Approximately one in three Americans will develop a malignancy in their lifetime.1 The chances of developing certain malignancies increase with age and several contributing risk factors such as tobacco and alcohol use. Notwithstanding significant decreases in death rates from heart disease, cerebrovascular disease and infections over the previous 50 years for many forms of cancer, death rates remain essentially unchanged during that same time period.1
Squamous cell carcinoma (SCC) is the most common malignant neoplasm affecting the head and neck. Mucosal cases account for more than 90 percent of all malignant neoplasms affecting oropharyngeal structures, with oral squamous cell carcinoma (OSCC) being the most common oral malignancy.2
Several variants of OSCC exist and histopathologic classifications for variants of OSCC include papillary, spindle cell, adenosquamous, and basaloid carcinoma; it is also possible to categorize types of OSCC based on clinical descriptors such as ulcerative, flat, polypoid and verrucoid.2 OSCC variants can have different growth patterns, ranging from small mucosal thickenings to large masses, and can appear endophytic or exophytic.
These tumors are erythematous to white to tan, frequently feeling firm on palpation. Conventional OSCC is composed of variable degrees of squamous differentiation, with well-differentiated cells closely recapitulating normal squamous epithelium but demonstrating some degree of basement membrane violation by nests of tumor cells, to poorly differentiated cells with more anaplastic-like appearances.
As a result of its complex exophytic papillary architecture, the papillary variant of SCC can be a challenge to accurately diagnose and histologic assessment of underlying invasion can be very difficult.3 Risk factors and pathogenesis for papillary SCC are unclear although human papilloma virus subtypes are thought to play a role in some cases.3
The purpose of this paper is to (a) present a rare case of papillary OSCC affecting the hard palate, and (b) describe the clinical and histologic features of this tumor in supporting the dentist’s role in early detection.
Case report
A 63-year-old female presented to the dental clinic at the Herman Ostrow School of Dentistry, University of Southern California with the chief complaint of a growth appearing on the roof of her mouth approximately two months prior to her presentation to our clinic. The patient’s past medical history included type II diabetes mellitus controlled with diet and exercise, and denial of any alcohol or tobacco use.
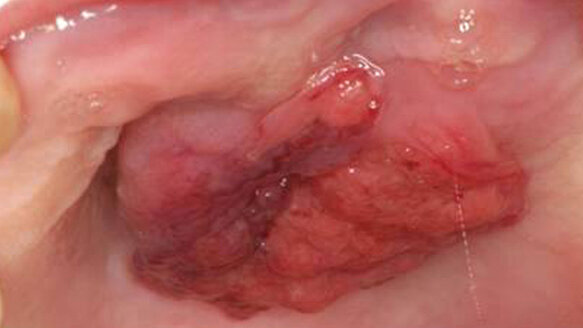
The remainder of her medical and social history was non-contributory; she was not taking any medications and a review of systems was unremarkable. Intraoral examination revealed a 3.5 cm exophytic mass in the anterior midline region of the hard palate (see Fig. 1). The lesion appeared vascularized with ill-defined borders and no evidence of ulceration or erosion.
The patient had mild sensitivity upon palpation of the lesion. No cervical or submandibular lymphadenopathy was observed during the extraoral examination of the head and neck. Panoramic radiography revealed no abnormalities of the palatal area.
The patient was informed that a biopsy must be taken to obtain a definitive diagnosis; informed consent was obtained for incisional biopsy with local anesthesia. During the administration of local anesthesia, the cortical bone under the tumor felt intact with the end of the needle. A representative wedge of tissue was removed and placed in 10 percent formalin for microscopic evaluation.
The biopsy site was cauterized to obtain postoperative hemostasis due to the high degree of vascularity. The biopsy site was closed with four 3.0 chromic gut interrupted sutures. Hemostasis was achieved, postoperative instructions were given and the patient’s postoperative condition was good.
The gross examination of the specimen consisted of a soft, tan papillary and friable mass. The histopathologic evaluation revealed an exophytic, papillary proliferation of surface mucosa showing marked maturational perturbations. It included cellular and nuclear pleomorphism, prominent nucleoli, hyperchromatism, acantholysis, increased mitotic activity and abnormal mitotic figures, dyskeratosis and keratin pearls, and increased nuclear-to-cytoplasmic ratios.
Invasive cords and islands of malignant mucosa were visualized and the associated connective tissue contained an influx of acute and chronic inflammatory cells. To evaluate whether the inflammatory infiltrates observed in the cancerous tissue were in response to superimposed fungal infection (because organisms such as Candida albicans are common oral inhabitants), periodic-acid Schiff staining was conducted and determined to be negative with appropriate staining of control tissue.
The patient was referred to the head and neck oncology group at the University of Southern California, Los Angeles County Hospital and Keck School of Medicine. Clinical work-up for staging was performed and computerized tomography scans of the head, neck and chest were determined to be negative for metastatic disease; the lesion was staged at T2N0M0.
The patient underwent tumor resection with 1 cm margins and suprahyoid neck dissection, with no radiation or chemotherapy. Her postoperative course was uneventful, and histopathologic analysis confirmed a diagnosis of papillary OSCC.
The dissected lymph nodes showed no metastatic involvement, confirming that the surgical margins were tumor free. There was no clinical evidence of recurrence at 6-months follow-up.
