If used appropriately, bisphosphonates are a tremendous tool in treating osteoporosis. There is currently a great deal of confusing information over when and how to safely use them. Clearing up the confusion is important because more than 30 million people in the United States are currently suffering from osteoporosis, and if they are not treated, they are at risk for osteoporotic fractures that seriously jeopardize their lives.
At present, bisphosphonates are the best tool to reduce bone loss and significantly reduce the chance of these fractures. It is estimated that 24 percent of patients with osteoporotic fractures not treated by bisphosphonates will die because of these fractures.
embedImagecenter("Imagecenter_1_278",278, "large");
Recently, reports of osteonecrosis of the jaw (ONJ) associated with bisphosphonates have caused fear about using bisphosphonates. The reports by Dr Marx and later by Dr Ruggerio related osteonecrosis lesions after oral surgical procedures were done on patients in hospitals under IV bisphosphonate administration.
This article seeks to clarify some of the unknowns, or innuendo, surrounding the fear of using bisphosphonates. As it was once wisely written: “We have nothing to fear but fear itself.”
Identifying the problem
Today we have acquired fear about using certain medication for osteoporosis. Namely, bisphosphonates and their relationship to osteonecrosis. Osteonecrosis is defined as the death of bone tissue due to an impaired blood supply. When the diagnosis of osteonecosis is made, the cause is listed as definite causes and possible causes.
Definite causes includes: alcohol abuse, atherosclerosis, decompression sickness, Guacher’s disease, high doses of corticosteroids, radiotherapy, sickle cell disease and tumors.
Possible causes include: blood clotting disorders, Cushing’s syndrome, diabetes mellitus, fatty liver, gout, lipid disturbances, pancreatic cancer, pancreatitis, smoking, systemic lupus and erythematosis.
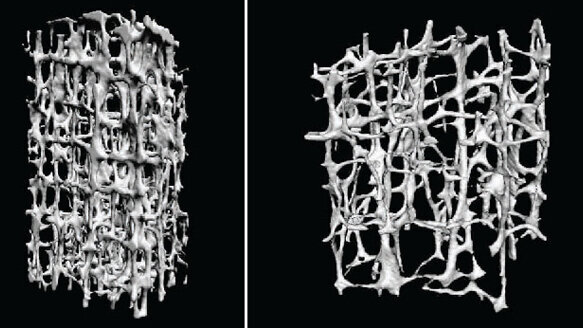
Brittle bones and fractures are more prevalent as the population lives longer. It is estimated that 20 to 30 million people have concerns about their osteoprosis and are taking medications to cease or prevent their osteoporosis. The medications to aid opsteoporosis are in general called bisphosphonates.
When clinical reports of associations of bisphosphonates to osteonecrosis were distorted, it started a reaction that caused people to associate all bisphosphonates and all levels of strengths and dosages in one grouping. It is as if one were to claim all antibiotics are the same and only one strength were to be used for all instances.
There is a benefit to being made aware by Marx and Ruggerio, and now drug makers are also aware of the possibility of ONJ and include this information in their listing of possible side effects for bisphosphonates.
However, the result of this information has also caused people to hesitate in their efforts to prevent or inhibit osteoporosity. Suddenly, lawyers have come to the fore who claim to specialize in representing patients using bisphosphonates who wish to instigate a lawsuit and actually advertise to acquire plaintiffs who have been harmed by using bisphosphonates.
In addition, some physicians now hesitate to prescribe bisphosphonates for fear of legal consequences, leaving the patient to deteriorate further.
Oral surgeons at dental meetings are also showing more osteonecrotic lesions in their presentations. However, the causes of these necrotic lesions are not necessarily from bisphosphonates.
Clinical reports of osteonecrosis associated with bisphosphonates was brought to dentists’ awareness by oral surgeons (Marx and Ruggerio) some 30 years after the use of bisphosphonates were first released to the public and received FDA approval.
Oral bisphosphonates were first approved and released in 1970, and clinical reports of oral necrosis were published after 2003. The clinical reports independently provided proof of oral necrotic bone lesions resulting when treating patients in hospitals that were under some regime and hospitalized.
Only after oral surgical therapy, while in the hospital, these patients presented necrotic oral lesions and their sequela.
While I do appreciate the reporting of such information and now avoid having patients acquire further trauma, I found myself asking: “What were these patients doing in a hospital environment to begin with?” As reported, the patients were all hospitalized for cancer therapy and undergoing chemotherapy. Their resistance factors certainly may, under those circumstances, be altered.
The method of receiving bisphosphonates while being treated in a hospital was not, as most commonly accepted, orally, but rather intravenously.
Intravenous bisphosphonates have been used for Paget’s disease, hypercalcemia associated with malignancy and with antineoplastic bone lesions associated with breast cancer and multiple myeloma. The strength and dosages of the medication used with the IV was close to four times the recommended oral dosage.
