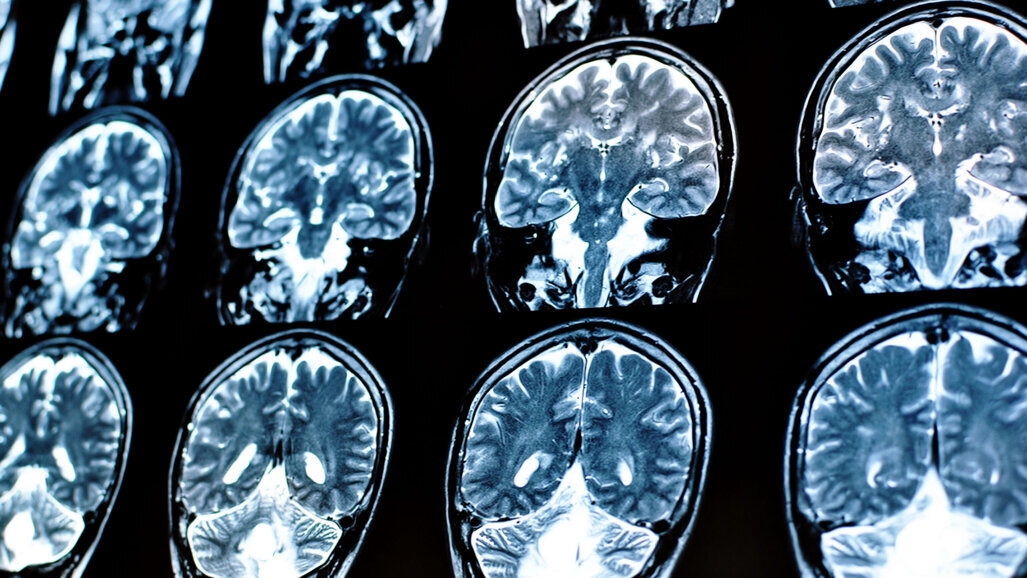
DALLAS, US: An increased burden of cerebrovascular disease could be connected to a genetic predisposition for poor oral health, according to a new study funded by the American Heart Association. The researchers used the presence of white matter hyperintensities, which are accumulated damage to the white matter of the brain, as evidence of cerebrovascular disease. Documented through magnetic resonance imaging (MRI), the resulting scans showed that for individuals who were genetically prone to edentulism or caries there was a 24% increase in white matter hyperintensities in their brains.
The white matter hyperintensities are linked to potential issues with balance, mobility and memory. The researchers also generated microstructural damage scores for the participants. Microstructural damage is the degree to which the fine architecture of the brain has changed in comparison with images for a normal brain scan of a healthy adult of similar age.
Using data from the UK Biobank, the samples included individuals primarily from the UK of European ancestry. They were evaluated for 105 possible genetic variations linked to caries, the eventual need for dentures or any form of edentulism. The researchers also noted that, when a participant had broader poor oral health beyond caries and edentulism as a result of genetics, the microstructural damage score increased to 43%.
Lead author Dr Cyprien Rivier, a postdoctoral research fellow in the Department of Neurology at the Yale School of Medicine in New Haven in Connecticut, commented in a press release: “Studying oral health is especially important because poor oral health happens frequently and is an easily modifiable risk factor—everyone can effectively improve their oral health with minimal time and financial investment.” Dr Rivier also noted the value of using neuroimaging tools such as MRI to assess the impact of oral health upon brain function.
Dr Joseph P. Broderick, a professor at the University of Cincinnati Department of Neurology and Rehabilitation Medicine and a Stroke Council member, said that the findings should spur more research but are not concrete evidence that improved oral hygiene will improve brain health. He noted that genetic factors for a variety of conditions could overlap with those that cause poor oral health. Dr Broderick said: “Environmental factors such as smoking and health conditions such as diabetes are much stronger risk factors for poor oral health than any genetic marker—except for rare genetic conditions associated with poor oral health, such as defective or missing enamel.”
The findings were presented at the American Stroke Association’s International Stroke Conference 2023, which took place from 8 to 10 February in Dallas in Texas.
Tags:
NEW YORK, NY, USA: NYU dental researchers have found the first long-term evidence that periodontal (gum) disease may increase the risk of cognitive ...
COLUMBIA, S.C., US: Growing evidence continues to demonstrate the far-reaching impact of oral health on systemic well-being. Just recently, two new studies ...
STONY BROOK, N.Y., US: The applicability and efficacy of artificial intelligence (AI) within dentistry appears to be limitless. With each passing day, ...
NEW YORK, N.Y., USA: A Danish–American study has proven that incidences of Alzheimer's disease can be traced back to chronic gum inflammation. ...
CHICAGO, IL / NEW YORK, NY, USA: The Academy of General Dentistry (AGD) and the AGD Foundation recently teamed up with the Louisiana State University (LSU) ...
BOSTON, US: Adding to existing evidence on the link between vaping and a deterioration in oral health, researchers from Tufts University School of Dental ...
WASHINGTON, US: While the links between oral and systemic health are well established and widely discussed in the dental literature, the broader ...
NEW YORK, US: At the 80th session of the UN General Assembly, member states adopted a landmark political declaration on non-communicable diseases (NCDs) and...
The minimally invasive (MI) concept was initially introduced in physical medicine and adopted into dental medicine in the early 1970s with the application ...
NEW YORK, N.Y., USA: Colgate-Palmolive has announced the launch of the Colgate Oral Health Network for Professional Education and Development — a new ...
Live webinar
Wed. 3 June 2026
1:00 PM EST (New York)
Live webinar
Thu. 4 June 2026
2:00 PM EST (New York)
Live webinar
Mon. 8 June 2026
12:00 PM EST (New York)
Live webinar
Mon. 8 June 2026
1:00 PM EST (New York)
Dr. Anthony Mak B.D.S, Prof. Marleen Peumans
Live webinar
Mon. 8 June 2026
2:00 PM EST (New York)
Live webinar
Wed. 10 June 2026
11:00 AM EST (New York)
Live webinar
Wed. 10 June 2026
2:00 PM EST (New York)
Nacho Fernández-Baca DDS, MSc



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East



















































To post a reply please login or register