Osseous grafting needs to be performed in some clinical situations. This may vary from socket preservation following extraction, repair of bone loss at the furcation, filling voids between the socket walls and implant when immediate implants are planned, sinus augmentation to treatment of exposed implant threads. These are managed by use of osseous particles, which can be allografts, autografts, xenografts or even synthetic materials.
Clinically, osseous particles have a potential for dispersement during the initial healing period. Although they may be rehydrated or wetted with various liquids, such as saline, water or anesthetic, these liquids do not hold the particles together, allowing them to spread in the area during initial healing. This results in less volume of the healed graft at the site and may compromise the intended results.
Utilization of patient-derived autogenous blood concentrates (ABC) mixed with the particulate graft material improves graft handling during placement as well as maintaining the graft at the intended site, eliminating dispersion potential. Autologous blood concentrates are defined as the concentrated portion of the patient’s blood following centrifuging. The resulting product contains growth factors, platelets, WBC and fibrin, but does not contain the RBC portion of the blood.
Benefits of using ABC with osseous graft materials
Several reports in the 1980s identified the pivotal role oxygen plays in wound healing.1-5 These studies were the first to recognize that growth factors promote healing related to the macrophage response to oxygen gradients, which secreted those wound-healing growth factors. Platelet-derived wound healing factor (PDWHF) was first introduced clinically6 and continued on to Platelet-Rich Plasma (PRP) utilized for more than two decades to initiate wound healing.
Thrombin-released platelets produce angiogenesis and collagen synthesis with fibrin eliciting a cellular exudate, followed by angiogenesis. Marx and Garg in the early 1990s began work on patient-derived blood as a fibrin source for use with osseous grafts to improve product handling. They first published in 1994 on this fibrin adhesive. 7
Growth factors are secreted by platelets (PDGFaa, PDGFbb and PDGFab) stimulating mesenchymal stem cells to replicate, osteoblasts to replicate and produce osteoid, endothelial cells to replicate secreting basal lamina for new blood vessels and fibroblasts to replicate producing collagen.
Additionally, bone morphogenic protein (BMP) and transforming growth factors (TGFß1 and TGFß2) are present to stimulate matrix production and guide cell differentiation into bone. Other factors present in the ABC include vascular endothelial growth factor (VEGF), which stimulates development of new blood vessels, and epithelial growth factor (EGF), which stimulates migration of the surrounding soft tissue to cover the area and form a basement membrane.
Incorporation of ABCs, such as PRP into a particulate graft material, provides growth factors to accelerate healing of the graft, stimulating the host cells adjacent to the graft to convert into native bone. Additionally, more rapid closure of the soft tissue using the patients’ own factors as a stimulating mechanism can be expected.
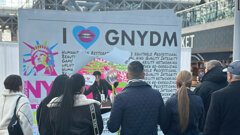
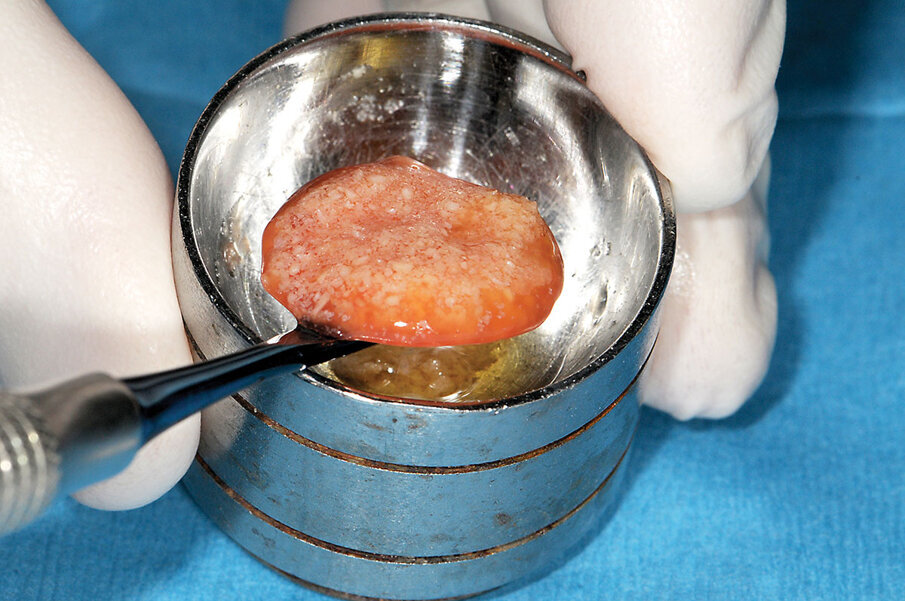
The additional benefit is a gelatinous mass, termed "gummy bone," that has improved handling without the dispersion issues found with particulate graft particles mixed with saline or even allowed to absorb blood at the site (Fig. 1). Gummy bone provides a flexible putty-like consistency that can be cut to desired dimensions prior to placement and utilized in a variety of clinical graft situations that include: socket grafting (Fig. 2), filling voids around immediate implant placement (Fig. 3), lateral sinus augmentation (Fig. 4), crestal sinus augmentation (Fig. 5), lateral ridge expansion (Fig. 6), dehiscence repair at implant placement (Fig. 7) and furcation repair (Fig. 8).
