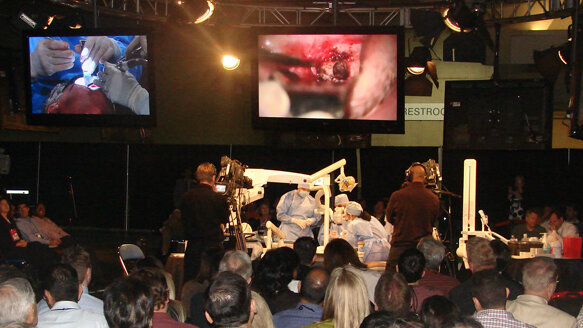
SAN DIEGO, USA: The first live demonstration of a cutting-edge endodontic surgical procedure was presented at the American Association of Endodontists’ annual scientific session. Performed by Dr L. Stephen Buchanan, the experimental procedure — CT-guided endodontic surgery (GES) — used SimPlant surgical treatment planning software to plot an ideal path to the diseased MB root and bone of an upper first molar.
It was followed by the digital fabrication of a SimPlant drill guide to transfer the treatment planned in computer space to the patient’s jaw.
While this drilled guide software has been used successfully for many years in implant dentistry, it has not been previously used for endodontic surgery. The presentation was made on Friday, 16 April.
Dr Buchanan said he became familiar with guided surgical concept as he trained to do implant surgery. His friend, the late Dr David Rosenberg, to whom he dedicated this procedure, taught him how drill guides can greatly improve surgical speed and accuracy during implant placement, so when a graduate student at UCLA asked if CT-generated drill guides could work for endodontic surgery, he said his whole concept of endodontic surgery changed. Surprisingly, upon doing a literature search, Dr Buchanan found out this concept was first brought into the public domain in 2007.*
For the several hundred endodontists who watched this live demonstration, it was clear this was not yet a more efficient procedure. The potential, however, was clearly evident.
Perhaps the most time-consuming part of the demonstration was the placement of a screw-fixated retraction fence he designed, but once the two 1.5 mm bone screws were set, retraction of the mucosa overlying the drill path required no more effort on Buchanan’s part.
He noted that inefficient tissue retraction is probably the biggest barrier to dramatically shorten surgical times, and this aspect of GES is obviously a work in progress.
Despite the challenge of placing the retraction fence and dealing with significant bleeding (the patient has high blood pressure), drilling through the guide, to length, with the 2, 3, 4 and 5 mm drills was very straightforward.
After the drill guide was removed, Buchanan captured a micro-mirror view through the resulting 5 mm drill hole — showing the MB root cut perfectly with the previously treated MB1 canal bisected and beyond it, toward the palatal aspect, a darkened isthmus that led directly to the previously untreated MB2 canal.
He then negotiated and enlarged the MB 2 canal through the resected root end using .04 tapered rotary NiTi files in sizes 15–40. He said the .04 taper limitation reduced the accumulation of cyclic fatigue caused by the flexure of the files past the cut root surface, allowing him to cut a larger diameter of preparation to the coronal extent of the canal than would have been possible with more tapered instruments.
Filling this canal created some additional challenges; however, Buchanan was able to accomplish that with a pressure syringe loaded with pink Cavit and a 27-gauge needle, resulting in a dense fill all the way to the pulp chamber. Buchanan typically uses Cavit because: A) it sets in the presence of moisture, B) it seals against leakage as good as MTA, and C) its viscosity allows it to be syringed quite a distance from the end of the needle.
An alternative he’s been experimenting with has been filling apically instrumented canals with a carrier-based obturator. While early results look good (excellent fills and much less time and frustration), he chose to do the more familiar technique — perhaps for the last time.
Following the fill of the MB2 canal, Buchanan brought in one of his newest ultrasonic tip designs, which he refers to as an Isthmus Hatchet (IH). Three millimeters in length, 0.4 mm wide, with acute angles on each end, the IH (Spartan) literally dropped down into the root through the center of the isthmus, resulting in a very smooth, straight-walled, retro preparation.
The apical retro seal was done with gray ProRoot MTA (Dentsply Tulsa) because Dr Buchanan likes the handling characteristics more than the white MTA used in esthetic areas.
The MTA was delivered with Tulsa’s MTA tube carrier/condensers in 5–6 aliquots and it was condensed with a hatchet plugger (HP) made to fit the prep the IH makes. A conventional digital radiograph confirmed a dense retro fill, and the minimally-invasive flap was sutured with four 5-0 Supramid sutures.
Next, a CT scan was done with a J. Morita Veraviewepocs 3De cone-beam CT machine showing the final result with the MB2 canal and the apical preparation densely and completely filled.
When attendees were asked their opinion of the demonstration and the new GES procedure, the most consistent response was firstly that Buchanan showed a lot of courage doing an experimental procedure in front of his peers, and secondly, although it is not there yet, the potential benefits of guided endodontic surgery are many.
What’s next for Dr Buchanan and the engineering team at Materialise? The next six to 12 months will be spent treatment planning and performing the hundreds of procedures needed to bring this procedure successfully into the mainstream of clinical endodontics, as well as setting up university-based research projects to bring GES into peer-reviewed literature.
At this point, Dr Buchanan said, “The iterative design process will take this from a fascinating but slow way to do endodontic surgery, to an elegant procedure that is much faster, much more precise and that requires less training than traditional methods.”
L. Stephen Buchanan, DDS, FICD, FACD maintains a private practice limited to endodontics and implant surgery in Santa Barbara, CA, USA, and is the founder of Dental Education Laboratories.
*Pinsky H., Champleboux G., Sarment, D., Periapical Surgery Using CAD/CAM Guidance: Preclinical Results., J Endod 2007; 33:148-151
Guided surgery for implant placement provides great benefits for clinicians but can also create complications. Because of this dichotomy, some dentists shy ...
ALBUQUERQUE, N.M., USA: OCO Biomedical will showcase its newly introduced Guided Surgery Kit, which features the world’s first two-step guided surgery...
OCO Biomedical, a global leader in world-class dental technology, training and instrumentation, will highlight its guided surgery kit, which features the ...
CHICAGO, Ill., USA: In a recent statement, the American Association of Endodontists (AAE) announced that it is strong in its stance that, amid a potential ...
CHICAGO, Ill., USA: As the global leaders in advocating the value and quality of endodontics, the American Association of Endodontists (AAE) supports a ...
ALBUQUERQUE, N.M., USA: OCO Biomedical, a company recognized for its dental technology, training and instrumentation, will showcase its Guided Surgery ...
BOLOGNA, Italy: Under the theme “Tradition and innovation of retentive systems”, Italian dental manufacturer Rhein’83 held its first ...
ORLANDO, FL, USA: Many companies launched new products at the 2009 Annual Session of the American Association of Endodontists. The meeting, which was held ...
AAE21, the annual meeting of the American Association of Endodontists, will take place April 21 to 24 (Wednesday through Saturday). The event is being ...
NEW ORLEANS, La., USA: In what will certainly be considered a highlight of AAE17, two live endodontic microsurgeries — one mandibular, one maxillary ...
Live webinar
Wed. 3 June 2026
1:00 PM EST (New York)
Live webinar
Thu. 4 June 2026
2:00 PM EST (New York)
Live webinar
Mon. 8 June 2026
12:00 PM EST (New York)
Live webinar
Mon. 8 June 2026
1:00 PM EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 PM EST (New York)
Live webinar
Wed. 10 June 2026
11:00 AM EST (New York)
Live webinar
Wed. 10 June 2026
2:00 PM EST (New York)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East



















































To post a reply please login or register