In an interview with Dental Tribune, Dr Gy Yatros of Dental Sleep Solutions in Holmes Beach, FL, USA, discusses obstructive sleep apnea, its medical ramifications — and what dentists can do to treat the condition.
When I was scouring the exhibit floor of the Yankee Dental Congress for new and interesting dental products, I had the pleasure of meeting Rani Ben-David, who is the president of Sleep Group Solutions and featured the company’s Dental Sleep Magazine during the event.
After expressing an interest in publishing some content on dental sleep medicine, Ben-David kindly put me in touch with a Dr Gy Yatros, who is a diplomate of the American Academy of Sleep Medicine.
Dr Yatros offers a practice that endeavors to be on the cutting edge of technology, but also emphasizes the importance of dental health. Aside from the variety of services he offers, the practice motto piqued my interest: “Smile Better. Eat Better. Sleep Better … Live Better.” How many dentists had I seen promote better sleep through dentistry? Well, none until Yatros.
What is dental sleep medicine?
Dental sleep medicine is a growing area of dentistry through which dentists can help their patients sleep better and snore less, which helps their bed-time partners sleep better too.
Obstructive sleep apnea [OSA] is one of the most prevalent and increasing medical problems in the United States, and dentists who are properly trained in dental sleep medicine can help control this life threatening disease.
How can dentists help treat obstructive sleep apnea?
Obstructive sleep apnea is a condition that occurs when the airway collapses during sleep, primarily due to loss of muscle tone. When the airway collapses, it prevents air from reaching the lungs, causing a myriad of serious and undesirable health consequences. The primary muscle that contributes to this collapsing airway is the tongue.
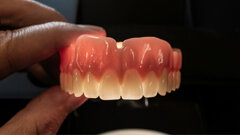
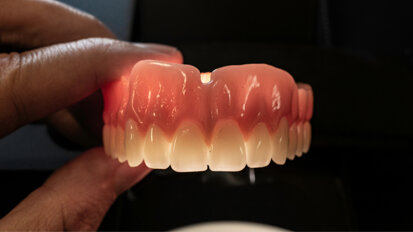
Dentists who are properly trained in dental sleep medicine make mouthpieces to hold the jaw and/or tongue forward, resulting in an increase in airway volume. There is, however, more to it than just making a mouthpiece. In our office, these dental sleep devices are custom made and adjustable.
Through our program we evaluate subjective findings and obtain objective testing with portable home sleep monitors. The results are evaluated and the devices are adjusted to obtain the maximum medical improvement for each individual.
It is more of a process than just handing someone a device. At Dental Sleep Solutions, we call the process Dental Sleep Therapy and it generally takes us one to three months to achieve the desired results.
How are the sleep devices different from snore guards?
The real question here is what is a snore guard and how do we know it is just snoring. Has the patient had a sleep study? I know there are several over-the-counter “boil and bite” products targeted at snoring prevention. In addition, I know there are dentists who claim to make “snore appliances,” but do not treat obstructive sleep apnea.
Well, I have news for them: if you are treating snoring you are likely treating OSA without a diagnosis! Snoring and OSA are caused from the same anatomic problem: a collapsing airway. Patients who snore also have an increased risk of having OSA and, furthermore, snoring is often the first sign of OSA.
Before making any type of device for snoring, I feel the patient should be evaluated for OSA with a sleep study. The majority of time we will find out it is more than snoring. Once the diagnosis is complete, then proper treatment decisions can be made. It really upsets me to see that some individuals and dentists are treating this very serious medical disorder without a proper diagnosis and follow through.
What other treatments are available?
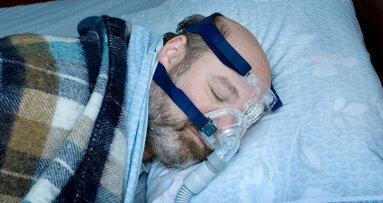
The “gold standard” for treatment of OSA has been CPAP, which stands for continuous positive airway pressure. Basically, it is a pump that is attached to a mask or nasal pillows — tubes in the nose — that increases the pressure in the airway. Much like blowing up a balloon, the pump is adjusted with enough pressure to keep the collapsing airway open.
It is the most predictable way to get air into the lungs and is a life saving device for many people. The major problem is that many people can’t tolerate its use. There are numerous common complaints with the CPAP, the most common among them are claustrophobia, GI problems, skin irritation and inconvenient use.