Fig. 2: Following extraction, ‘gummy bone’ is placed into the socket for preservation of the site.
Fig. 3: Voids between the implant being placed and the extraction socket walls are filled with ‘gummy bone’ prior to site closure.
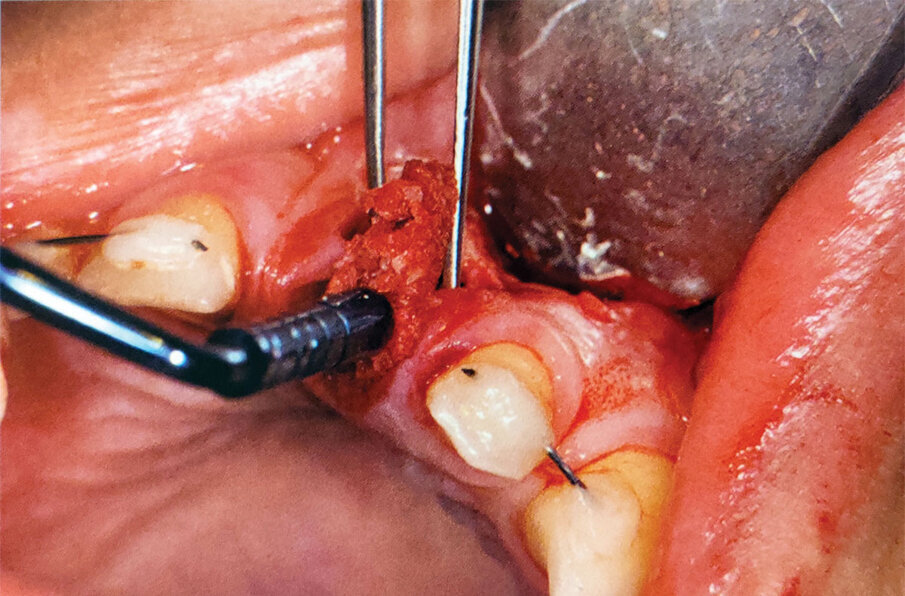
Fig. 4: ‘Gummy bone’ being placed into a lateral window sinus augmentation, allowing better placement against the medial, distal and mesial walls of the elevated sinus.
Fig. 5: ‘Gummy bone’ being introduced into the osteotomy where a crestal sinus elevation has been performed to increase the crestal height prior to implant insertion.
