Histologically, enamel scaffold proteins, such as amelogenin, are routinely secreted by ameloblasts and deposited within immature enamel during the secretion stage. As the maturation stage begins, these proteins are degraded by protease activity and spatially replaced by hydroxyapatites. In the case of fluorosis, an increased level of fluoride ions (instead of calcium ions) is detrimental to protease activity, leading to protein and water molecule retention within the enamel layers; as a result, the affected enamel is low in mineral content and is porous.4
Several treatment modalities have been suggested for treating fluorosis enamel discoloration, ranging from ultra conservative tooth bleaching to invasive complete crowning of the affected teeth.4 Resin infiltration, enamel macro- and micro-abrasion, and facial veneers are other options for correcting shade discrepancy.5 Choosing the appropriate treatment depends greatly on the size and depth of the lesion, the clinician’s experience and the patient’s choice. In mild cases, bleaching alone may provide satisfactory aesthetic results, as the discoloured spots will blend better with the surrounding healthy enamel.5 Alternatively, mild to moderate cases may be approached by bleaching treatment followed by resin infiltration, enamel macro-or micro-abrasion, resin or porcelain veneers, or a combination treatment. Nevertheless, deeper lesions are more challenging and often require more invasive procedures, such as complete crown coverage.4
Dental bleaching is routinely done in office or at home, both achieving similar long-term success.6 Resin infiltration is a technique that utilises a low-viscosity, polymerisable resin after the external enamel surface has been treated with 15% hydrochloric acid. A single application of 15% hydrochloric acid to enamel surfaces can dissolve and remove 37–58μm of superficial enamel, rendering the deeper fluorosis lesion more accessible by the infiltrate. This novel technique was initially