By far the most frequently asked question in every orthodontic office is, “When are my braces coming off?” In the fast-paced, busy lives of patients, there is little time to spend on lengthy orthodontic therapy. In the ever-advancing field of orthodontics, many barriers have been overcome, leading to healthier results and more beautiful smiles. Now, the focus is on reducing treatment time (Proffit, 2013).
Faster care without sacrificing quality would be advantageous in (a) reducing hygiene problems, (b) increasing patient acceptance of treatment plans and (c) creating a higher level of overall treatment satisfaction.
This new focus can be seen through the development of techniques such as the accelerated osteogenic orthodontics known as Wilckodontics, and the micropulse technology seen in AcceleDent (Kau, 2011). With the emphasis on shortening treatment time, it is critical that practitioners be aware of all medications that patients are taking that could unknowingly slow down their orthodontic treatment.
This must be accomplished by thorough evaluation of the patient’s medical history with close attention to medications, including over-the-counter analgesics. Various analgesics taken by patients during orthodontic treatment, including traditional non-steroidal anti-inflammatory drugs, aspirin and acetaminophen, have been scientifically shown to decrease the rate of tooth movement (Tyrovola, 2001).
Mechanism of tooth movement
Orthodontic tooth movement is mediated by specific reactions at a cellular level that take place in the tissues surrounding teeth. Cellular, chemical, and mechanical reactions bring about the structural changes that prompt tooth movement. Bone is resorbed on the pressure side and deposited on the tension side of a tooth. An acute inflammatory response with periodontal vasodilation occurs.
Cyclic adensine monophosphate (cAMP), calcium, collagenase and prostaglandins mediate tooth movement as a response to orthodontic force. Chemicals in drugs taken by patients can pass through the bloodstream, reach the mechanically stressed tissues, and interact with local cells. This can have an inhibitory effect on orthodontic tooth movement (Diravidamani, 2012).
Orthodontic patients often use over-the-counter analgesics to control the discomfort associated with tooth movement as well as to treat other ailments (Salmassian, Oesterle, Shellhart & Newman, 2009). Many of these pharmaceutical agents are known to systemically influence bone and the velocity of tooth movement by interfering with prostaglandin production and the inflammatory process.
The pressure-tension theory describes tooth movement occurring in three stages, “alterations in blood flow associated with pressure in the periodontal ligament (PDL), formation or release of mechanical messengers, and activation of cells” (Salmassian, et al., 2009).
After force is applied, there is an increase of prostaglandin E and interleukin-1 B levels in the PDL and gingival crevicular fluid. This is a critical step in increasing the number of osteoclasts, the rate bone resorption and orthodontic tooth movement, and is the step that is affected by NSAID medication (Salmassian, et al.).
Process of orthodontic tooth movement
In order to appreciate how NSAIDs can affect the rate of orthodontic tooth movement, one must first understand the complex process. Tooth movement due to orthodontic forces is induced by prolonged application of mechanical forces, creating pressure and tension zones in the periodontal ligament and alveolar bone (Gameiro, Pereira-Neto, Magnani & Nouer, 2007).
Bone is deposited on the alveolar wall in the tension zone and resorbed by osteoclasts in Howship’s lacunae in the pressure zone (Knop, Shintcovsk, Retamoso, Ribeiro & Tanaka, 2011). Remodeling occurs in dental and paradental tissues, including dental pulp, periodontal ligament, alveolar bone and gingiva. These tissues, when exposed to mechanical loading, express significant macroscopic and microscopic changes.
On a cellular level, orthodontic tooth movement is characterized by initial acute inflammation, followed by a chronic inflammatory process (Krishnan & Davidovich, 2006). The acute inflammatory process that characterizes preliminary orthodontic tooth movement consists of periodontal vasodilation and migration of leukocytes. This inflammation is mainly exudative, indicating that the plasma and leukocytes are exiting the capillaries in areas of paradental strain.
These migratory cells produce a variety of cytokines that act as local biochemical signals, interacting directly and indirectly with the population of resident paradental cells. Cytokines are responsible for evoking subsequent biological events and bone remodeling which accommodate tooth movement (Knop, et al., 2011). These target cells make up the functional units that are responsible for remodeling the paradental tissues while facilitating tooth movement (Krishnan & Davidovich, 2006).