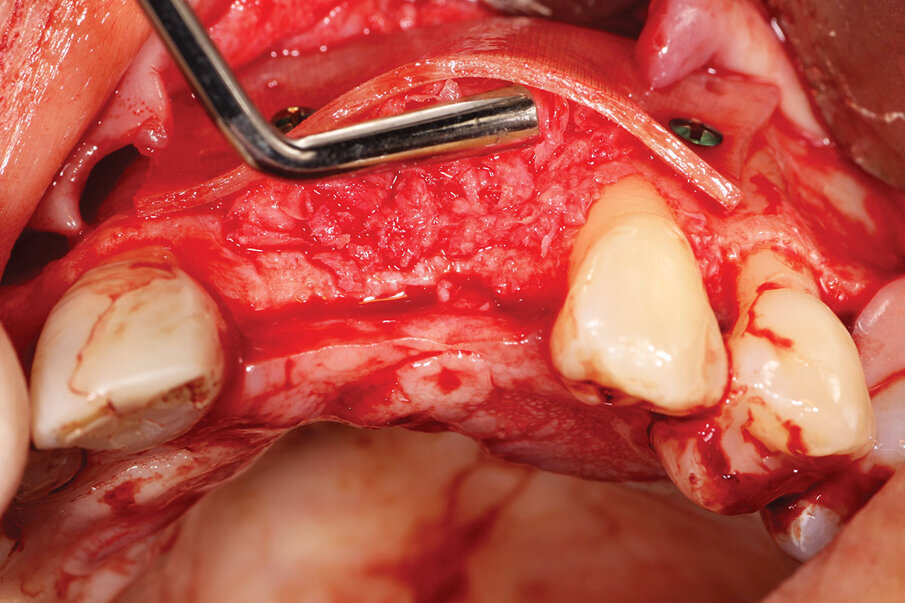
Fig. 6: ‘Gummy bone’ being placed between the facial aspect of the ridge, and the bone plate placed to widen the ridge to allow implant placement after healing.
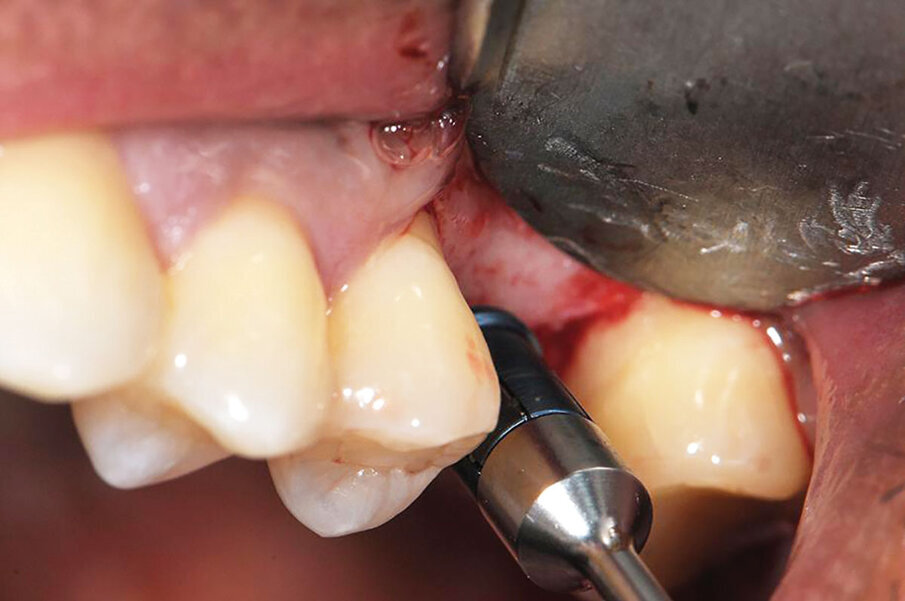
Fig. 7: Placement of ‘gummy bone’ over exposed implant threads at implant placement that will allow the osseous graft to remain where needed as the bone heals and prevent dispersement found when particulate graft is used alone.