introduced as a conservative approach to arresting incipient carious lesions.5 Over time, clinical evidence has emerged that suggests its ability to mask opacities associated with hypomineralised enamel lesions.7 In theory, treating white spot lesions with resin infiltration obliterates enamel pores with a material (i.e. resin) that has a refractive index closer to that of healthy enamel (RI = 1.62; resin RI = 1.42) than air (RI = 1.00) and water (RI = 1.33). In contrast to resin infiltration, micro-abrasion utilises an acidic slurry of hydrochloric acid and pumice that is actively brought into contact with affected enamel using a rubber cup rotating at a slow speed. A recent systematic review concluded that resin infiltration has the highest effectiveness in treating mild to moderate lesions, followed by bleaching and then micro-abrasion. Macroabrasion simply utilises a dental bur to eliminate the affected hypomineralised area, which is subsequently restored with a restorative material. This case study aimed to visually evaluate the effectiveness of home bleaching followed by resin infiltration in resolving the aesthetic concerns of a patient with fluorosis-affected central incisors.
Case presentation
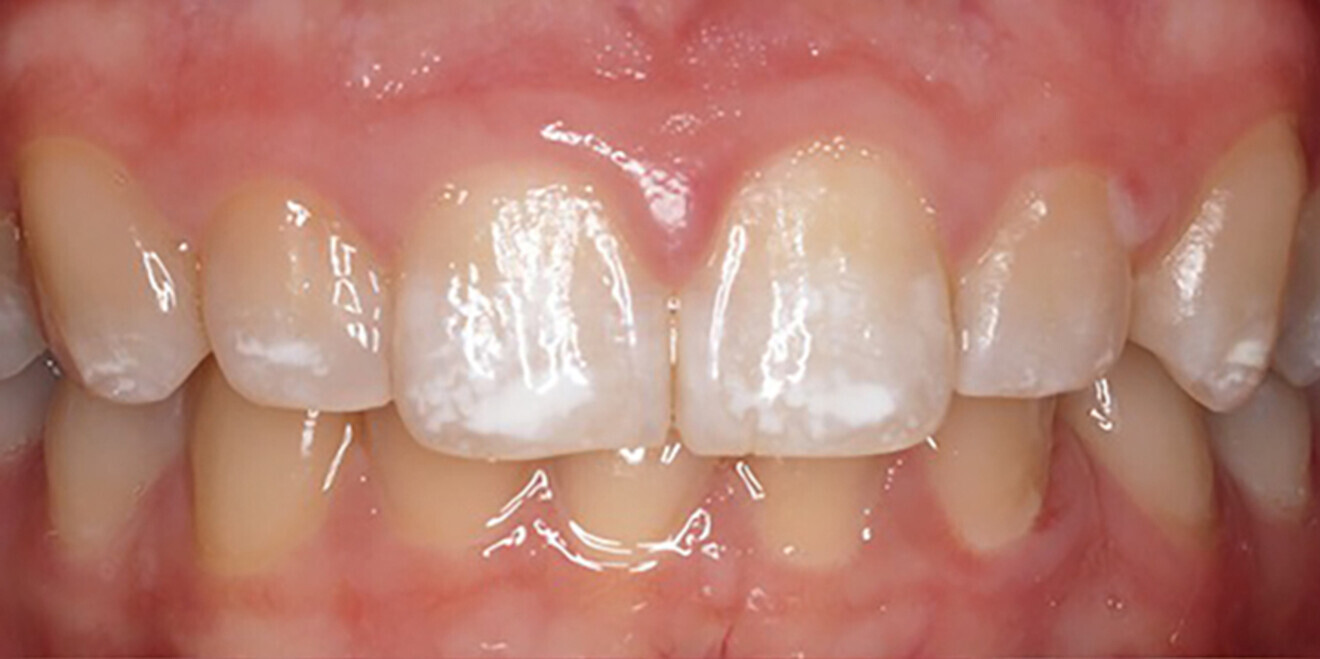
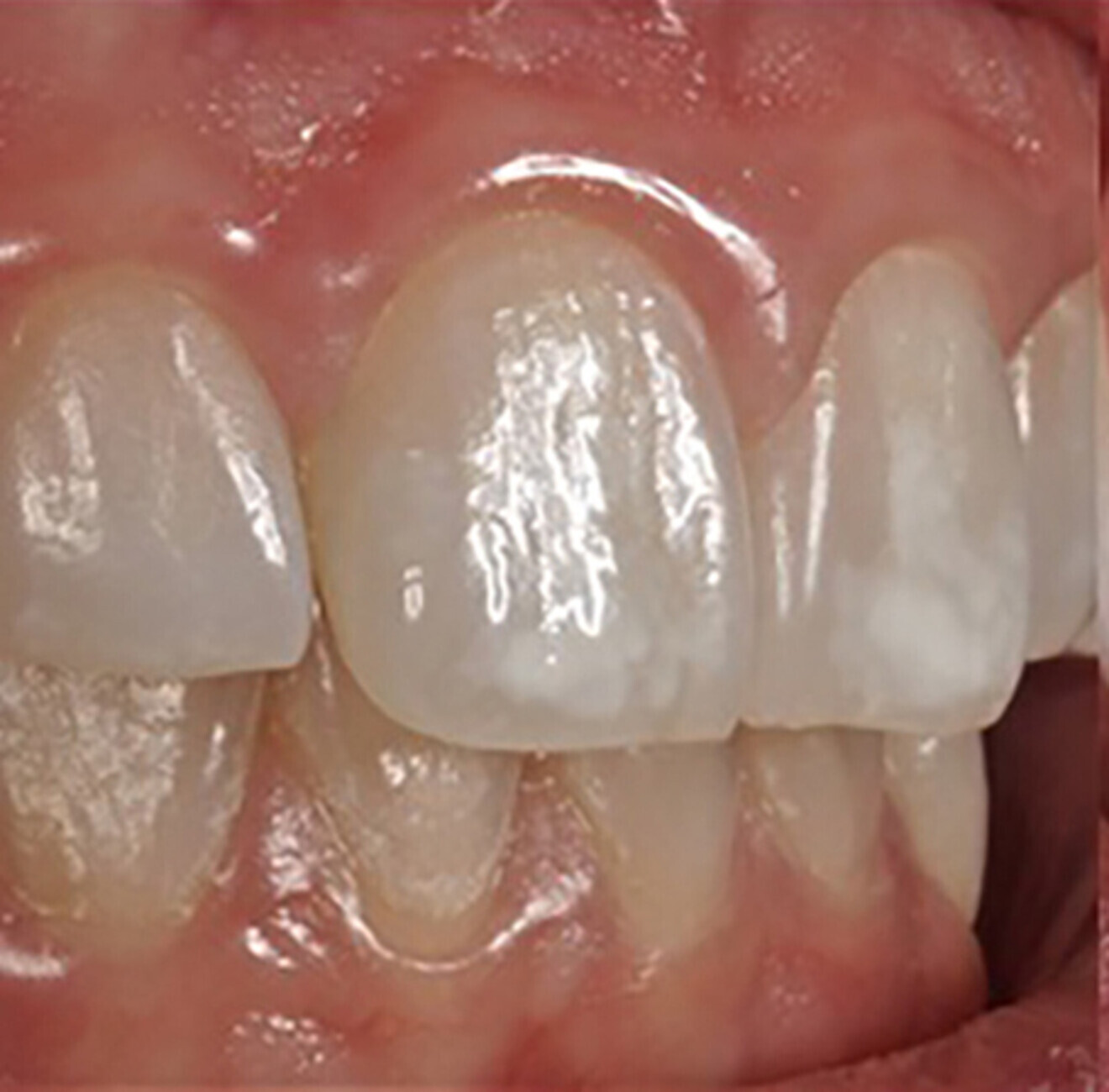
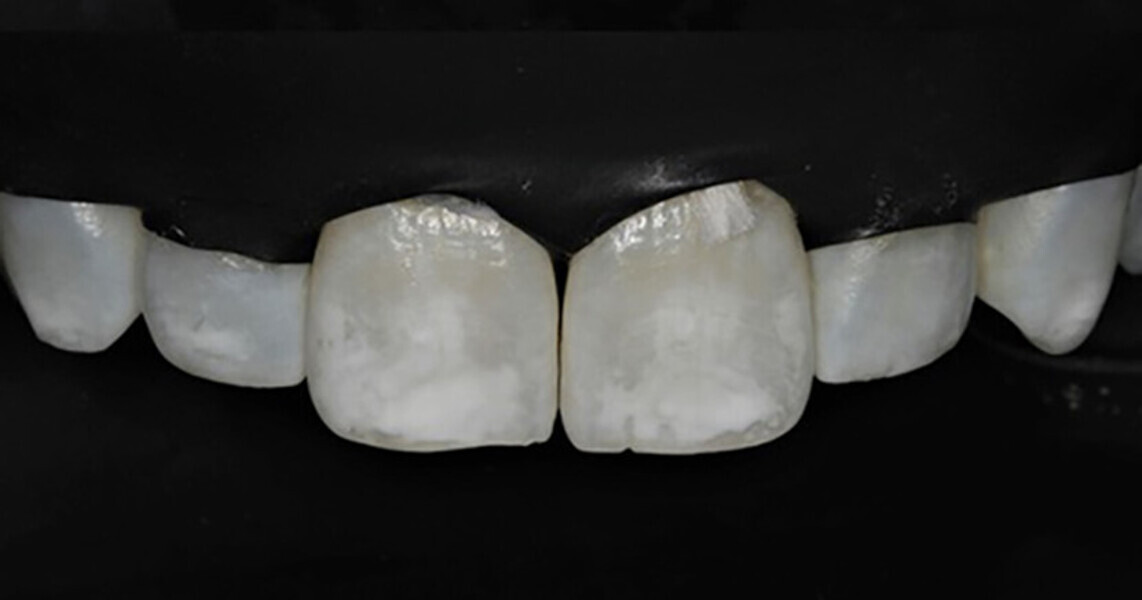
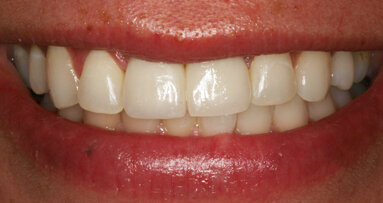
A 27-year-old female patient attended the Operative Dentistry Clinic at the University of Iowa College of Dentistry and Dental Clinics complaining of white spot enamel opacities on her maxillary anterior teeth, mainly the central incisors (Fig. 1a). There was no discomfort or history of sensitivity. Other family members had similar white spot complaints, according to the patient. Her local dentist suggested that her condition was most likely due to the high fluoride content of the drinking water. Periapical radiographs were within normal limits, and vitality testing (liquid carbon dioxide) revealed a normal