In addition, one of the common reasons for seeking treatment for OSA is excessive daytime sleepiness [EDS]. CPAP can help, but sometimes the CPAP itself disrupts sleep so much that the positive effects on EDS are negated by this disruption.
Other treatment options include various surgeries. Most of these surgeries are less predictable than treatment with dental sleep devices or CPAP and they are, of course, non-reversible, painful and have medical risks.
The American Academy of Sleep Medicine recommends dental sleep devices for patients with mild to moderate OSA who prefer them to CPAP and for patients with severe cases of OSA who cannot tolerate CPAP. Surgery is recommended only after the non-surgical options.
How well do dental sleep devices work?
They work very well at relieving symptoms and decreasing apnea for mild to moderate OSA. They can even work well in many severe cases, but with less predictability. A recent study by Dr Aarnoud Hoekema [Oral –Appliance Therapy in Obstructive Sleep Apnea-Hypopnea Syndrome ©2008] found that dental sleep devices were 84 per cent effective for mild to moderate OSA patients —4 per cent higher than CPAP — and 69 per cent effective for severe OSA.
Are dental sleep devices comfortable?
I guess the best answer to this is one of personal experience. I have OSA and I wear a device comfortably every night and have been for over five years. Patients generally find them much more comfortable and portable than CPAP. The compliance rates vary from around 70 to 95 per cent in studies. I have found that the vast majority of our Dental Sleep Solutions patients find them to be comfortable and wear their devices nightly.
What specialized equipment is necessary for a dentist to become involved in this kind of treatment?
The equipment necessary to successfully treat these patients for OSA is not nearly as involved and costly as it is for other areas of dentistry. I’ve often thought if I were just getting out of school that getting involved in this area would be a great way to get started. Due to the increasing need for dentists in this area and the minimal equipment costs, it can be a great profit center for little investment.
A home sleep recorder, by Embletta, and the phayrngometer/rhinometer by Ecovision are the two pieces of equipment that I feel are necessary in treating OSA with dental sleep devices. Our Embletta home recorder is a way of completing a home sleep study. This precise piece of equipment can be used for diagnosis if utilized with the help of a board certified sleep physician, and is essential to determine if our dental device is adjusted properly.
The Embletta is a little computer about the size of an iPod that is attached to the patient while he or she sleeps at night. It records many channels of information including airflow, pulse, oximitry and respiratory effort. The Embletta is then returned in the morning and we download its information into the specialized software.
This software will help us analyze the data that was obtained to see if our sleep device is adequately alleviating the apnea. Without this piece of equipment, we would not be able to tell if our devices are working properly.
The Ecovision is an apparatus that sends sound waves through the airway, giving us a volumetric reading of the airway in a graphic format on our computer screen. We can use it to measure the nasal airway, the rhinometer, or the oral airway, the phyarngometer. It is great for screening patients for airway problems, and for helping to determine the optimal jaw position for our dental devices. By manipulation of the jaw while using the Ecovision, we can more adequately predict treatment outcomes and more desirable jaw position. Both the Embletta and Rhinometer can be purchased solely through Sleep Group solutions
What special training does a dentist need to provide these services?
Dentist wanting to get involved should take an introductory course on dental sleep medicine. There are many good places to obtain education, but I recommend that they take one of our courses at Sleep Group Solutions. I feel our courses offer an excellent non-biased curriculum and they are geared toward getting the dentists started immediately.
I treat sleep patients every day in my own office and I am passionate about getting other dentists involved in this exciting area. There are other places to obtain education in this area, but some of these are sponsored by dental appliance companies. At Sleep Group Solutions we can give our students honest advice about dental sleep devices as well as practical and useful systems to get started. Dental Sleep Medicine has become a large part of my practice and I want to show other practitioners how to do it for themselves. They can go to wwwsleepseminars.com to see the upcoming schedule.
Is there a need for more dentists to become involved?
Are you kidding? Absolutely yes. Because of the lack of available dentists with knowledge of dental sleep medicine, I have been recruited by the neighboring medical community to provide care in the cities of Sarasota and Tampa.
In both of these areas, I was recruited by sleep physicians to help treat their patients because there was no other trained dentist in the area. We now have three offices at Dental Sleep Solutions to help with the demand. The prevalence of OSA and snoring is overwhelming and there are very few dentists available to help.
How did you get involved in providing this service?
Much like most of my life: a little luck and a little perseverance. Nine or so years ago, I had a patient of record who needed a dental sleep device, which was prescribed by her physician. I didn’t know much about it at the time, but I started learning.