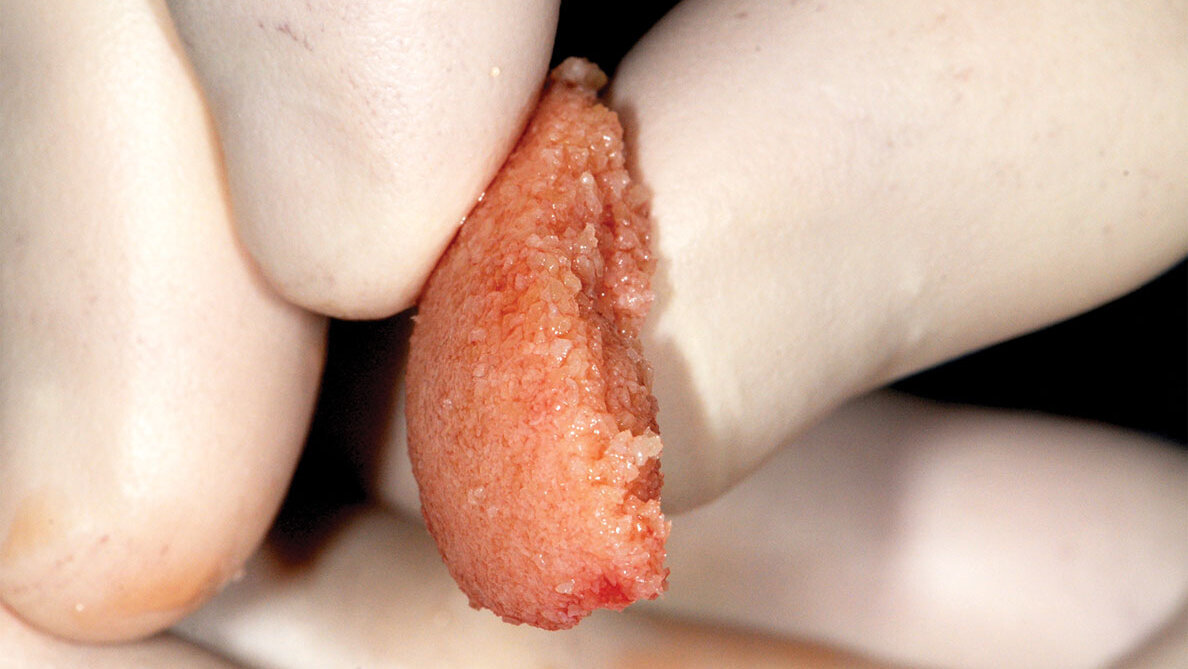
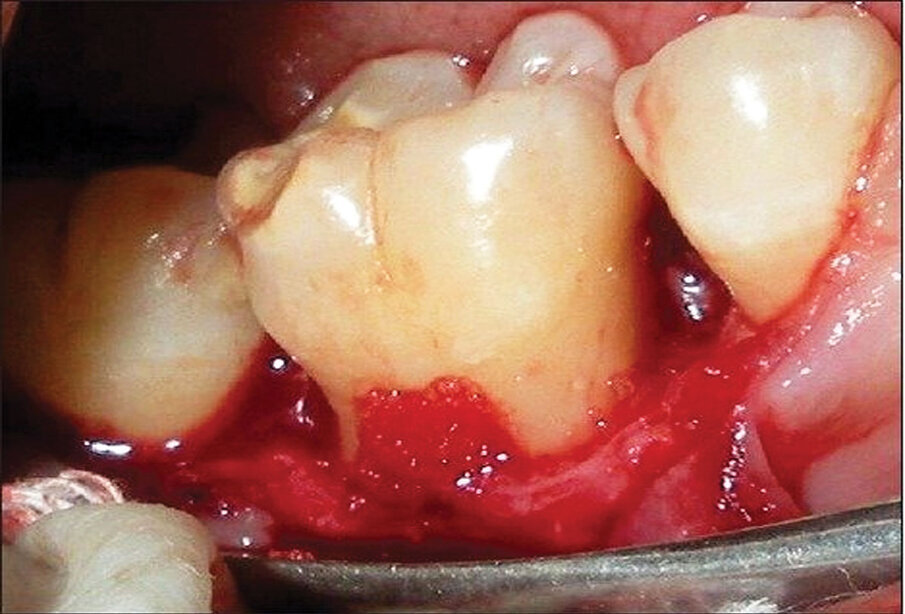
Fig. 8: Placement of ‘gummy bone’ into a furcation defect, allowing the graft to remain where placed and avoid dispersement potential typically observed with particulates rehydrated with saline.