response. Conservative treatment options to correct shade discrepancy included resin infiltration, enamel macro- and micro-abrasion, and/or porcelain veneers.
Tooth bleaching was suggested to reduce colour discrepancy and enhance the blending effect between the lesion body and the surrounding enamel. The patient opted for home bleaching using 10% carbamide peroxide with potassium nitrate and fluoride (Opalescence PF 10%, Ultradent). Custom-made trays and home instructions were also provided at the same visit. The patient was asked to discontinue bleaching two weeks prior to her upcoming infiltration treatment appointment. According to a review, a waiting period of one to three weeks is recommended prior to resin composite bonding to reverse the detrimental effect of any remaining oxygen on resin polymerisation and bonding.8
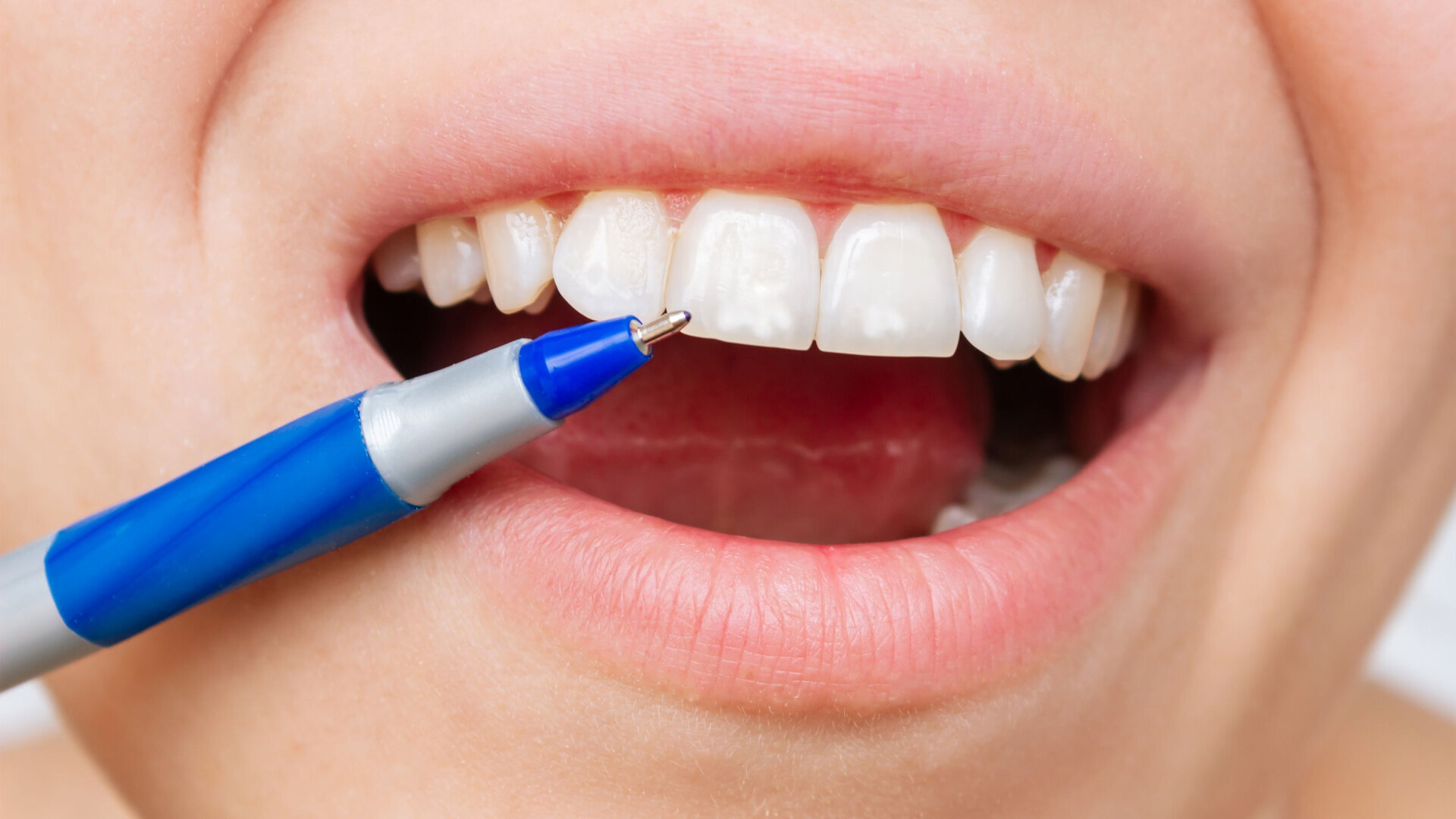
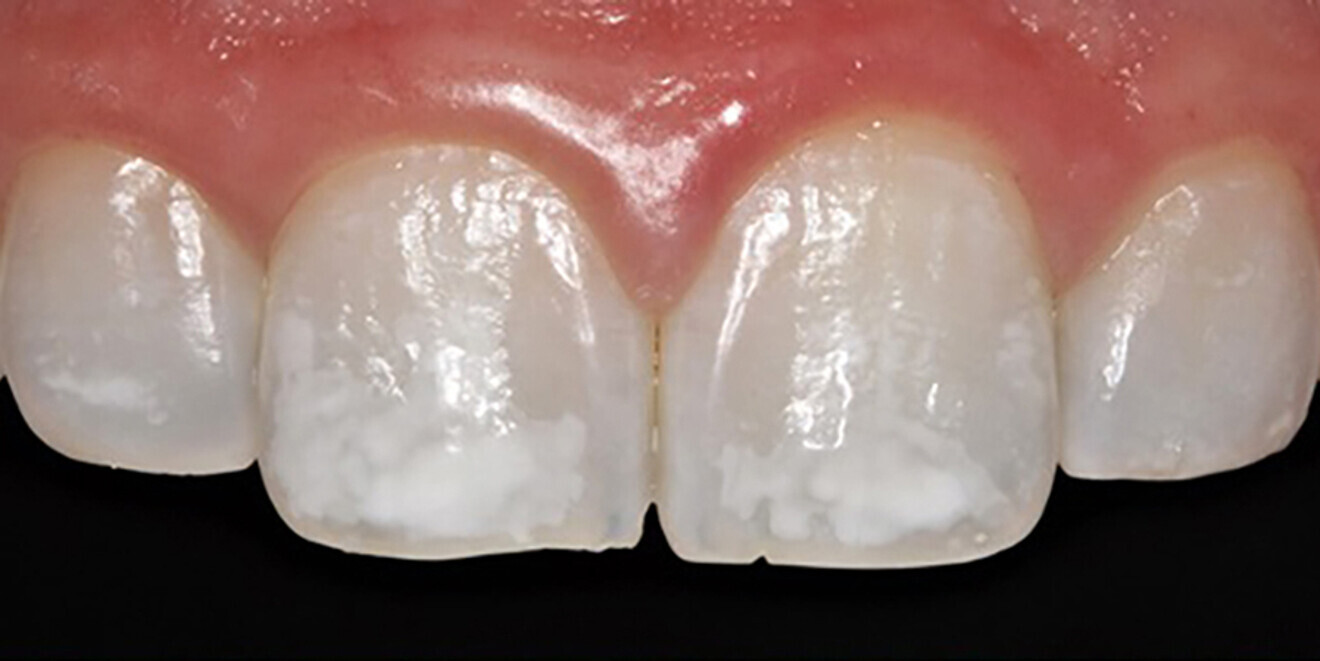
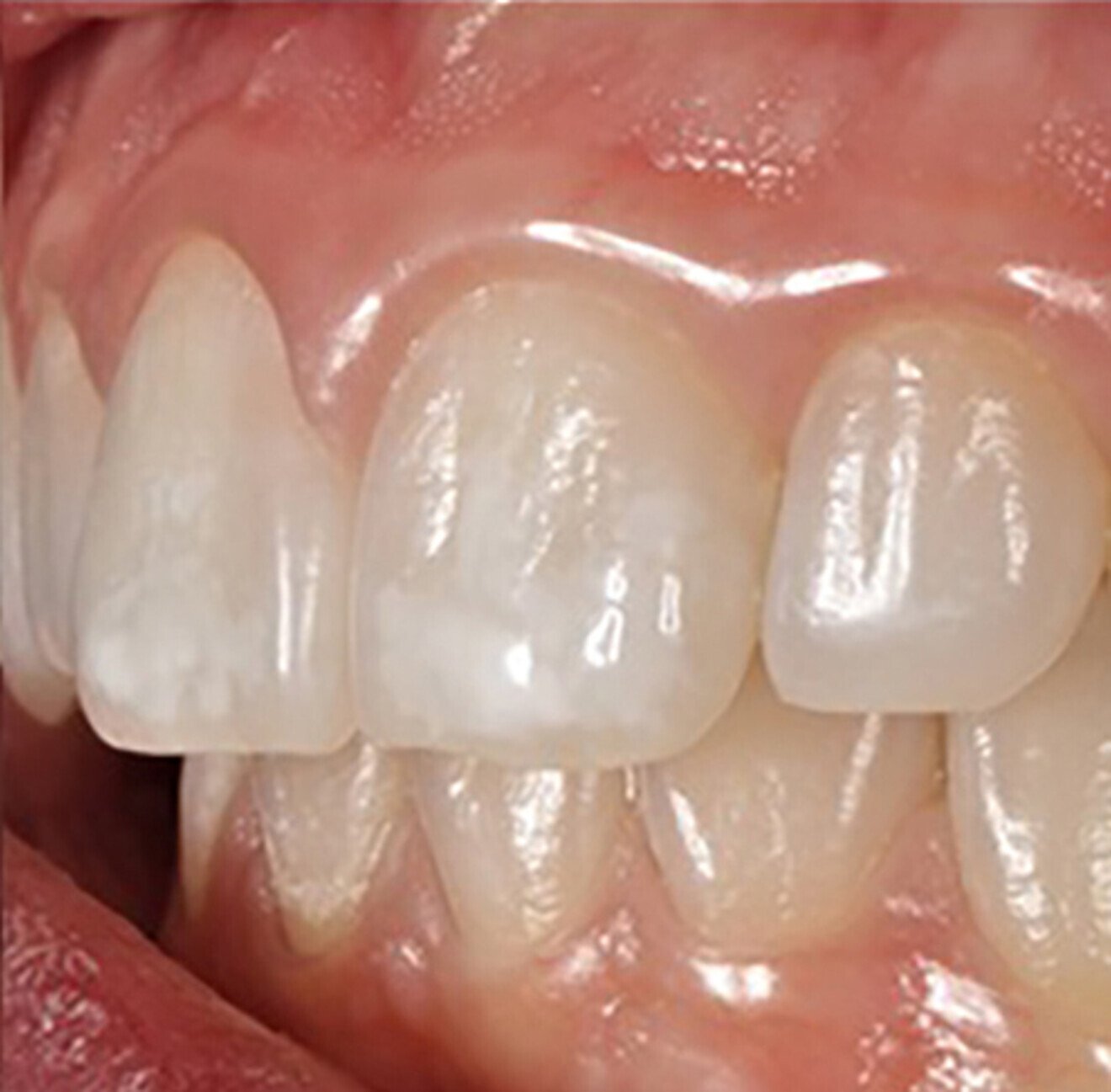
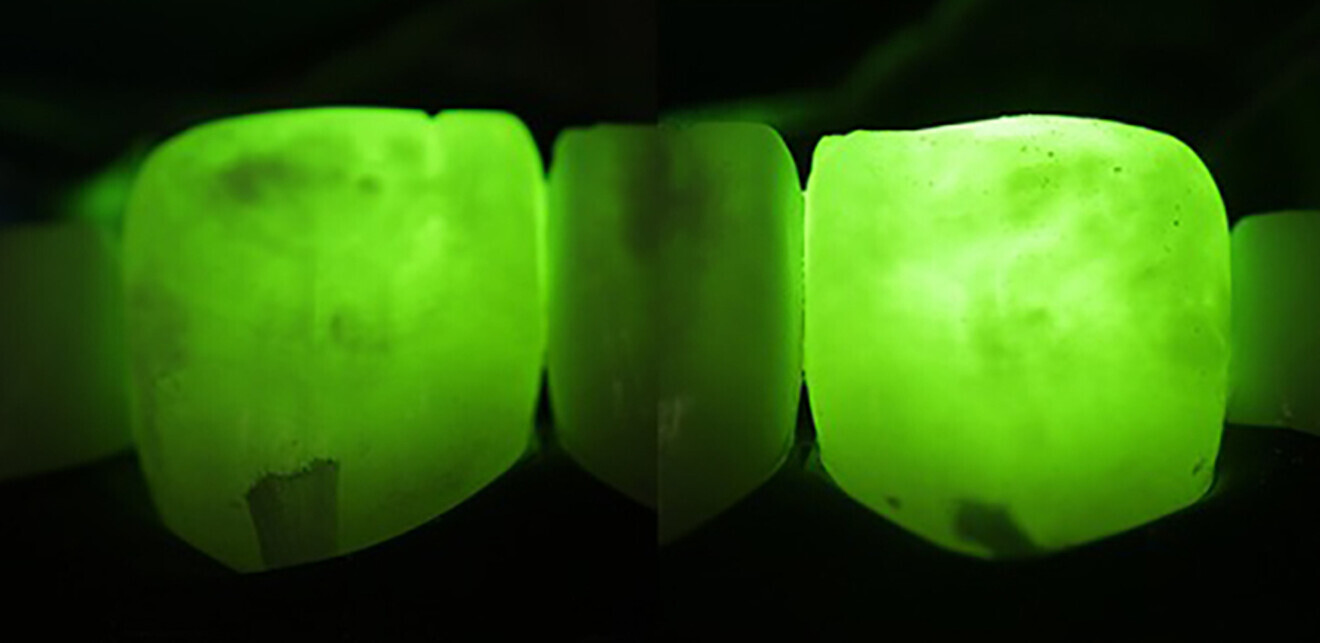