Approximately two days following application of orthodontic force, the acute phase of inflammation subsides. It is replaced by a chronic, proliferative process involving fibroblasts, endothelial cells, osteoblasts and alveolar bone marrow cells. During this time, leukocytes will continue to migrate into strained paradental tissues, modulating the remodeling process. This chronic inflammation will persist until the next orthodontic adjustment appointment when another period of acute inflammation will begin. (Krishnan & Davidovich, 2006).
It is during the acute inflammatory phase of orthodontic tooth movement that patients experience painful sensations and reduced chewing function. Ninety to ninety-five percent of orthodontic patients report experiencing this discomfort (Patel, et al., 2010). Indications of this phenomenon can be seen in the gingival crevicular fluid of moving teeth by significant elevations of inflammatory mediators such as cytokines and prostaglandins (Krishnan & Davidovich, 2006).
The discomfort associated with orthodontic tooth movement in patients can be decreased by inhibiting inflammation. NSAIDs are thus a viable option. However, because they inhibit prostaglandin synthesis, the rate of tooth movement may be affected because inhibition of prostaglandins prevents activation of osteoclastic cells that induce bone resorption (Sari, Olmez, & Gurton, 2004).
It would be appropriate for clinicians to understand this effect of NSAIDs so that they can take heed to prescribe or suggest a pain medication that has minimal effect on prostaglandin synthesis. This is also important in order to prevent prolonged orthodontic treatment time, which could lead to increased dental health risks.
Prostaglandins and NSAIDs
Many studies have confirmed that prostaglandins are critical mediators of the inflammatory process that allows for orthodontic tooth movement through their ability to increase vascular permeability and dilation (Sari, Olmez, & Gurton, 2004). Studies show that injecting exogenous prostaglandins enhances the amount of tooth movement (Bartzela, Turp, Motschall & Maltha, 2009).
Prostaglandin synthesis in humans is catalyzed by two forms of cyclooygenase (COX): COX-1 and COX-2. COX-1 is present throughout the body and has physiologic functions such as vascular hemostasis and maintenance of the normal gastric mucosa. COX-2, on the other hand, is regulated by inflammatory mediators, and creates prostaglandins that play a role in pathophysiological and inflammatory processes including pain.
Studies have also found that these prostaglandins not only mediate inflammation, but also participate in bone formation and induction of bone resorption through activation of osteoclastic cells (Sari, et al., 2004). Specifically, it is believed that they are responsible for increasing the number of osteoclasts through enhancement of their ability to form a ruffled border, thus effecting bone resorption (Krishnan & Davidovich, 2006). Prostaglandins also stimulate osteoblastic differentiation and new bone formation (Knop, Shintcovsk, Retamoso, Ribeiro & Tanaka, 2011). Therefore, prostaglandins play a significant role in mediating orthodontic tooth movement.
The discomfort associated with archwire placement and subsequent tooth movement can be controlled by inhibiting the inflammatory response. This makes nonsteroidal anti-inflammatory drugs a logical choice for treating this type of pain. However, NSAIDs are also powerful inhibitors of prostaglandin synthesis, which recent studies have shown to be responsible for delaying or inhibiting orthodontic tooth movement.
This area of research is critical to the field of orthodontics because it is important for orthodontists to be aware of in order to find the analgesic of choice for treating patients experiencing dental discomfort that will not prolong the patient’s orthodontic treatment. The orthodontist can then educate his or her patients on proper pain management during treatment.
Clinical studies on effects of various analgesics on orthodontic tooth movement
Nonsteroidal anti-inflammatory analgesics such as aspirin, ibuprofen and naproxen have been found to reduce the rate of orthodontic tooth movement. Research shows these effects result from diminishing the number of osteoclasts through inhibition of biosynthesis of prostaglandins when they act over the cyclooxygenase mediated catabolism of arachidonic acid (Arias & Marquez-Orozco, 2006).
When the number of osteoclasts are diminished, there is a decrease in bone resorption and therefore a reduction in the rate of tooth movement. Histological studies were performed comparing bone in the pressure zone from rats undergoing orthodontic tooth movement that had been administered these drugs, with those that have received acetaminophen or a control.