The more I learned the more I realized the need for help in this area and the enjoyment that you can get from treating these patients. Once I became more educated in the area, I realized that I too had OSA. Of course, this increased my interest in the subject as well. The more I learned about and treated this life threatening disorder, the more passionate I became. Now it is the primary focus of my practice and I love it.
What do you like about providing this service?
That could be a lengthy answer. There are a great many things that I find enjoyable about treating OSA in my practice. I guess the most impressive is the fact that I am now providing a service that is not only dramatically improving peoples lives, I am actually helping to save them. Not many dentists can say that.
In my restorative practice, I have completed some fairly comprehensive rehabilitative cases. After months and even years of work, I have received many gratifying thanks from happy patients.
The amazing thing about treating OSA patients is that in a matter of a few weeks, I commonly receive more heart-felt gratitude from patients then I do after months or years of restorative treatment.
I routinely receive tearful embraces of appreciation from these desperate patients. Talk about going home at night feeling good!
In addition, dental sleep medicine has far less physical or mental strain then restorative dentistry. I find treating sleep patients is a welcome hiatus from the mental and physical challenges of restorative dentistry. Moreover, I guess it wouldn’t be fare if I didn’t mention that it also gives the practice a nice financial boost in this down economy.
Which dental sleep device is the best?
This is often the first question that is asked at one of our Sleep Group Solutions seminars. I usually answer it by saying that it isn’t a matter of which device as much as it is about where the jaw is placed.
There are many FDA-approved devices for treatment of OSA, and they all have pros and cons and they all work. Although one may work better than another in some situations, it is mostly a question of comfort. It isn’t so much about the particular device but more about proper follow through of their dental sleep therapy.
How much does the treatment cost and does insurance pay for it?
Of course, treatment costs can range depending on the practice and the particular patient. My estimated range for dental sleep therapy would be from $2,000 to $5,000. At Dental Sleep Solutions, we are experienced at medical insurance billing.
Of course, it depends on an individual’s coverage, but we are finding that medical insurance is helping to cover the costs in most situations. {Editor’s note: In Dental Tribune Vol. 5 No. 2, there was an article on medical coding by Marianne Harper in the pages of Hygiene Tribune.}
What is the first step for a dentist to become involved?
Take a course at Sleep Group Solutions. They offer a two-day course that will get them off and running.
How does Sleep Group Solutions service help a new dentist?
Of course, the first step is through the educational courses we previously mentioned. Also, as previously stated, Sleep Group Solutions offers the two pieces of essential equipment needed to treat patients with breathing disorders.
Finally, SGS is a great resource. SGS is one of the largest companies in the sleep field and they have many contacts throughout the country. I have had great experiences working with this company. The representatives at SGS are always willing to help and will continue to support dentists new to this field with advice as well as helping with relationship building with other sleep professionals.
What is something you know now after nine years of practice that you wish someone had told you before you began practicing?
I assume you mean after nine years of practicing dental sleep medicine because I’ve been practicing dentistry for 20 years. I wish someone would have told me or influenced me to get involved in treating dental sleep patients earlier. I never knew how much I could enjoy this field.
Do you have any other pearls of dental practice wisdom you would like to share with our readers?
I have many “pearls” for dentists who are becoming involved in the treatment of sleep apnea but my “pearl” for those who aren’t is — consider doing it! I think you’ll be happy that you did!
The Web site presentation of your practice is very inviting. Do you happen to know how many of your new patients have found you via your Web site alone?
Presently we are getting one or two cases per month from the Internet, but we are completely revamping our Web site [located at www.dentalsleepsolutions.com] along with search engine optimization. We expect those numbers to explode in 2010 for Dental Sleep Solutions.
About Dr Gy Yatros
Dr Gy Yatros has been practicing since 1992 and is a diplomate of the American Academy of Dental Sleep Medicine. He is also a member in good standing of the American Dental Association, Academy of General Dentistry, American Academy of Cosmetic Dentistry, Florida Academy of Cosmetic Dentistry (Charter Member), Academy of Computerized Dentistry, Florida Dental Association, West Coast Dental Association. He teaches courses and is available for practice consultation for dentists interested in becoming involved in dental sleep medicine.
Dr Yatros may be contacted at dryatros@dentalsleepsolutions.com.
NEW YORK, NY, USA: Selenium Ltd., a biopharmaceutical company based in Lubbock, Texas, founded in 2004 out of research from Texas Tech University, is using ...