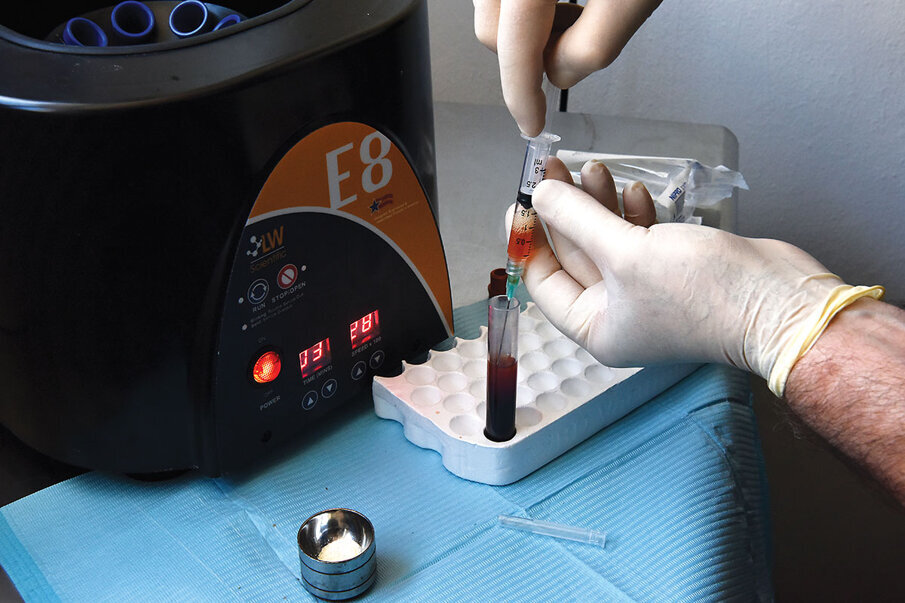
Fig. 9: Following phlebotomy, the patient’s blood is centrifuged at 2,200 rpm for three minutes.
Fig. 10: Following centrifugation, the blood separates into several layers as outlined in Fig. 9.
Fig. 11: Allograft (cortical, cancellous or a mixture of the two) is dispensed from the bottle into a sterile dish.
Fig. 12: The plasma (yellow liquid) is drawn out of the centrifuged tube with a syringe.
Fig. 13: The plasma is placed into the sterile dish containing the allograft particles.
Fig. 14: The plasma wets and rehydrates the allograft particles and is allowed to sit for 10 to 12 minutes before use.
Fig. 15: After 10 to 12 minutes, the fibrin within the plasma that had been mixed with the allograft particles forms a gelatinous mass referred to as ‘gummy bone.’
Fig. 16: The ‘gummy bone’ is used as a single mass when placing in large voids.
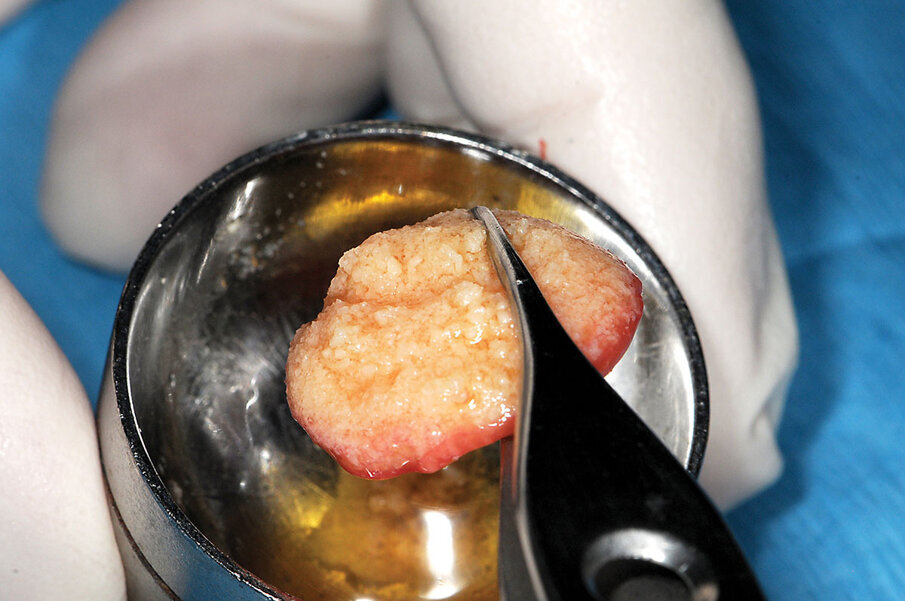
Fig. 17: The ‘gummy bone’ is cut with scissors into smaller pieces that can be incrementally placed into the surgical site.
Author Gregori M. Kurtzman, DDS
Author Maria del Pilar Rios, DMD, MSc, PhD
Author Renato Rossi Jr., DMD, MSc, PhD
‘Gummy bone’ fabrication
Blood is drawn from the patient at the initiation of surgical treatment into red top tubes. These red top tubes are glass walled and contain no anticoagulant. These are immediately centrifuged at 2,200 rpm for 3 minutes to create separation of the layers of the patient’s blood (Fig. 9). Upon completion of centrifuging, distinct layers are present in the tube (Fig. 10). For the purposes of creating "gummy bone", the yellow layer, which is the plasma (and is high in fibrin) and platelets will be used.