Discussion
The typical presentation for OSCC can be either a symptomatic or asymptomatic mucosal ulcer. These superficial ulcers often progress into symptomatic or asymptomatic exophytic or endophytic nodules with eroded or ulcerated surfaces, and can progress to direct invasion of the deeper structures resulting in a firm, non-movable mass.1
However, OSCC often begin as white or red plaques of surface mucosa, making early clinical detection possible. If a leukoplakic or erythroplakic lesion appears in the oral cavity and does not heal within a few weeks, biopsy is recommended for definitive diagnosis, which may represent levels of histologically normal tissue (e.g., keratosis) to atypia, dysplasia, carcinoma in situ or overt carcinoma.1
Papillary OSCC, such as the case presented here, is a variant of SCC as classified by the World Health Organization4 and can present as either in situ or invasive lesions.5 Male predominance exists in OSCC cases, and the sites most commonly affected in order of prevalence are the larynx, nasal cavity and oral cavity.2, 5
The clinical appearance of papillary OSCC often mimics other variants such as verrucous carcinoma, which is included in a differential diagnosis until confirmation with microscopic examination and diagnosis.3
Microscopically, OSCC can show invasive and disorganized growth with the following: dyskeratosis, keratin pearls and intercellular bridges, increased nuclear-to-cytoplasmic ratios, nuclear chromatin irregularities, prominent eosinophilic nucleoli and increased mitotic figures with atypical formation. Perineural invasion can be seen in some lesions, presenting a positive correlation to metastatic potential.1 In this case presentation, many of the aforementioned microscopic features of OSCC were evident without evidence of perineural invasion.
Early detection of OSCC, specifically stage I or II diagnosis, is usually associated with a favorable prognosis. Papillary OSCC in general has a 70 percent, five-year survival rate at any stage, and at T1 it carries a 100 percent survival rate6 compared to other variants, such as basaloid (40 percent, two-year survival), adenosquamous (55 percent, two-year survival), and spindle cell (80 percent, five-year) carcinomas.2 Most reported cases of papillary SCC exhibit a mean diameter of 1 to 1.5 cm2. Our patient presented with a relatively large lesion measuring over 3 cm in diameter.
Dentists have a critical role in early identification of and effective care during OSCC progression from premalignant lesion to malignancy.7 A study conducted to evaluate the effectiveness of dentists in the early detection, treatment and postoperative care of OSCC in a central European population revealed the following results: Dentists identified 72.5 percent of the tumors in the 608 patients they saw as malignant, while family physicians did so in only 40.11 percent of their 406 patients. This difference was statistically significant (P < .001).8
OSCC is a major public health problem that is not just limited to certain risk groups, such as those who smoke and drink as in this case report. Early detection and identification of OSCC is critical to patient treatment and survival.
embedImagecenter("Imagecenter_1_172",172, "large");
About the authors
Paul C. Lee, BA; Justin Olsen, BS; and Joshua Adcox, BS, are dental students at the Herman Ostrow School of Dentistry of USC, University of Southern California, Los Angeles. Parish P. Sedghizadeh, DDS, MS, is an assistant professor at the Herman Ostrow School of Dentistry of USC, University of Southern California, Los Angeles. For correspondence, contact Paul C. Lee, chong.lee@usc.edu.
A complete list of references is available from the publisher.
Your staff members are essential to the smooth functioning of your practice, and you rely on them to keep things going. But according to a 2014 report by ...
The greatest challenge in treatment planning is to assign a predictable accurate prognosis. In the era of evidence-based dentistry, outcome studies have ...
Henry Schein Inc. and the Global Visionary Fund (GVF) of the International College of Dentists (ICD) have once again joined together to support the oral ...
Still in the early stages of the new millennium, we are in an era of dentistry and orthodontics where more accurate diagnoses are possible thanks to ...
NEW YORK, N.Y., USA: The impact of oral disease on whole-body health and the changes to the practice of dentistry worldwide are the subjects of “The ...
Extraction versus non-extraction treatment in orthodontics has been a matter of controversy since the beginning of the specialty. Edward H. Angle debated, ...
CHICAGO, US: Dentistry is undergoing a generational and gender shift. As highlighted in The U.S. Dentist Workforce, a new report from the American Dental ...
As dentists in most countries grapple with soaring inflation, some potential buyers and sellers of dental clinics may have paused to rethink their options. ...
NEW YORK, N.Y., USA: SharperPractice specializes in distributing innovative products from around the globe that are Best in Class. For more than 20 years, ...
Abstract: This case report aims to present a clinical case in which periapical surgery with root-end filling was performed with the use of new ...
Live webinar
Wed. 10 June 2026
11:00 AM EST (New York)
Live webinar
Wed. 10 June 2026
2:00 PM EST (New York)
Nacho Fernández-Baca DDS, MSc
Live webinar
Wed. 10 June 2026
7:00 PM EST (New York)
Live webinar
Thu. 11 June 2026
1:00 PM EST (New York)
Live webinar
Thu. 11 June 2026
2:00 PM EST (New York)
Prof. Hani Ounsi DDS PhD FICD
Live webinar
Fri. 12 June 2026
8:00 AM EST (New York)
Dipl.-Hdl. Joachim Brandes
Live webinar
Mon. 15 June 2026
11:00 AM EST (New York)
Dr. Cristian Scognamiglio, Dr. Alessandro Perucchi



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East


















































To post a reply please login or register