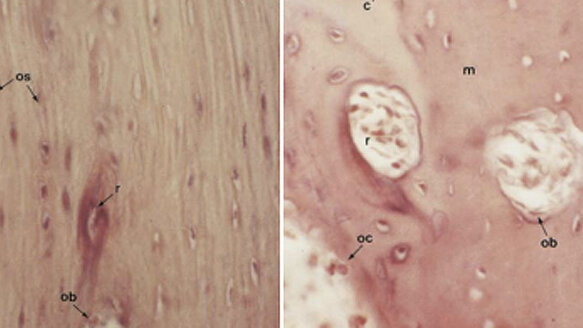
The NSAID administered bone (Fig. 1) showed less remodeled areas, few and smaller osteoblasts, indistinguishable osteclasts in the pressure region, abundant parallel layered osteocytes, reduced Howship lacunae (Knop, et. al., 2011), and no observed growth lines (Arias & Marquez-Orozco, 2006).
The control and acetaminophen group (Fig. 2) showed abundant remodeled areas, distinguishable multinuclear osteoclasts, mesenchymal appearing osteogenic cells, epithelial osteoblasts, and normal appearing trabeculation. Numerous growth lines were also apparent, typically concentric around osteons. The results of the histological analysis of the acetaminophen and control groups are indicative of normal, uninhibited orthodontic tooth movement (Arias & Marquez-Orozco, 2006).
embedImagecenter("Imagecenter_1_813",813, "large");
Acetaminophen as the drug of choice
Acetaminophen is a nonopiod analgesic in the family of paraminophenols. The exact mechanism of action of acetaminophen has not been determined. Acetaminophen differs from other nonsteroidal anti-inflammatory drugs and prostaglandin inhibitors because although it has similar antipyretic and analgesic properties, it exhibits little effect on inflammation.
According to Anderson (2008), the analgesic effect is produced at the central nervous system level without inhibiting peripheral prostaglandin secretion via cell membranes as do typical NSAIDs. Acetaminophen, being inactive as an anti-inflammatory agent in peripheral tissues, does not inhibit tooth movement (Arias & Marquez-Orozco, 2006).
Beyond the fact that it is not detrimental to orthodontic tooth movement, acetaminophen is a readily available, over-the-counter, inexpensive analgesic that has been found to be equally effective as ibuprofen and a placebo in controlling discomfort after archwire placement (Salmassian, Oesterle, Shellhart & Newman, 2009). Therefore, acetaminophen might be the drug of choice in treating mild to moderate discomfort associated with orthodontic treatment.
NSAID use and the orthodontic practitioner
Clinicians are responsible for comprehensive evaluation of a patient’s medical history and for its use as an integral part of the patient’s diagnosis. This includes an understanding of how their medication, prescription or over-the-counter, will effect their treatment. Given the frequency of NSAID use in this country, clinicians in the dental field are likely to encounter patients that are using these drugs regularly.
Furthermore, the future of analgesics in the United States is likely to hold tremendous growth due to the aging population who are facing conditions such as arthritis, which requires treatment using NSAID medications to allow for their increasingly active lifestyles. Given that more orthodontic practices are focusing on treating patients of all ages, this issue of increased NSAIDs use is more prevalent than ever (Turpin, 2009).
Common analgesics prescribed
Prescription and over-the-counter (OTC) use of analgesics among adults in the United States is extremely high. Most of these drugs are non-steroidal anti-inflammatory drugs that have analgesic, antipyretic, and anti-inflammatory action. They are used in treating headaches, arthritis, sports injuries, menstrual cramps and other illnesses.
Aspirin, a drug considered to be in the NSAID category, but distinguished from them by its irreversible inhibition of COX enzymes (Grosser, 2011), is also often taken regularly by patients to inhibit blood clotting and to prevent heart attack and stroke. Acetaminophen is also segregated from the NSAIDs by its weak anti-inflammatory effect, although it has similar analgesic and antipyretic effects. Important to note is that cold and allergy medications often contain these analgesics as well.
In a survey of American adults, OTC analgesics were shown to be the most frequently used of all medications and are taken by 20 percent of the adult populations in a given week (OTC Medications, n.d.). The non-prescription analgesics acetaminophen, aspirin, and ibuprofen are the most frequently used drugs in the United States (Slone Survey, 2006).