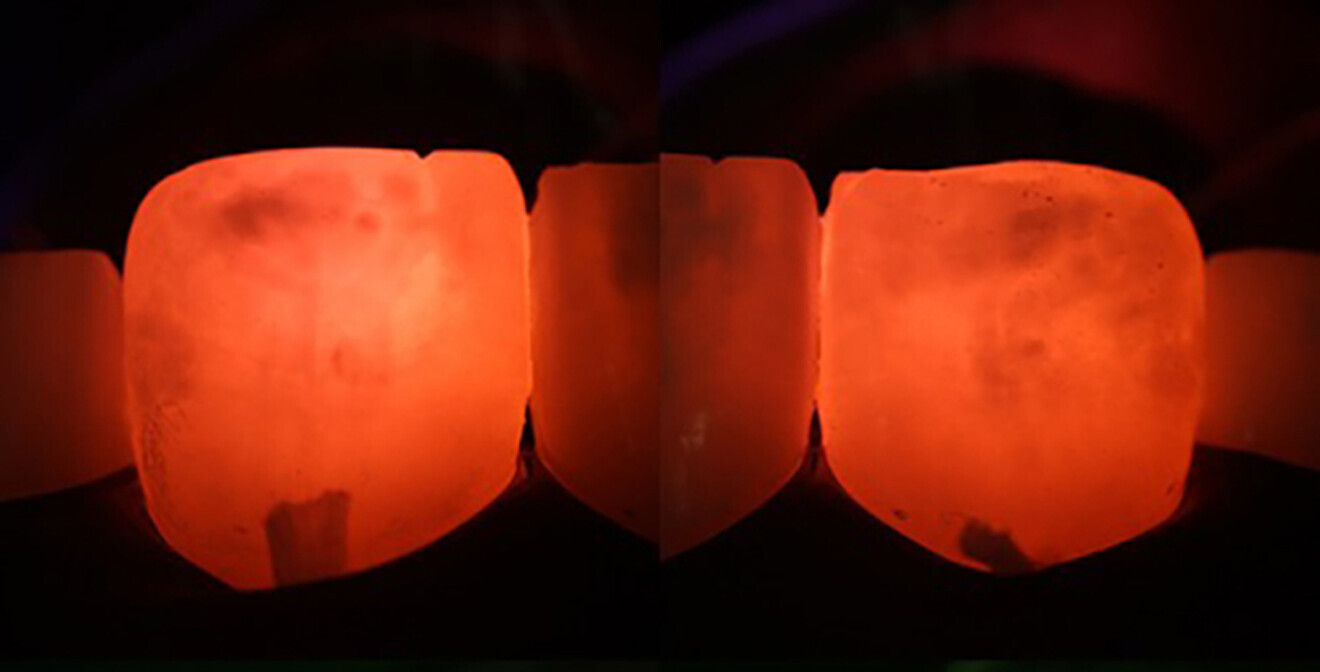
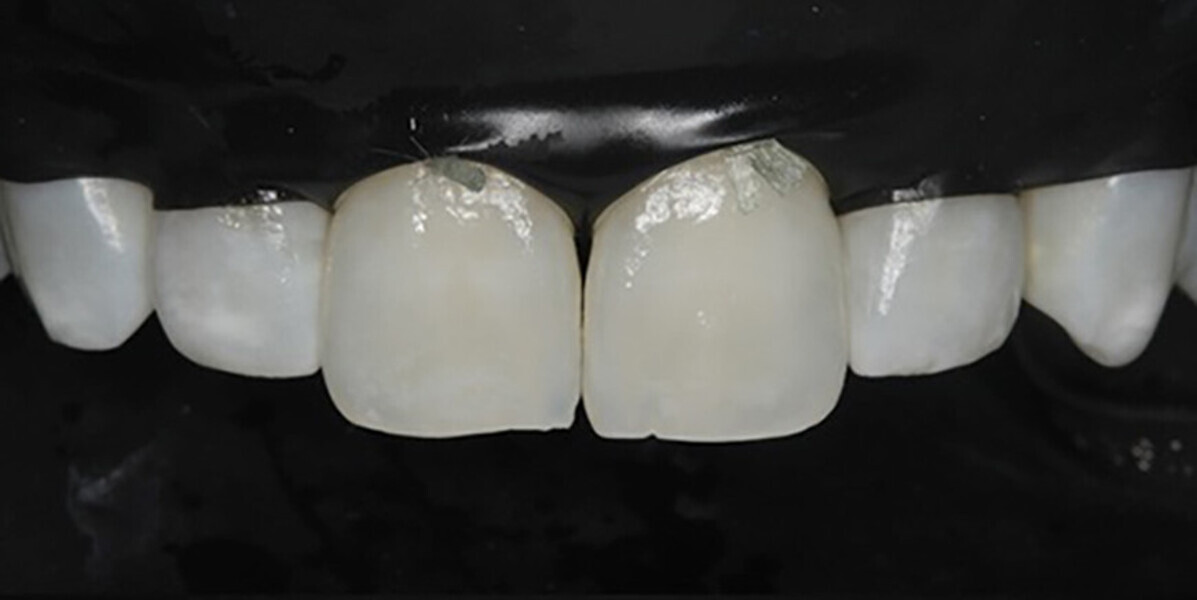
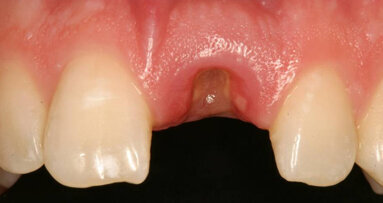
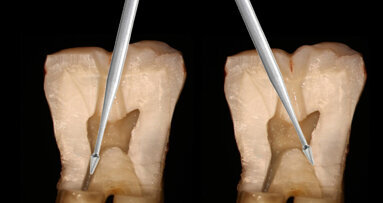
Six weeks after the initial appointment, the patient returned with visually whiter teeth, but the lesions were still noticeable (Figs. 1b & 2). To determine the most conservative and effective technique to address her aesthetic concerns, coloured filters were attached to a curing light tip, the light was projected from the lingual aspect and the colour changes on the facial surface were observed (Fig. 3). This procedure can assist the clinician in estimating the depth of the lesion; the deeper the lesion, the greater the light blockage. For deeper lesions, a combination of various treatment means may be more appropriate. In this patient’s case, the right central incisor lesion was less extensive than the left central incisor lesion, and thus, a better outcome was anticipated. Resin infiltration was selected to treat both lesions.