2016 marks the 45th anniversary of Planmeca. Founder and President Heikki Kyöstilä attributes the company’s success to a strong commitment ...
WAUKESHA, Wis., USA: Functionally and esthetically optimal dental restorations traditionally have been fabricated by restorative clinicians and dental ...
CHARLOTTE, N.C., US: With a heritage of more than 150 years in dentistry, Dentsply Sirona is highlighting trust as a central theme in its endodontic ...
Of the commercially available hard- and soft-tissue lasers, only the LightWalker (Fotona, San Clemente, Calif.) combines two proven wavelengths, Nd:YAG and ...
NEW YORK, N.Y., USA: Sleep dentistry is changing the way patients with sleep disorders are treated. Traditionally, sleep apnoea has been the exclusive ...
Teams are becoming increasingly important in today’s organizations. Whether they are striving to improve quality, increase efficiency or focus on ...
NEW YORK, N.Y., USA: It was approximately 11 years ago when Mic Falkel, DDS, founder of Onpharma, first recognized that the performance and inconsistency of...
NEW YORK, NY, USA: Organizers of the Greater New York Dental Meeting (GNYDM) have announced that this year’s event will feature not one but two live ...
WESTCHESTER, IL, USA: According to new research that received the Graduate Student Research Award at the 19th Annual Meeting of the American Academy of ...
Live webinar
Tue. 12 May 2026
1:00 PM EST (New York)
Live webinar
Thu. 14 May 2026
12:00 PM EST (New York)
Live webinar
Thu. 14 May 2026
2:00 PM EST (New York)
Prof. Hani Ounsi DDS PhD FICD
Live webinar
Tue. 19 May 2026
11:00 AM EST (New York)
Live webinar
Tue. 19 May 2026
1:00 PM EST (New York)
Prof. Dr. med. dent. Ivo Krejci
Live webinar
Wed. 20 May 2026
7:00 AM EST (New York)
Dr. Graham Carmichael BDSc (Hons), DClinDent (Pros), FRACDS, Dr. Robert Gottlander DDS
Live webinar
Wed. 20 May 2026
9:00 AM EST (New York)



 Austria / Österreich
Austria / Österreich
 Bosnia and Herzegovina / Босна и Херцеговина
Bosnia and Herzegovina / Босна и Херцеговина
 Bulgaria / България
Bulgaria / България
 Croatia / Hrvatska
Croatia / Hrvatska
 Czech Republic & Slovakia / Česká republika & Slovensko
Czech Republic & Slovakia / Česká republika & Slovensko
 France / France
France / France
 Germany / Deutschland
Germany / Deutschland
 Greece / ΕΛΛΑΔΑ
Greece / ΕΛΛΑΔΑ
 Hungary / Hungary
Hungary / Hungary
 Italy / Italia
Italy / Italia
 Netherlands / Nederland
Netherlands / Nederland
 Nordic / Nordic
Nordic / Nordic
 Poland / Polska
Poland / Polska
 Portugal / Portugal
Portugal / Portugal
 Romania & Moldova / România & Moldova
Romania & Moldova / România & Moldova
 Slovenia / Slovenija
Slovenia / Slovenija
 Serbia & Montenegro / Србија и Црна Гора
Serbia & Montenegro / Србија и Црна Гора
 Spain / España
Spain / España
 Switzerland / Schweiz
Switzerland / Schweiz
 Turkey / Türkiye
Turkey / Türkiye
 UK & Ireland / UK & Ireland
UK & Ireland / UK & Ireland
 International / International
International / International
 Brazil / Brasil
Brazil / Brasil
 Canada / Canada
Canada / Canada
 Latin America / Latinoamérica
Latin America / Latinoamérica
 China / 中国
China / 中国
 India / भारत गणराज्य
India / भारत गणराज्य
 Pakistan / Pākistān
Pakistan / Pākistān
 Vietnam / Việt Nam
Vietnam / Việt Nam
 ASEAN / ASEAN
ASEAN / ASEAN
 Israel / מְדִינַת יִשְׂרָאֵל
Israel / מְדִינַת יִשְׂרָאֵל
 Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
Algeria, Morocco & Tunisia / الجزائر والمغرب وتونس
 Middle East / Middle East
Middle East / Middle East






















































To post a reply please login or register