In any given week, 23 percent of adults in the U.S. report use of acetaminophen products, 17 percent used ibuprofen, 17 percent used aspirin and 3.5 percent use naproxen (NSAIDs, n.d.).
Over-the-counter analgesics are also regularly used by children. Of all prescription and OTC drugs taken by children in the United States, ibuprofen and acetaminophen are the two most frequently used (OTC Medications, n.d.). NSAIDs are mainly used in children in treating inflammatory pain, including chronic conditions such as juvenile idiopathic arthritis, where it is used for both its anti-inflammatory and analgesic properties. NSAIDs are also used in children to treat mild to moderate acute pain where inflammation is the source. (Gazarian & Graudins, 2006).
Acetaminophen is the first drug of choice for analgesia and treatment of febrile illness in single dose therapy for children because its analgesic and antipyretic efficacy is equivalent to NSAIDs but with less adverse effects. The combination of ibuprofen and acetaminophen or any alternating regimen of these two in treating fever in children is not recommended as it may potentiate the risk of toxicity of either drug (Gazarian & Graudins, 2006).
Adverse side effects of commonly used analgesics
In spite of the therapeutic efficacy and widespread usage of aspirin and NSAIDs, there are unwanted and serious side effects that have been recognized. It is doubtful that if these drugs were developed in this century that they would have been regulatory approved due to many and serious adverse effects (Jones, 2008).
The most common side effects that occur with aspirin and NSAID use are gastrointestinal(GI) (Grosser & Smyth, 2011), but other organ systems are also effected (Jones, 2008). GI symptoms occur in approximately 60 percent of users of these drugs (Jones, 2008). They are potentially serious and include anorexia, nausea, dyspepsia, abdominal pain, and diarrhea. These effects may be due to the creation of gastric or intestinal ulcers that occur in 15-30 percent of regular users of aspirin and NSAIDs (Grosser & Smyth, 2011).
Blood loss from ulcerations may be slow leading to anemia or become acute and life threatening. Risk is increased by consumption of alcohol, use of glucocorticoids, heliobacter pylori infection, and other factors that injure the mucosa (Grosser & Smyth, 2011). The vast majority of deaths due to NSAID and aspirin use are due to gastrointestinal bleeding (NSAIDs, n.d.).
GI effects of aspirin and NSAIDs occur at their recommended doses and the risk is dose related. In a study of users of aspirin and NSAIDs at OTC doses by Blot & McLaughlen, it was found that there was a two-fold risk of GI complications at lower than the maximum recommended OTC dosage, a four-fold increase at doses near the maximum, and a six-fold or greater increase at doses higher than the recommended daily OTC dose (NSAIDs, n.d.). Studies have shown that combining NSAIDs with low dose aspirin synergistically increase the risk of GI bleeding (Grosser & Smyth, 2011).
NSAID use also can have serious cardiovascular effects. According to studies made by regulatory agencies in the United States, Europe and Australia, “all NSAIDs have the potential to increase the risk of heart attack and stroke” (Grosser & Smyth, 2011). Patients that are at high risk of cardiovascular disease are most likely to be subject to adverse events when they are taking NSAIDs (Grosser & Smyth, 2011). Low dose use of aspirin has been prescribed for its cardioprotective effect, but at high doses can lead to congestive heart failure and pulmonary edema (Grosser & Smyth, 2011).
Studies have shown that NSAID use produces an increase in mean blood pressure of approximately 5 mmHg. This is significant, considering that a 5-6 mmHg increase in diastolic blood pressure lasting for a few years is associated with a 67 percent increased stroke risk and increase in coronary heart disease by 15 percent (Johnson, 1997). The hypertensive effect is related to the inhibition of COX-2 in the kidneys and vasculature, which decreases sodium excretion and increases peripheral vasculature volume (Grosser & Smyth, 2011).
Large studies of women in 2002 and men in 2007 at Harvard Medical School both show association between ibuprofen, acetaminophen and aspirin with hypertension. Compared with those who took no analgesics, men who took NSAIDs six to seven times per week showed a 38 percent greater chance of developing high blood pressure, as compared to those who took acetaminophen with a 34 percent greater risk, and to aspirin users who showed a 26 percent greater risk (Forman, Rimm & Curhan, 2007).