A dental dam with tight floss ligation was placed (Fig. 4a) to assist in isolation, prevent saliva contamination and protect the soft tissue from the hydrochloric acid. Both central incisors were polished with a non-fluoride polishing paste and a rubber cup. The resin infiltration treatment was performed according to the manufacturer’s instructions. Icon-Etch (15% hydrochloric acid; DMG) was applied passively to the affected areas and periodically massaged for 2 minutes. The surfaces were then wiped with a cotton pellet to remove the acid gel, and the residue was rinsed off with copious water irrigation for 30 seconds. The surfaces were then thoroughly dried with a continuous stream of oil-free and water-free air.
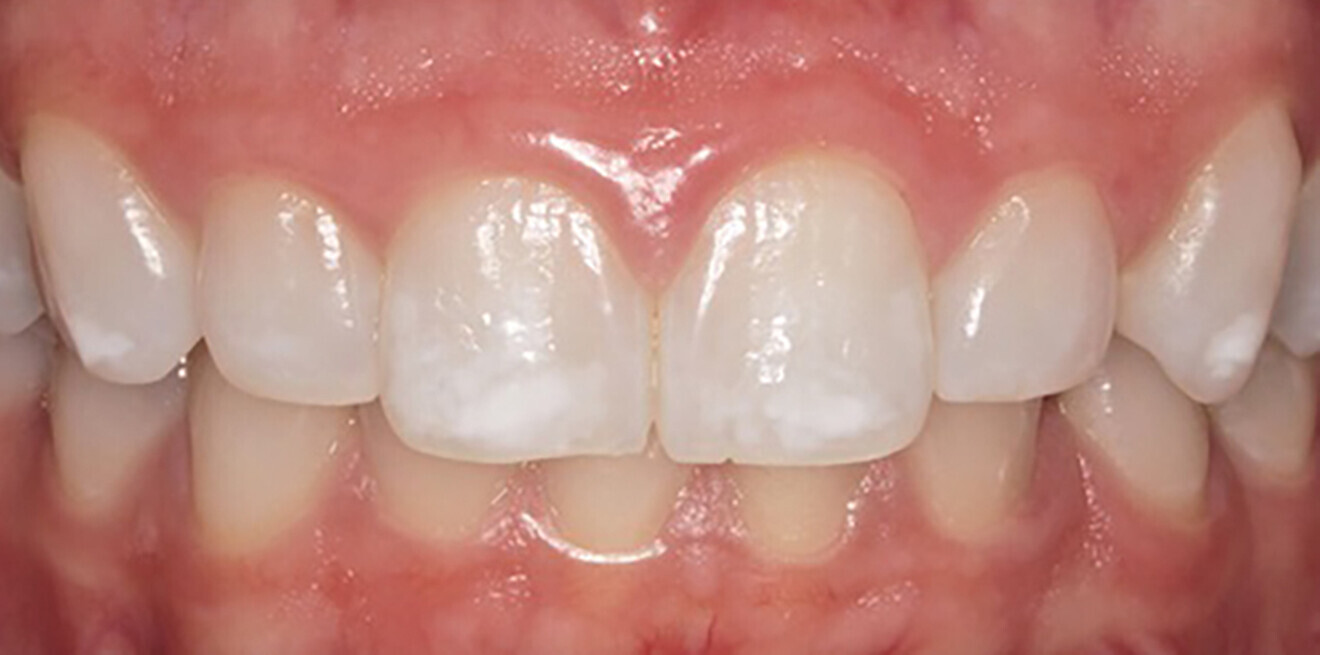
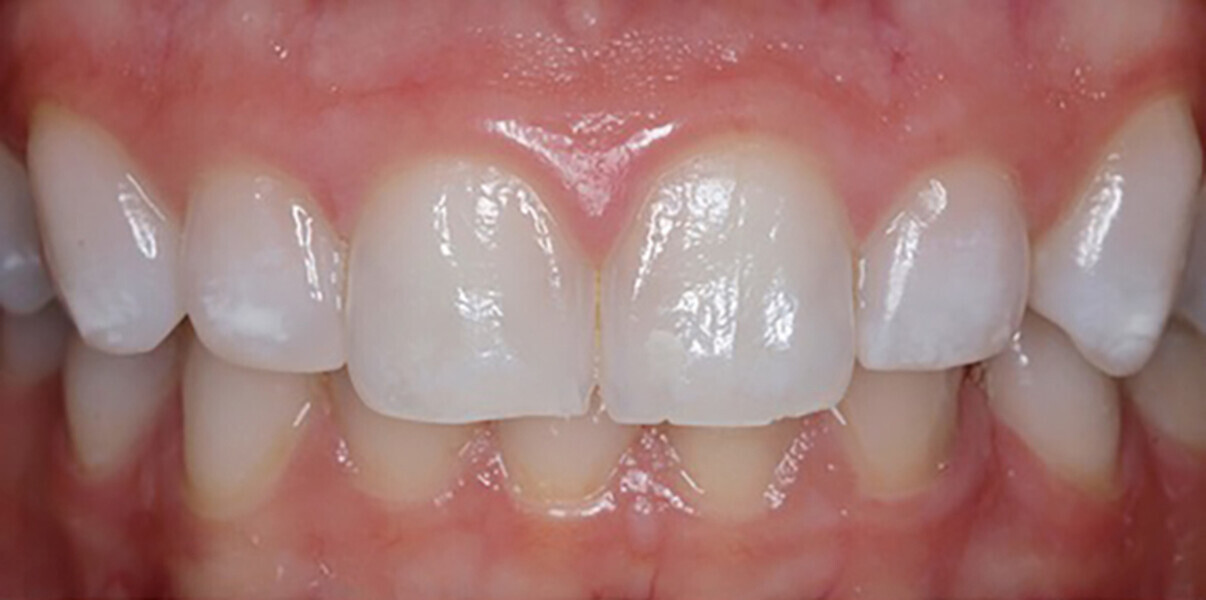
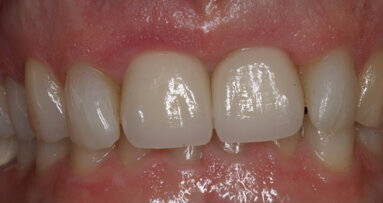
Icon-Dry (99% ethanol; DMG) was applied to and left on the surface to slowly evaporate, facilitating the elimination of water molecules located within the enamel porosities. Shade improvement was observed, but the process was repeated to further enhance the result. After the second Icon-Dry application, a substantial shade enhancement was observed clinically, and the TEGDMA-based Icon-Infiltrant (DMG) was applied to the etched and dried surfaces and periodically massaged to enhance penetration for 3 minutes. Excess material was removed with a cotton pellet and dental floss