Osseous graft particles that will be used are dispensed into a sterile dish (Fig. 11). A syringe and needle is used to withdraw the plasma liquid from the tube (Fig. 12), and then it’s dispensed into the dish containing the osseous graft particles (Fig. 13). This hydrates the dry graft particles, which is allowed to sit for 10-12 minutes to coalesce into a gelatinous mass (Fig. 14).
Following the coalescence period, the "gummy bone" is formed and is ready for use (Fig. 15). This does not need to be immediately used during the surgery and can sit in the dish until graft placement in the treatment process is ready.
The gummy bone can be used as a single mass when placing in large voids (Fig. 16), such as a sinus augmentation, or cut with scissors into smaller pieces that can be incrementally placed into the surgical site (Fig. 17). These pieces of “gummy bone” will adhere to each other when they are placed into contact with each other or the surrounding tissues.
Conclusion
As discussed, one of the main challenges to osseous grafting is handling of the graft materials both during initial placement and during the initial healing period. Particle dispersement is not uncommon with particulate materials, as when wetted by non-hematological liquids, this can limit site blood from infusing into the graft placed initially, allowing dispersement to occur. Placing the dry particles into the site to be grafted and allowing blood from the surrounding tissues to wet it also limits holding the mass together. There may be limited bleeding from the bone surface and it might not penetrate throughout the graft.
Fibrin from the autogenous blood concentrate has more favorable characteristics, acting as "tissue glue" to hold the particulate graft into a pliable mass. This pliable material handles better, allowing easier shaping for the defect being treated, with potential to increase width when needed that can not be easily accomplished with particulate bone when autogenous blood concentrates are not added.
The added benefit of the platelets and associated growth factors stimulates angiogenesis, thus using the patients’ own systemic factors to aid in graft coalescence, organization and maturation. Those practitioners who are utilizing particulate graft materials in their treatment modalities should consider incorporating autogenous blood concentrates such as PRP to improve graft handling, eliminate particle dispersement during healing and stimulate regeneration via the growth factors that are now incorporated within the placed graft material.
Authors
Arun K. Garg, DMD; Gregori M. Kurtzman, DDS; Renato Rossi Jr., DMD, MSc, PhD; and Maria del Pilar Rios, DMD, MSc, PhD
References
- Knighton DR, Silver IA, Hunt TK.: Regulation of wound-healing angiogenesis-effect of oxygen gradients and inspired oxygen concentration. Surgery.1981 Aug;90(2):262-70.
- Knighton DR, Hunt TK, Scheuenstuhl H, Halliday BJ, Werb Z, Banda MJ.: Oxygen tension regulates the expression of angiogenesis factor by macrophages. Science.1983 Sep 23;221(4617):1283-5.
- Marx RE, Johnson RP.: Studies in the radiobiology of osteoradionecrosis and their clinical significance. Oral Surg Oral Med Oral Pathol.1987 Oct;64(4):379-90.
- Hunt TK.: The physiology of wound healing. Ann Emerg Med.1988 Dec;17(12):1265-73.
- Marx RE, Ehler WJ, Tayapongsak P, Pierce LW.: Relationship of oxygen dose to angiogenesis induction in irradiated tissue. Am J Surg.1990 Nov;160(5):519-24.
- Knighton DR, Hunt TK, Thakral KK, Goodson WH 3rd.: Role of platelets and fibrin in the healing sequence: an in vivo study of angiogenesis and collagen synthesis. Ann Surg.1982 Oct;196(4):379-88.
- Tayapongsak P, O'Brien DA, Monteiro CB, Arceo-Diaz LY.: Autologous fibrin adhesive in mandibular reconstruction with particulate cancellous bone and marrow. J Oral Maxillofac Surg.1994 Feb;52(2):161-5; discussion 166.
Tags:



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East























































To post a reply please login or register