NSAIDs and aspirin have also been associated with adverse effects in other organ systems. Renal and renovascular side effects can occur, especially in patients that have heart, liver, or kidney disease (Grosser & Smyth, 2011). Hypersensitivity to aspirin and NSAIDs are also seen in some individuals. NSAID and aspirin use are contraindicated late in pregnancy due to increased chance of post partum hemorrhage and potential fetal risk (Grosser & Smyth, 2011).
Aspirin has other adverse effects that contribute to its potential misuse and toxicity. At anti-inflammatory doses, aspirin and other salicylates stimulate respiration by increasing oxygen consumption and production of carbon dioxide, and also by direct stimulation of the respiratory center in the medulla. Salicylates, at high doses, can cause injury to the liver. Use is contraindicated in patients under the age of 20 with viral illness associated fever due to its correlation with a severe hepatic injury and encephalopathy seen in Reye’s syndrome. Aspirin ingestion prolongs bleeding time through irreversible inhibition of platelet function.
A 325-mg dose of aspirin can double a person’s bleeding time for four to seven days. This calls for usage to be stopped at least one week prior to surgery and for caution or avoidance in patients with hepatic damage, hypoprothrombinemia, vitamin K deficiency, hemophilia, or undergoing long-term treatment with oral anti-coagulants. Long-term use also increases thyroidal uptake and iodine clearance, and at high doses hearing impairment and tinnitus commonly occur (Grosser & Smyth, 2011).
Acetaminophen, which is used for its analgesic and antipyretic effects, is a drug that is generally well tolerated at therapeutic doses, showing low incidence of GI side effects, and no cardiovascular or respiratory side effects. Acute overdose of acetaminophen however, can cause liver damage (Grosser & Smyth, 2011). With acetaminophen being the most commonly used OTC medication in the United States, it is important that patients are informed about guidelines for its usage.
Overdose of acetaminophen is the most common cause of acute liver failure (Wolf, et.al., 2012). Poor product labeling has been identified as a factor that has contributed to overdose of acetaminophen. A study published in the Journal of General Internal Medicine by Wolf, et. al. (2012) that surveyed 500 adult patients taking acetaminophen showed that 23.8 percent of participants would take more than the recommended maximum daily 4 gram dose of acetaminophen per day, and 5.2 percent would have taken a dangerously high dose of more than 6 grams per day. In another part of this study, 45.6 percent of patients would have exceeded maximum recommended doses by taking two products that contain acetaminophen.
Consumers do not adhere closely to labeled instructions and also do not recognize active ingredients in OTC pain medications (Wolf, et.al., 2012). Due to these studies, in July of 2011 Johnson & Johnson McNeil division lowered the maximum dose for Tylenol from 4000 mg (8 extra strength Tylenol pills) to 3000 mg (6 extra strength Tylenol pills) to reduce the risk of accidental acetaminophen overdose and possible liver failure and death (Mitchell, 2011). With acetaminophen included in over 600 OTC medications, as well as certain prescription analgesics, people can unknowingly ingest too much acetaminophen. Patients with liver disease or who drink alcohol heavily should avoid acetaminophen to decrease risk liver disease (Wolf, et.al., 2012).
In children it is uncommon to have serious toxicity associated with NSAID use, however similar effects that occur in adults can occur in children but with some variation. Although serious GI effects are uncommon in children, NSAIDs should be given with food to reduce mild gastrointestinal symptoms that can occur. Hepatitis is another side effect that can occur in children during NSAID treatment, but is most common with aspirin. Therefore, liver function in children should be monitored in those receiving long term NSAID treatment.
Incidence of renal toxicity in pediatric patients is low, with 0.2-0.4% prevalence in children with juvenile idiopathic arthritis (Gazarian & Graudins, 2006). CNS effects, including headache, skin reactions, and bronchospasm can also occur in children using NSAIDs. Long term NSAID use in children can also prolong bleeding time through inhibition of platelet aggregation (Gazarian & Graudins, 2006).