before light polymerising at a minimum intensity of 800mW/cm2 for 40 seconds. The infiltration process was then repeated with only 1 minute of application time. Finishing cups and polishing discs were utilised to smooth the surfaces (Fig. 4b). The dental dam was removed, and the patient asked to assess her outcome. She was happy with the result and the shade modification (Fig. 5a).
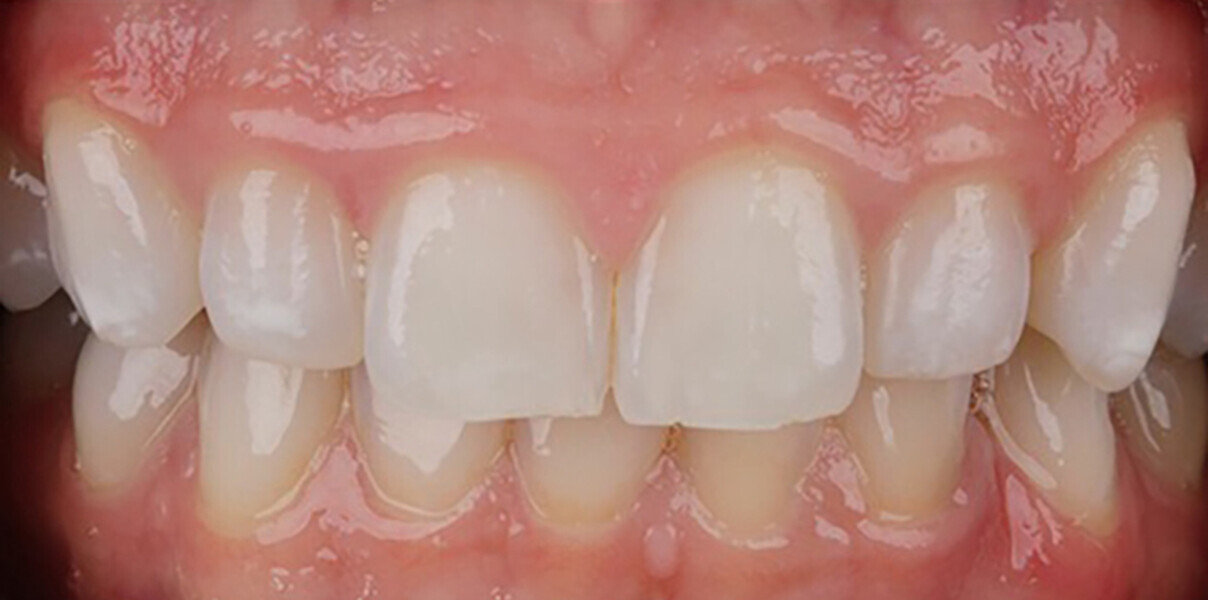
At the 14-month follow-up appointment, the patient expressed her great satisfaction with the result and agreed that no further treatment was needed (Fig. 5b).
Conclusion
Dental fluorosis is an increasingly prevalent phenomenon. According to a Centers for Disease Control and Prevention website review paper,9 the prevalence of fluorosis in 2011/2012 has doubled from 30% in 2001/2002.10 This rapid increase in fluorosis cases, accompanied by growing public awareness and aesthetic demands, requires dental care providers to be creative in offering the most conservative treatment modalities, such as tooth bleaching and resin infiltration. A combination of home bleaching and resin infiltration was used in this case to successfully resolve anterior white spot fluorosis. The 14-month follow-up indicated both colour stability and patient satisfaction.



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East











































To post a reply please login or register