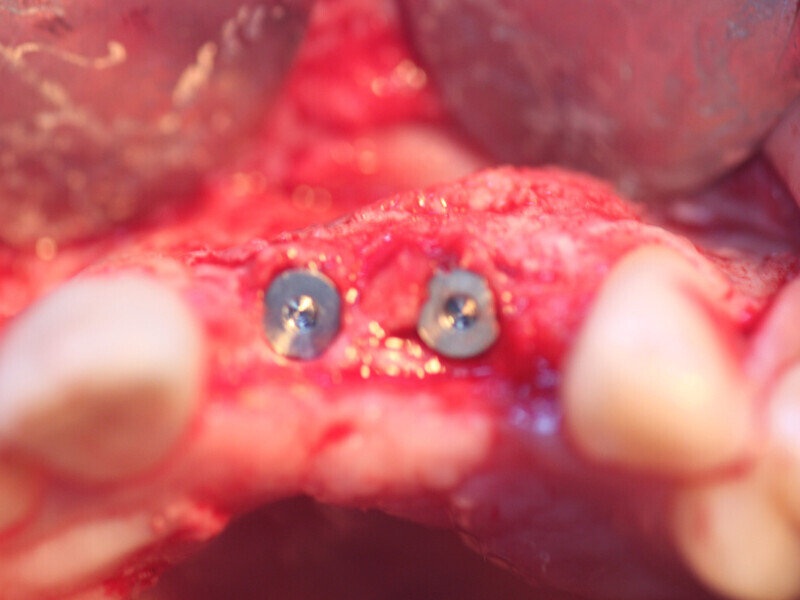
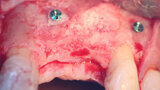
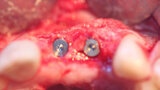
Fig. 18: Implants have been placed into the grafted previously deficient ridge showing adequate bone to house the implants and a lack of dehiscence on the facial aspect, shown prior to flap closure.
Fig. 19: CBCT cross-section following implant placement demonstrating adequate width to house the implant and sufficient facial plate thickness.
Renato Rossi Jr., DMD, MSc, PhD
Maria del Pilar Rios, DMD, MSc, PhD



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East