Discussion
Knowledge of the effects of NSAIDs on orthodontic tooth movement must encourage dental professionals to take a step back and focus on the foundation of patient care, starting with the medical history. Consideration of medications taken by patients that can interfere with tooth movement is important in order to reduce negative effects of prolonging orthodontic treatment.
Many studies on NSAIDs such as those by Knop, Shintcovsk, Retamoso, Ribeiro, and Tanaka, as well as Arias and Marquez-Orozco, have been conclusive in showing that NSAIDs slow down tooth movement by blocking the inflammatory response through inhibition of prostaglandins. In spite of the fact that these studies are scientific and well designed, there is some uncertainty when extrapolating data and applying it to humans in a clinical scenario. Weaknesses include animal subjects, variability in experimental design, drug administration techniques, and force characteristics (Bartzela, Turp, Motschall & Maltha, 2009).
The future of this research should include a design for further studies analyzing the effects of NSAIDs in humans during orthodontic treatment. With the information provided today, acetaminophen appears to be the analgesic of choice for orthodontic patients because it has been shown to have no effect on tooth movement, while being equally as effective as other NSAIDs in controlling orthodontic discomfort.
Summary
The practice of orthodontics is based on tooth movement through bone in response to application of mechanical forces. The bone remodeling that takes place occurs through an inflammatory process that is mediated by prostaglandins. Many orthodontic patients use OTC analgesics such as NSAIDs to control the discomfort associated with the inflammatory process, unaware that studies have shown these NSAIDs inhibit orthodontic tooth movement. Chemicals in the drug can pass through the bloodstream, reach the mechanically stressed tissues, and interact with local cells. In doing so, NSAIDs inhibit prostaglandin synthesis, therefore inhibiting the rate of orthodontic tooth movement as well.
It is suggested that practitioners be aware of all medications taken by patients that could interfere with tooth movement in order to reduce the negative effects of prolonging orthodontic treatment. Research has shown that traditional NSAIDs such as ibuprofen and aspirin decreased the rate of orthodontic tooth movement. Acetaminophen, an inactive inflammatory agent, had no effect. Acetaminophen should therefore be considered the analgesic drug of choice for patients undergoing orthodontics, unless contraindicated by the patient’s medical history or physician.
Note: This article will be published in a future issue of Ortho Tribune U.S. Edition. A complete list of references is available from the publisher.
Moving teeth with braces has long been considered a permanent cure to crowded teeth. However, we now know this traditional approach is neither permanent nor...
NEWARK, N.J., US: Acute and postoperative dental pain are inevitable, and pain management strategies often include the use of opioids; however, many studies...
Still in the early stages of the new millennium, we are in an era of dentistry and orthodontics where more accurate diagnoses are possible thanks to ...
With his high-definition photography of complex root canal systems, Dr. Craig Barrington, who practices dentistry in Waxahachie, Texas, is developing quite ...
A hallmark of the most successful modern clinicians is the ability to strike a balance between a daily load of 12 to 16 patients and maintaining the same ...
CORVALLIS, Ore., USA: A few years from now, millions of people around the world might be walking around with an unusual kind of glass in their mouth, and ...
Brea, Calif. — A global leader in orthodontic products, solutions and education for more than 60 years, Ormco Corp.is proud to announce The Ormco Forum ...
Over a thousand dental implant specialists who arrived in the Bahamas for the Fourth MIS Global Conference experienced the treat of their lives, well even ...
NEWPORT BEACH, Calif., USA: New research conducted on behalf of the Oral Cancer Foundation has found that many Americans are unaware of the fact that the ...
In 2002, 300 full-time faculty positions were unfilled, and an additional 200 to 600 new faculty members would be needed every year thereafter (Trotman, ...
Live webinar
Wed. 3 June 2026
1:00 PM EST (New York)
Live webinar
Thu. 4 June 2026
2:00 PM EST (New York)
Live webinar
Mon. 8 June 2026
12:00 PM EST (New York)
Live webinar
Mon. 8 June 2026
1:00 PM EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 PM EST (New York)
Live webinar
Wed. 10 June 2026
11:00 AM EST (New York)
Live webinar
Wed. 10 June 2026
2:00 PM EST (New York)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East



















































To post a reply please login or register