There are, of course, protocols for treating hospitalized patients, and they were all followed. Yet, these reports are being interpolated to encompass all modes of bisphosphonates delivery systems.
However, there are positive results from using oral bisphosphonates when administered at the proper dosage. Emphasis must be placed upon differentiating the reported results from all intravenous delivery of bisphosphonates as well as the recognition of different dosages.
In my practice, I have patients who are taking oral bisphosphonates. I treated them for periodontal disease with surgical intervention with positive results over the years.
The same goes for patients that continued taking their oral bisphosphonate medication when I placed implants and achieved successful results.
Dr M. Jeffcoat reported a three-year study comparing patients taking oral bisphosphonates with non-medicated patients. Each group received the same number of implants inserted. The results were the same for each group: approximately a 98 to 99 percent acceptance.
The millions of patients that have osteoporosis and need assistance are the ones that we are trying to aid, not deter. Let our profession encourage and inform patients of all the facts pertaining to bisphosphonates. Indeed, I have apprehensions of unknown possibilities for those taking various medications.
As such, in the case of oral bisphosphonates, what might be the accumulative effects of taking this medication for five or 10 years?
A recent report from University of Southern California showed a 96 percent success rate of people using oral bisphosphonates with osteoporosis. A new acronym for bisphosphonate-associated osteonecrosis, BON, has become popular in discussions.
It behooves us to share this knowledge with our patients. In particular, we must clearly note the difference in administration of bisphosphonates via an IV or orally when discussing the use and safety of these drugs.
So-called “drug holidays” are not the answer. There is no supporting data that stopping the use of bisphosphonate medication for a set amount of time reduces the risk of developing BON.
Perhaps standardizing a bone turnover marker test and getting a base line of bone metabolism, a DTX information gathering radiograph — definitely as the American Dental Association suggests with osteoporosis — and trying to avoid oral pathology by undergoing regular oral examinations by a dentist and increasing good oral hygienic techniques by using power toothbrushes or hand toothbrushes, and avoiding alcohol rinses would decrease risk.
There are millions of people who need, or will need, treatment for osteoporosis. Let us help ourselves with knowledge, not fear. Let us start by recognizing the different administartion methods, oral as opposed to IV, as well as their dosage differences.
Perhaps with knowledge and statistical studies we can help eliminate this fear.
About the author
David L. Hoexter, DMD, FACD, FICD is director of the International Academy for Dental Facial Esthetics, and a clinical professor in periodontics at Temple University, Philadelphia. He maintains a practice in New York City limited to periodontics, implantology and esthetic surgery. He can be reached at drdavidlh@aol.com.
Editorial note: This article was originally published in Dental Tribune U.S. Edition, Vol. 6 No. 5, March 2011.
Controversy involving the oral cavity and the effects of using bisphosphonates is causing an obstacle for dentists to help patients achieve optimal health. ...
NEW YORK CITY, N.Y., USA: The results of a study conducted at the New York University College of Dentistry seem to confirm the hypothesis that the use of ...
NEW YORK CITY, N.Y., USA: Results derived from a study conducted at the University of New York College of Dentistry seem to confirm the assumption that the ...
WASHINGTON, US: Covering everything, including composite fillings and disposable suction tips, plastics are woven into all aspects of modern dental care. ...
CHICAGO, IL / NEW YORK, NY, USA: The Academy of General Dentistry (AGD) recently announced that 326 dentists have earned its prestigious Fellowship and ...
CHICAGO, Ill., USA: The Academy of General Dentistry (AGD) recently announced that 302 dentists earned the AGD’s prestigious Fellowship and Mastership...
CHICAGO, IL, USA: The Academy of General Dentistry (AGD) recently announced that 435 dentists have earned the AGD’s Fellowship and Mastership awards, ...
The American College of Prosthodontists is taking Southwest Florida by storm from Wednesday through Saturday. The JW Marriott Marco Island will host this ...
For dental professionals, delivering predictable aligner outcomes continues to be a challenge — especially when patient compliance is inconsistent. Even ...
A patient who is happy with his or her smile will ultimately be a more compliant patient. One of the easiest and most significant methods to achieving an ...
Live webinar
Wed. 3 June 2026
1:00 PM EST (New York)
Live webinar
Thu. 4 June 2026
2:00 PM EST (New York)
Live webinar
Mon. 8 June 2026
12:00 PM EST (New York)
Live webinar
Mon. 8 June 2026
1:00 PM EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 PM EST (New York)
Live webinar
Wed. 10 June 2026
11:00 AM EST (New York)
Live webinar
Wed. 10 June 2026
2:00 PM EST (New York)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East



















































To post a reply please login or register